Erin McCloskey, 11, has been a regular at Seattle Children’s her entire life. First diagnosed with a rare heart defect, a genetic specialist at Seattle Children’s later discovered she had fibrodysplasia ossificans progressiva (FOP). FOP is a complex condition that turns tissue, ligaments and tendons into bone that is outside the typical skeletal structure. Eventually, a person’s joints lose their mobility and it can cause breathing, movement and eating difficulties.
In August, Erin’s mother, Suzanne, sat with her in her hospital room as she did almost every minute of every day since April. Erin’s bed was stacked with stuffed animals and cards sent from members of the online FOP community who showered her and her family with support.
Erin, who was admitted to the hospital because her airway was being constricted by her jaw bone, could not speak due to the intubation that made it possible for her to breathe. However, McCloskey was able to translate every movement her daughter made into action.
During this long stay at Seattle Children’s, McCloskey has only left her daughter’s room to run quick errands and to see her other 18 and 16-year-old children.
“I pretty much stay glued to her hip,” McCloskey said.
McCloskey said she always dreamed of a day that her daughter would not be as reliant on the hospital, and would be able to experience the freedom of a more normal childhood – a dream she hoped was about to come true. The removal of Erin’s intubation is a big step toward more mobility and normal childhood experiences.
A rare condition requires a modern approach
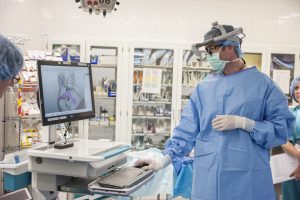
In order to allow Erin the ability to breathe on her own, doctors at Seattle Children’s would have to accomplish what other institutions had said could not be done: place a tracheotomy in Erin’s throat so that she can breathe on her own.
What may be a straightforward procedure in some patients was anything but simple for Erin. FOP had caused her to have a complicated anatomical layout in her throat and trachea that made it difficult to surgically open an airway. Other doctors had already declined trying to create a tracheotomy due to challenges caused by FOP.
Dr. Kaalan Johnson, surgical director of the aerodigestive program at Seattle Children’s, and his team decided to use a high-tech approach to Erin’s situation. To be able to successfully place the tracheotomy, Johnson and his team created a 3-D model of Erin’s throat and airway so they could practice the surgery and ensure it could be done successfully.
“We did a surgical rehearsal,” Johnson said. “Thanks to the model, we knew what things looked and felt like, as well as what tools we needed to use to achieve a successful outcome.”
The preparation for Johnson’s simulation required the work of a cross-functional team that included radiologist Dr. Jeff Otjen, site director of the radiology residency program, and Dr. Seth Friedman who worked to prepare the digital model. The team itself was supported by Seattle Children’s Imagination Lab which facilitated the design and printing of the model, including suggesting the materials for casting, and the Learning and Simulation Center (LSC) team lead by Dr. Kimberly Stone who facilitated and debriefed the simulation scenario.
The technical precision practiced on the model allowed the team to prepare for the actual surgery, which they performed immediately following the simulation. Instead of seeing Erin’s trachea for the first time in the operating room, they used the model to perfect the technique and strategy needed to make the tracheotomy successful before they even began her surgery.
Moving forward with newfound freedom
Nearly a week after the successful two-hour surgery, Erin was able to breathe on her own through the tracheostomy, alleviating her constant risk of intubation for the first time in years. With a little training and assistance of home health nurses, McCloskey plans to take her daughter home in the near future.
“We really feel that she has been given a life line with her tracheotomy,” said McCloskey. “Not having to be intubated has given her the chance to more fully experience life. She’ll be able to do things that other kids do and that’s a major step forward for us. It’s a beautiful feeling that someone listened and advocated for our child.”
For Johnson and the team who worked on Erin, it is gratifying to see their planning and practice result in a positive outcome.
“The combination of the team’s skill and the latest technology allowed us to take a uniquely challenging situation and turn it into a positive outcome for a very special child,” said Johnson.
“We’re so thankful there are doctors willing to think outside the box and not just say no,” McCloskey said. “Thank goodness for Dr. Johnson.”
Resources
Fibrodysplasia ossificans progressiva
Learning and Simulation Center

