Rachael and her husband had saved for years to buy their first home, where they hoped to settle and raise their family. With a two-year-old boy and a baby on the way, they excitedly made an offer on a house in Bellingham and scheduled an appointment to sign the last of the papers. While they […]
On the Pulse
Seattle Children’s welcomes Laura Knapp as its new vice president of Mental and Behavioral Health. An innovator, collaborator and optimist, Knapp leads Seattle Children’s mental and behavioral health strategy. She is responsible for the organization’s efforts to meet the recent increased demand for services and develop strategies for long-term growth and expansion. In her 20-year […]
Attention Deficit Hyperactivity Disorder (ADHD) is one of the most common neurodevelopmental disorders that affect children. While patients may first be diagnosed in childhood, ADHD often persists and can be diagnosed at any age. Management of the condition varies as symptoms manifest differently through various milestones in a person’s life. Common ADHD symptoms include trouble […]
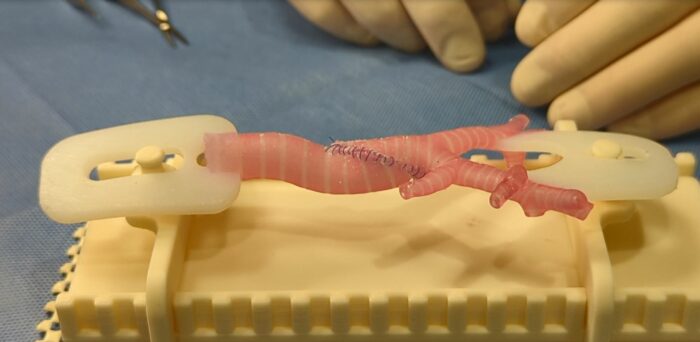
Seattle Children’s Doctors Use 3D Printing to Help Train International Care Teams on Complex Surgery
Healthcare organizations are increasingly looking to incorporate the use of 3D-printed models to help improve outcomes for pediatric patients in need of very complex surgeries. Doctors at Seattle Children’s are now utilizing 3-D printed models created in the hospital’s Innovation Lab to train international care teams in a highly specialized procedure, known as a slide […]
Hundreds gathered in Seattle’s Central District neighborhood to celebrate the Odessa Brown Children’s Clinic’s (OBCC) future location on 18th Ave. S. and S. Jackson St. at a community homecoming event to learn about the services that will be provided, meet their neighbors, enjoy food from local vendors and celebrate the day with family-fun activities.
On Saturday, October 28, Seattle Children’s honored Wizards of the Coast for their $5M commitment to Seattle Children’s Magnuson by naming the Autism Center registration area and main waiting room. The celebration included a ribbon-cutting and tours of Magnuson, which opened last year and was fully funded by philanthropy.
During a regular 12-week prenatal visit, Mollee Lewallen’s obstetrics appointment went from routine to worrying in a matter of seconds. “We found out that our son, Knox, had an extremely high heart rate,” she explained. “After that appointment, we went to a follow up where his high heart rates continued, so we were recommended to […]
You may have heard about a respiratory infection that hit babies and young children particularly hard last year, sometimes resulting in hospital stays. The infection was RSV, which is short for respiratory syncytial virus. As RSV season arrives this year, Dr. Tony Woodward, medical director of emergency medicine at Seattle Children’s, shares information to help […]
Stage was born three weeks premature and soon began having seizures. He was diagnosed with mitochondrial myopathy, a life-threatening diagnosis with no cure and which causes significant muscular and neurological problems. For Stage and his family, it meant unexpected, lifelong care. “I was naïve enough to think that insurance covered everything if your kid was […]
Almost all parents and caregivers are familiar with bullying that happens in person. But fewer adults understand cyberbullying. It refers to bullying that happens in the digital world via devices like smartphones, computers and gaming systems. A type of harassment, cyberbullying includes sending messages meant to intimidate, humiliate, manipulate or cause other distress. Cyberbullying can […]