More than 50 research studies to understand, detect, treat and prevent the coronavirus in children and families have launched at Seattle Children’s since the virus emerged in late 2019. The following post is part of the “Quest(ion) for Discovery” series highlighting this research in progress and the search for answers that could result in major […]
More than 50 research studies to understand, detect, treat and prevent the coronavirus in children and families have launched at Seattle Children’s since the virus emerged in late 2019. This is the first post in a new weekly series called “Quest(ion) for Discovery” highlighting this research in progress and the search for answers that could […]
Although children don’t typically fall seriously ill from the new coronavirus, doctors in Europe are now expressing concern that children with COVID-19 have developed mysterious symptoms that mimic those appearing with Kawasaki disease. On the Pulse asked Dr. Michael Portman, pediatric cardiologist and director of the Kawasaki Disease Clinic at Seattle Children’s, to help break […]
Eighteen months ago, Dr. Lynn Martin, an anesthesiologist and medical director of the ambulatory surgery center at Seattle Children’s, and his colleagues at the Seattle Children’s Bellevue Clinic and Surgery Center set out to reduce the use of opioids during outpatient pediatric surgeries, while maintaining or improving pain management and outcomes for patients. Ultimately, they […]
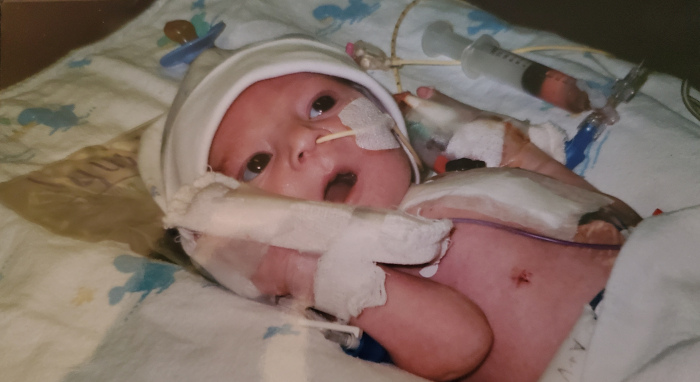
Worry flooded Candice Andrews’ mind as doctors wheeled her newborn son away for open heart surgery. “I knew about his heart condition since I was 7 months pregnant,” Andrews said. “However, it was still very scary knowing that someone was going to do surgery on my 7-day old baby.” Andrews’ son, Marcus, was born with […]
When Dr. Bonnie Ramsey entered medical school at the advice of an undergraduate professor in the early 1970s, she and her female classmates at Harvard Medical School were still among the early coteries of women to pursue careers in science and medicine. “We were the first bolus of women,” Ramsey said, using the medical term […]
Dr. Dimitri Christakis, director of the Center for Child Health, Behavior and Development at Seattle Children’s Research Institute, was featured on the TODAY Show to discuss the evolving digital age children are growing up in. Watch as three families learn more about how their children interact with devices like the iPad and hear about the challenges Christakis […]
“You pay the price for having cancer over and over again.” Mai Nguyen’s words are loaded with sorrow as she speaks about her 17-year-old daughter, Taylor Tran, who is dealing with fertility concerns more than a decade after she survived late-stage cancer. It’s easy to understand the exasperation Nguyen feels: Her daughter was diagnosed with […]
When 17-year-old Ellie Osterloh spins high above the ground from a lyra, a circular hoop used in aerial acrobatics like Cirque du Soleil, she feels empowered. “On the lyra, it’s an incredible feeling to be so high in the air with no harnessing,” Ellie said. “It’s a lot of adrenaline and I feel like I […]
Chimeric antigen receptor (CAR) T-cell immunotherapy, which reprograms a child’s white blood cells so they can seek out and destroy cancer cells, is making a difference in children’s lives. Currently, Seattle Children’s has multiple trials open that could benefit children and young adults with relapsed or refractory cancers. In October, Seattle Children’s opened a new […]