It’s estimated nearly 86,000 adolescents and young adults (AYAs) will be diagnosed with cancer this year; in fact, one-third of patients treated for cancer at Seattle Children’s are AYAs. These 15- to 39-year-olds face the unique challenges of their life stage — finishing high school or college, starting a career, establishing independence, finding a romantic […]
On Sept.12, leaders from Odessa Brown Children’s Clinic (OBCC) announced the location of its new clinic site in Seattle’s Central District. The future home of OBCC, situated on the corner of 18th Ave. S. and S. Jackson St., will serve area patients and families with robust mental health and behavioral health services, nutrition, acute and […]
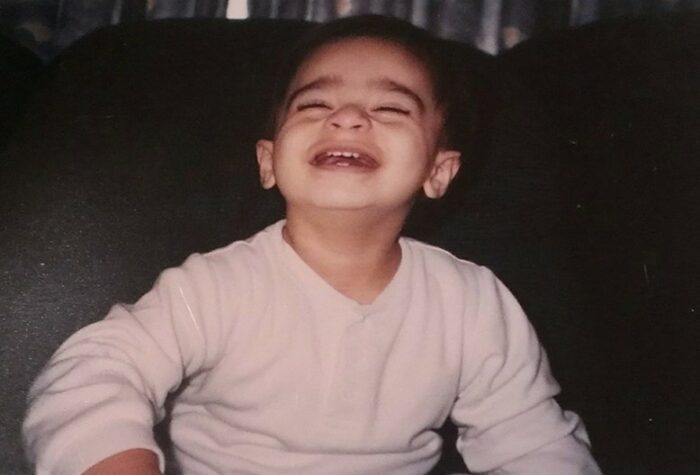
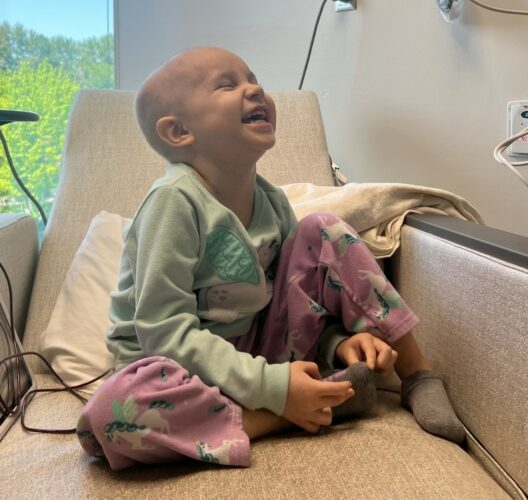
As a second-year grad student working toward a doctorate degree in the field of health sciences, Emma is as busy as ever. But for this 23-year-old, originally of Snohomish, WA, facing extraordinary challenges with determination and resilience is a skill she mastered early on. In 2017, after experiencing extreme bouts of itchiness from head to […]
Each year, Seattle Children’s Craniofacial Center treats hundreds of children with craniosynostosis, a condition most families have never heard of, yet can affect approximately 1 in every 2,500 babies in the United States. That was the case for Kali Dempsey’s family, of Camano Island, WA, in early 2017. “We were sent to Seattle Children’s when […]
Seattle Children’s providers are leaders in brain tumor care and research, offering some of the most advanced treatments, neurosurgeries and clinical trials of any children’s hospital. Its Brain Tumor Program is the largest in the Northwest and one of the largest in the world. In this edition of On the Pulse, one Seattle Children’s patient shares […]
As a part of the festivities leading up to the MLB All-Star game, hosted in Seattle on July 11, two Seattle Children’s patients, Isaac Williams and Tiago Viernes, got once-in-a-lifetime experiences thanks to MLB and MLB All-Star partners Dairy Queen (DQ) and Children’s Miracle Network Hospitals (CMN). Each year, MLB invites a guest that has […]
Seattle Children’s patients, families and staff were surprised by a pop-up performance from students in Yale University’s a cappella group, Mixed Company. The undergraduate students traveled over 2,000 miles for a series of performances in the Seattle area and made a stop at Seattle Children’s with the hope of bringing joy to those staying and […]
At just 19 years old, Faye, an avid swimmer and college freshman at Northeastern University, found her life plans on hold when she began experiencing fevers and flu-like symptoms. When her temperature reached 104 degrees, Faye called an Uber and headed to the nearest emergency department. While at Boston Medical Center, providers discovered Faye had […]
After a family trip to Finland last summer, Jasmine’s family became increasingly concerned about some unusual symptoms she was experiencing. What started as occasional numbness in her lip or left side of her face last spring had progressed to twitching, which the family later learned were increasingly strong seizures. Her family had been proactive in […]
9-year-old DeAngelo “DJ” has his dreams for the future all planned out. “DJ tells everyone that he wants to become a pediatric surgeon or a pediatric gastroenterologist one day,” explained Angela McCulloch. “He says that he plans to go to school at the University of Washington and work at Seattle Children’s to help kids like […]