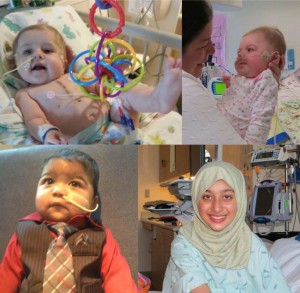
In one five-day span this September, four patients – one teenager and three critically ill infants – received life-saving heart transplants at Seattle Children’s.
For four families, the week meant the end of an agonizing wait and the start of a new life.
To perform four transplants in five days is very unusual, says Dr. Lester Permut, heart surgeon and interim chief of Cardiothoracic Surgery at Seattle Children’s. “But these are situations we train for.”
The first notification came at the end of a busy Friday: A donor heart was available for 6-month-old AJ Baird, who had spent half his short life waiting for a heart in Children’s Cardiac Intensive Care Unit (CICU).
A team from Children’s – two heart surgeons and a transplant nurse – set out immediately to get the donor heart while a team led by Dr. Permut and another heart surgeon, Dr. Michael McMullan, readied AJ at Children’s. The transplant surgery started early on Saturday, Sept. 22.
The team was finishing AJ’s surgery when the beeper went off again: a heart was available for 14-year-old Batul Al-Salami, who has been followed by the Heart Center since birth.
Then it happened again, and again, until Wednesday, Sept. 26. By then, the team had completed a total of four heart transplants – more than Children’s had ever done in a single week.
The cluster of transplants made for an exhilarating week.
“When a heart comes up for one of our patients, we’re excited about it and the energy from that sustains us,” says Dr. Permut, who traded the role of lead and assistant surgeon with Dr. McMullan for all four surgeries.
“It was a tour de force for a big group of people,” adds Dr. McMullan. “It took an incredible team and a very good system to pull this off.”
The rough road to transplant
By the time the rush of heart offers began, AJ and the two other infants – 4-month-old Hannah Campbell and 7-month-old Brooke Naab – had been in the CICU for months.
Many people – nurses, nutritionists, respiratory therapists, pharmacists, social workers, physicians and many others – had key roles in caring for the infants and helping their families.
“To get just one of these kids through a critical period is difficult,” says Dr. Harris Baden, medical director of the CICU. “But to support three babies with failing hearts through serious ups and downs for a period of months – all the while preventing serious infections that could jeopardize their candidacy for a transplant – well, it’s an amazing feat.”
 The smallest routine activity, like a diaper change or feeding, was enough to trigger a dangerously high heart rate, notes Dr. Baden.
The smallest routine activity, like a diaper change or feeding, was enough to trigger a dangerously high heart rate, notes Dr. Baden.
“These babies have no margin for error,” he says. “Caring for them takes incredible devotion, attention and respect for their fragility. All three have thrived, and that’s really a tribute to the nurses at the bedside, who took such meticulous care.”
Brooke’s parents, John and Rebekah Naab, say they witnessed heroics every day during their roller-coaster stay in the CICU. They will never forget watching Dr. Mithya Lewis-Newby, a cardiac critical care specialist, calm Brooke by leading a quiet chorus of “Take Me Out to the Ballgame” as she intubated the baby to connect her to a ventilator.
“Dr. Lewis-Newby knew that I sing that song to Brooke every night,” says John. “It just goes to show the type of people who work here – they realize they’re working with human beings, and they’re willing to pull out anything from their bag of tricks to help their patient.”
The road ahead
While AJ, Batul, Hannah and Brooke recovered in the hospital after surgery, four sets of parents received a crash course in caring for a child with a heart transplant.
Months from now, the four should be able to do the same things as other kids their age – “toddling around at home, going to school, playing sports and essentially being normal kids,” notes Pam Hopkins, a nurse and heart transplant coordinator. But, they will need daily medication and follow-up care for the rest of their lives.
“The biggest thing we tell families is that transplantation is not a cure – it’s trading one set of problems for another set that’s more manageable,” adds Dr. Erin Albers, a doctor on the Heart Failure and Transplantation team.
The medications that will keep their bodies from rejecting the transplanted hearts also make them vulnerable to infections, kidney injuries and some types of cancer. On top of that, the drugs can trigger side effects like high blood pressure and stomach problems.
But, those are manageable problems, notes Dr. Permut. “After a transplant, a patient immediately has a working heart,” he says. “It’s fairly common for children to recover enough to leave the ICU quickly, and many go home within weeks of a transplant.”
Over the course of the next year, the four will be weaned from many of the medications.
Meet the patients
Antonio Jesus (AJ) Baird
- Born: March 15, 2012
- Home: Bothell, Wash.
- Heart transplant date: Sept. 22, 2012
AJ’s mother, Yuselmi Villega Reyes, was five months’ pregnant when she went for an ultrasound, eager to learn her baby’s sex. That’s when she and AJ’s father, Antonio Baird, learned that their unborn baby had a serious heart problem: tricuspid atresia, a valve defect that prevents blood from flowing though the heart and into the lungs to pick up oxygen.
