
In February 2010, Jennica Clasby knew something was wrong when her 3-year-old daughter, Brooklyn, said she needed to sit down because her “heart hurt.”
“I thought it was really odd to hear that coming from a 3-year-old,” Clasby said. “I sat her down on my lap, put my hand over her heart and I was terrified to feel that it was practically pounding out of her chest.”
Clasby and her husband Brandon, who lived in Colorado, rushed Brooklyn to the emergency room where they were shocked to learn she was in heart failure. Brooklyn was diagnosed with pulmonary hypertension (PH), or high blood pressure in the lungs. PH is a chronic condition that occurs when the muscle in the wall of the blood vessels and arteries in the lungs thickens and cannot properly expand to receive blood coming from the heart. This causes resistance to the heart, which then works harder to pump the blue blood in need of oxygenation into the lungs. Over time, the strain on the heart can cause it to fail.
“Our world was turned upside down,” Clasby said. “It’s incredibly hard to hear that your daughter has an incurable, lifelong disease that will progressively get worse. It changed the way we lived and gave us a new appreciation for life.”
For Brooklyn and her family, the next few years were full of daily procedures, numerous medicines and regular check-ups to manage her condition. That was, until they found a solution in an old surgical tool called a Potts shunt that’s been repurposed to give hope to people with PH.
An answer is found in something old, something new, something borrowed and something blue
In 2012, under the advisement of Brooklyn’s doctor, the Clasby family moved to Seattle to be at sea level, which helps relieve pressure in the lungs. They picked Seattle because the mountains reminded them of home, and because they wanted Brooklyn to see a leading PH specialist at Seattle Children’s Pulmonary Hypertension Clinic – Dr. Delphine Yung, a pediatric cardiologist who is also a part of Seattle Children’s Heart Center team.
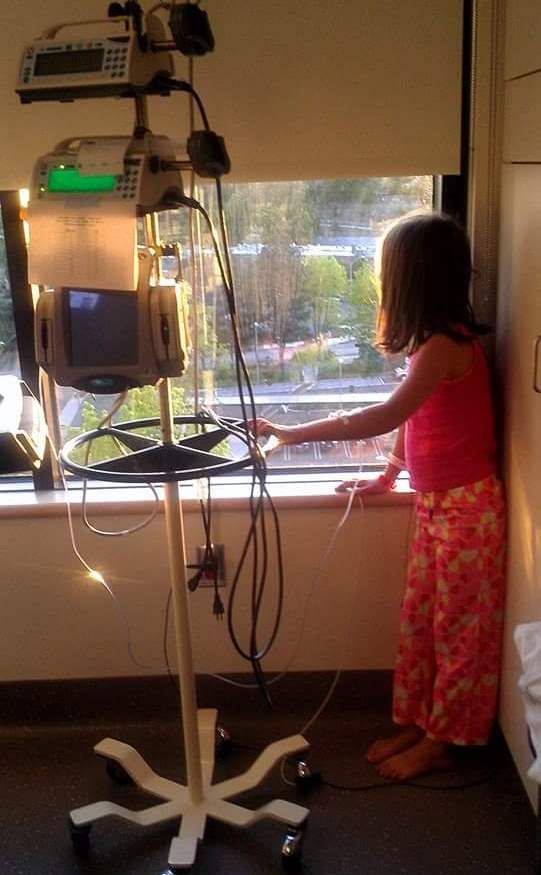 At first, Brooklyn’s condition improved, but over the years, her health rapidly declined.
At first, Brooklyn’s condition improved, but over the years, her health rapidly declined.
“At 8 years old she was maxed out on her medications, she wasn’t growing and she couldn’t walk 10 feet without being short of breath,” Clasby said. “It was terrible watching her constantly fight for air.”
It was at that point the Clasby’s began to consider their last option – a lung transplant, which can improve a child’s quality of life but is not a cure and carries a risk of a 50% mortality rate. However, with Brooklyn’s condition deteriorating, transplant seemed out of reach as obstacles like insurance coverage and coordinating travel to another center delayed the process. That’s when Yung presented them with another option that involved revolutionizing the once failed Potts shunt to use it in a new way.
The Potts shunt was first created in the 1940s to help get blood from the heart to the lungs, but the shunt overwhelmed the lungs with blood so it soon fell out commission for several decades. That was, until doctors in France had the idea to repurpose the shunt for PH patients and reverse its use, redirecting excess blood in the pulmonary artery to the aorta in the heart.
“I had heard of a few PH cases abroad and later in the U.S. where the Potts shunt was used successfully and I felt it could hold a lot of potential for Brooklyn,” Yung said. “In PH, it’s like your pulmonary artery from your heart is a hose with a kink in it. The heart is the pump that works harder to push the blue blood through the kink with no success. But with the shunt in place, we can give the blood an alternate path through a new piece of hose to relieve the pressure.”
That is when Yung took the idea to Brooklyn’s cardiac surgeon, Dr. Jonathan Chen, who is chief of pediatric cardiovascular surgery and co-director of Seattle Children’s Heart Center.
“Surgery can be very complex for these patients given how sick they are, but after researching the revised use of the shunt, I felt that it was worth going out on a limb to do all we could to try to improve Brooklyn’s life,” Chen said.
Chen and Yung approached Clasby and her husband with the idea, and while they felt nervous that Brooklyn would be the first patient at Seattle Children’s and one of only a few in the world to try this approach, they felt relieved to have another option.
“While it was scary, having another possible solution in sight was an answer to our prayers,” Clasby said.

On Sept. 11, 2014, Chen performed the surgery to implant the shunt. The surgery went smoothly. Brooklyn’s heart finally had some relief.
After a few weeks of recovery, Brooklyn no longer needed supplemental oxygen and she was able to get her central line catheter removed, which delivered a medication she no longer needed. A major milestone as it meant she could go swimming for the first time in her life. Yung was sure she didn’t miss the remarkable moment.
“It was wonderful to see her swim for the very first time,” Yung said. “It signified the beginning of a new life for her where she could start to really enjoy being a kid.”
Chen added, “I was in awe of the incredible courage of her parents to try the shunt and it was amazing how well this repurposed approach quickly transformed her life,” Chen said. “I also couldn’t help but think that as a wedding is the mark of a new life, so was this procedure, and for Brooklyn the shunt was her something old, something new, something borrowed and something blue.”
Potts shunt allows Brooklyn to not miss a beat of childhood

Today, Brooklyn is 10 years old and thriving.
“The shunt led to a drastic improvement in her quality of life,” Clasby said. “She went from not being able to walk from the car into the grocery store, to running with friends and playing sports like volleyball and softball. She has found renewed confidence and an excitement for life that she didn’t have before.”
As for the future, doctors don’t fully know what to expect with the shunt since it’s so new, but Clasby is thankful for the life it has given her.
“We don’t fully know what to expect, but we’re so thankful because we’re confident she wouldn’t be here with us today if she didn’t get the shunt,” Clasby said. “She wouldn’t have experienced all the incredible things she has over the last few years – all the joys of just being a kid.”
Yung and Chen have implanted a Potts shunt in one other patient who had a similar positive outcome. Now seeing two successful cases, they are optimistic about the promise the shunt may hold.
“We’re thrilled that the Potts shunt is another step in the right direction as we continue to work toward finding a cure for pulmonary hypertension,” Yung said. “It’s a step that potentially provides families with an option aside from transplant and gives them hope that their child’s quality of life can improve.”
Resources:
- Seattle Children’s Pulmonary Hypertension Clinic
- Seattle Children’s Heart Center

