Creativity is at the center of 11-year-old Carson Bryant’s life. “I would describe her as being imaginative,” her mother, Andrea Bryant, said. “She has a love for theater and dreams of being an illustrator someday.” In January 2018, Carson had to put her creative passions aside when she began experiencing symptoms that sparked concern for […]
Hudson Hill was born with biliary atresia, a liver condition that affects a baby’s bile ducts. At only 2 months old, Jordan Hill’s beautiful blue-eyed baby with long brown locks was in dire need of a new liver. His only hope was a donor. Below, Jordan explains the hopelessness she felt after her son was […]
For many parents, caring for a child with a serious medical condition can have its challenges. For Hailee and Ray Hughes, the challenge of caring for their 3-year-old daughter, Ruth, who has a rare gastrointestinal disorder, meant learning complicated skills like how to maintain Ruth’s nutritional needs intravenously through a tube connected to her chest. […]
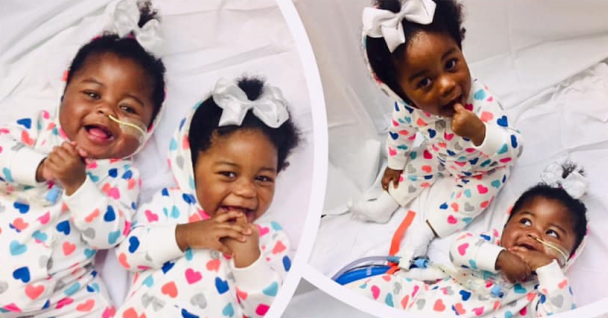
Amani Jackson and her identical twin sister, Amira, possess a rare bond that began in their mother’s womb. Up until the moment they were born, grasping on to one another, their bond remained unbroken. It wasn’t until surgeons noticed one of them wasn’t quite like the other, that they needed to part ways. “Although they […]
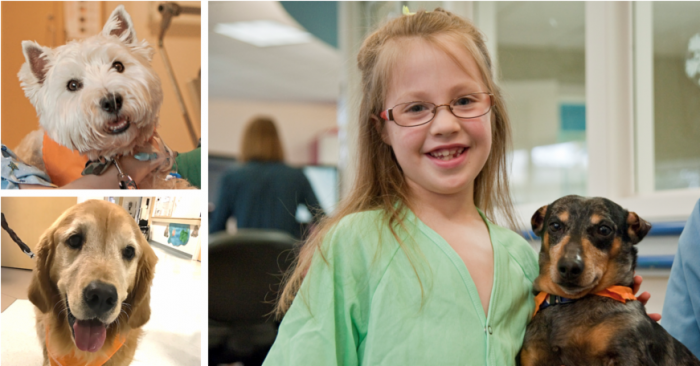
In honor of National Dog Day, On the Pulse is recognizing three unique four-legged visitors who bring joy to kids at Seattle Children’s. When a child is in need of some cheering up during a hospital stay, Seattle Children’s knows just the right MVP for the task – Most Valuable Pup that is. With their […]
It’s not uncommon for kids to complain of abdominal pain around the start of the school year, before a big test, sports game or performance — when their stress and anxiety levels can be at an all-time high. While this may not be a cause for immediate concern for some parents, others may feel uncertain […]
Claire and Emma Brennan are 13-year-olds who are always on-the-run. Whether it’s sprinting across the basketball court or flying to their next volleyball tournament halfway across the country, these twin sisters stop at nothing to achieve athletic excellence. “Claire and Emma have sports practice almost every day of the week,” said their mother, Cathy Brennan. […]
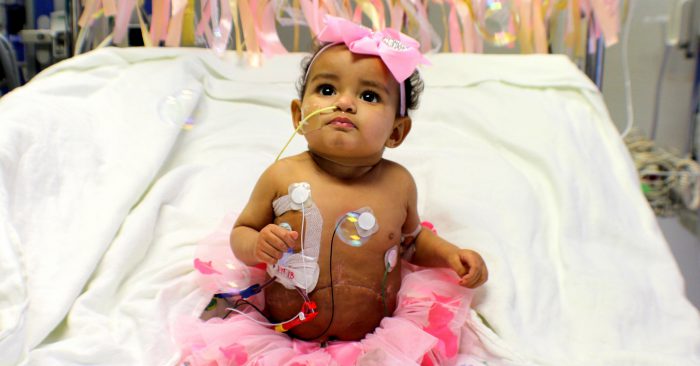
Picturing her daughter making it to her first birthday was difficult for Rachael Rowe as she watched her baby struggle to survive each passing day waiting for a liver transplant. Time officially took its toll on Feb. 6, 2018 — four months after 10-month-old Raylee was put on the transplant waiting list. “I remember it […]
With 2018 in full effect, On the Pulse is taking a moment to hit rewind to share five stories that might have floated beneath the flurry of headlines in 2017. We invite you to take a look back at some of last year’s stories that inspired us and gave us hope. 1. A Mother’s Intuition […]
It’s holiday time in the Louden household. However, this year is unlike any other. For the first time in 11 years, 17-year-old Amber Louden will be able to join her family at the Thanksgiving table and indulge in some of her favorite dishes pain-free. “I remember Thanksgiving two years ago; I ate so much food […]