 On its own, tricuspid atresia is treatable with surgery. But shortly after he was born, AJ’s heart started showing more signs of trouble and he received a second diagnosis: left ventricular non-compaction, a heart muscle disease that can’t be fixed surgically.
On its own, tricuspid atresia is treatable with surgery. But shortly after he was born, AJ’s heart started showing more signs of trouble and he received a second diagnosis: left ventricular non-compaction, a heart muscle disease that can’t be fixed surgically.
AJ was in and out of Children’s for the first few months of his life, and in mid- May, he came back to the CICU to stay.
“For the most part, we couldn’t hold him,” says Yuselmi. A ventilator helped AJ breathe, and monitors tracked his heart rate (which was too high) and the amount of oxygen in his blood (which was too low).
Through it all, AJ’s parents marveled at the kindness and competence of the nurses who treated AJ.
“AJ would get angry, and his heart rate would shoot into the 220s for four or five hours,” says Antonio. “His nurses knew exactly how to comfort him. They know him really well.”
The first things Antonio and Yuselmi noticed after AJ’s heart transplant were his pink feet and fingers, which had always looked blue from lack of oxygen. And they did a double-take at the monitors: AJ’s heart rate – which had rarely dipped below 140 before the transplant, was a steady 117. His blood oxygen level was 100% for the first time in his life.
A week after surgery, AJ moved out of the CICU, and on Oct.12, he and his parents went home.
Batul Al-Salami
- Born: Jan 27, 1998
- Home: Lynnwood, Wash.
- Heart transplant date: Sept. 23, 2012
Batul, a cheerful high school freshman who loves to bake, was accustomed to being blue. Not sad, but literally blue from a lack of blood oxygen.
When she was born, Batul’s parents, Qassim and Madina, learned that she had a heart defect called hypoplastic left heart syndrome, which can sometimes be corrected through a series of three surgeries. That’s the path Batul started down when she was less than 1 month old.
 But, Batul’s heart function declined too rapidly to be corrected. Although medications have helped her live as normal a life as possible, as she got older she tired more easily and just getting through the days became exhausting.
But, Batul’s heart function declined too rapidly to be corrected. Although medications have helped her live as normal a life as possible, as she got older she tired more easily and just getting through the days became exhausting.
A few years ago, the Heart Center team started to talk Batul and her parents about a heart transplant, and this summer Batul agreed that it was time. “She was tired of being tired and unable to keep up with her cousins,” says Pam, the heart transplant coordinator, who has been part of Batul’s care team since she was a baby.
“For teens, it’s really important that they are involved in the decision-making process,” says Pam. “Their survival depends on taking medication and getting regular medical care for the rest of their lives – and those things require an emotional commitment from the teen.”
When Batul was listed for a transplant, she expected to settle in for a long wait. She was shocked – and very frightened – when she learned that a heart was available after a wait of less than two months.
“I was scared that it would change the way I look,” says Batul.
Afterward, that’s the first thing Qassim noticed about his daughter. “We told her, ‘you are pink instead of blue,’” he recalls. “She didn’t quite know what we were talking about.”
Batul says she likes the change – in her appearance and also in her energy. Two weeks after surgery, she was walking around Children’s with more energy than she’d had in years. By Oct. 14, she had recovered enough to go home.
“It feels like I came back from the dead,” says Batul. The thing she is most looking forward to doing, she says, is running.
Hannah Campbell
- Born: May 18, 2012
- Hometown: Everett, Wash.
- Heart transplant: Sept. 24, 2012
When she was born, Hannah was a little too listless and a little too blue. And her heart was pumping at 253 beats per minute. By that night, Hannah and her parents, Jennifer and Jon, were at Children’s.
 They went home a week later with two diagnoses: supraventricular tachycardia (a wildly fast heartbeat) and hypertrophic cardiomyopathy (a thickening of the heart muscle that can cause dangerous rhythm problems).
They went home a week later with two diagnoses: supraventricular tachycardia (a wildly fast heartbeat) and hypertrophic cardiomyopathy (a thickening of the heart muscle that can cause dangerous rhythm problems).
Twelve days later, Hannah’s heart had doubled in size – and she was back at Children’s.
For her parents and two older brothers, Hannah’s stay on the CICU was a cycle of heartbreak and hope.
Four times, she was so sick that Jennifer and Jon prepared to say goodbye to their infant daughter. She had a pacemaker implanted, but it failed to steady her heartbeat.
When she went on ECMO – a machine that does the work of heart and lungs – Hannah went into cardiac arrest. It took two hours of CPR for her heart to stabilize enough to be connected to the machine.
“The doctors didn’t think she’d get off ECMO without a new heart, but her lungs were too sick to list her for transplant,” recalls Jennifer.
To everyone’s relief, Hannah’s lungs and hearts started to improve after three weeks on ECMO, and when she was disconnected from the machine she was added to the transplant list.
By the time Hannah’s new heart came, her own heart had expanded to the size of an orange, in contrast to the walnut-sized heart of a typical infant.
While Hannah was in surgery on Sept. 24, Jon and Jennifer tuned into the Seahawks vs. Packers football game to distract themselves – and to watch for their son, Cavan, who was celebrating his 9th birthday at the game.
Just as Golden Tate scored a controversial touchdown at Century Link Field, they got the message that for the first time their daughter had a healthy heart pumping blood through her body.
The Campbells’ joy at their daughter’s fortune is muted by their sadness for the family of the heart donor.
“This family, whoever and wherever they are, lost a child and they’re grieving,” says Jennifer. “To give part of the person they’ve lost to save another child – that’s absolutely amazing to me.”
Brooke Naab
- Born: Feb. 11, 2012
- Hometown: Mukilteo, Wash.
- Heart transplant: Sept. 26, 2012
Brooke was 7-days-old when she came to Children’s with breathing trouble. She was diagnosed with a type of interrupted aortic arch, a rare heart defect that prevents the heart from pumping blood to the lower body.
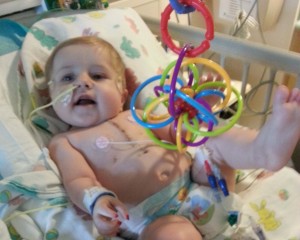 She had her first surgery before she was 2 weeks old, and she recovered well enough to go home after a month. Soon, however, her skin turned a tell-tale shade of blue, a sign that her blood wasn’t getting enough oxygen.
She had her first surgery before she was 2 weeks old, and she recovered well enough to go home after a month. Soon, however, her skin turned a tell-tale shade of blue, a sign that her blood wasn’t getting enough oxygen.
Brooke was getting sicker.
In June, Brooke returned to Children’s, where she shared a hospital room (dubbed by nurses “the princess room”) with Hannah. In the princess room, the families quickly discovered the many things they had in common: they live five minutes from each other; both dads – Jon and John – coach baseball teams; and they share a deep religious faith.
The families had no way of knowing, then, that their daughters would both be listed for heart transplants, or that they would receive them within days of each other. They have supported each other throughout the journey, and they see a long future friendship for Hannah and Brooke.
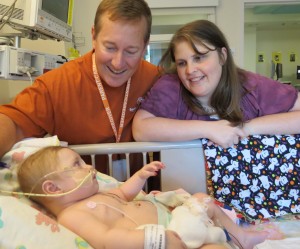 “Oh, my goodness, we were so happy for Hannah when she got her heart,” says Rebekah.
“Oh, my goodness, we were so happy for Hannah when she got her heart,” says Rebekah.
Less than a day later, the Naabs learned that Brooke would also receive a heart.
“It was a complete surprise,” says John. “And there are always mixed emotions, because you know another family has lost a loved one.”
Since the transplant, Brooke has quickly gained strength.
When he thinks about the team at Children’s that gave his daughter a shot at life, John sees a cast of hundreds – not just the surgeons who transplanted her heart or the doctors and nurses who sustained her on the CICU.
“Everyone from medical assistants to sonographers to social workers, nutritionists –even the people who keep the hospital clean,” says John. “Every role is critical to getting these hurting children back to health.”
John sums up what he saw at Children’s with a quote from John Wooden, the hall-of-fame UCLA basketball coach: “The star of the team is the team.”
Still waiting
The team at Children’s has performed 107 heart transplants, an average of 10 to 12 each year.
But more children are always waiting for hearts.
Today, six Children’s patients are listed on the heart transplant list, including one infant who has been waiting for months in the CICU.
It is highly unusual for four transplants to happen in five days. According to the U.S. Department of Health and Human Services, in 2011 only 373 children ages 17 or younger received heart transplants across the entire U.S. 110 of the 373 were under the age of 1.
Learn more about organ donation and find out how to become an organ donor.
Additional information
- Hi-resolution photo gallery: http://www.flickr.com/photos/38997016@N03/sets/72157631970647216/
- Captions for photos above:
- Heart transplant recipients (clockwise, from top left): Brooke Naab, Hannah Campbell, Batul Al-Salami and AJ Baird.
- AJ Baird after his heart transplant at 6-months-old.
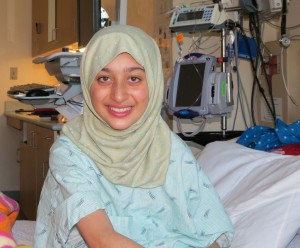
- 14-year-old Batul Al-Salami after her heart transplant.
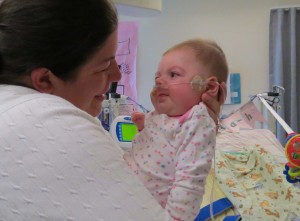
- Hannah Campbell after her heart transplant at 4-months-old with mom Jennifer.
- Brooke Naab after her heart transplant at 7-months-old.
- Brooke Naab with her parents John and Rebekah after her heart transplant.

