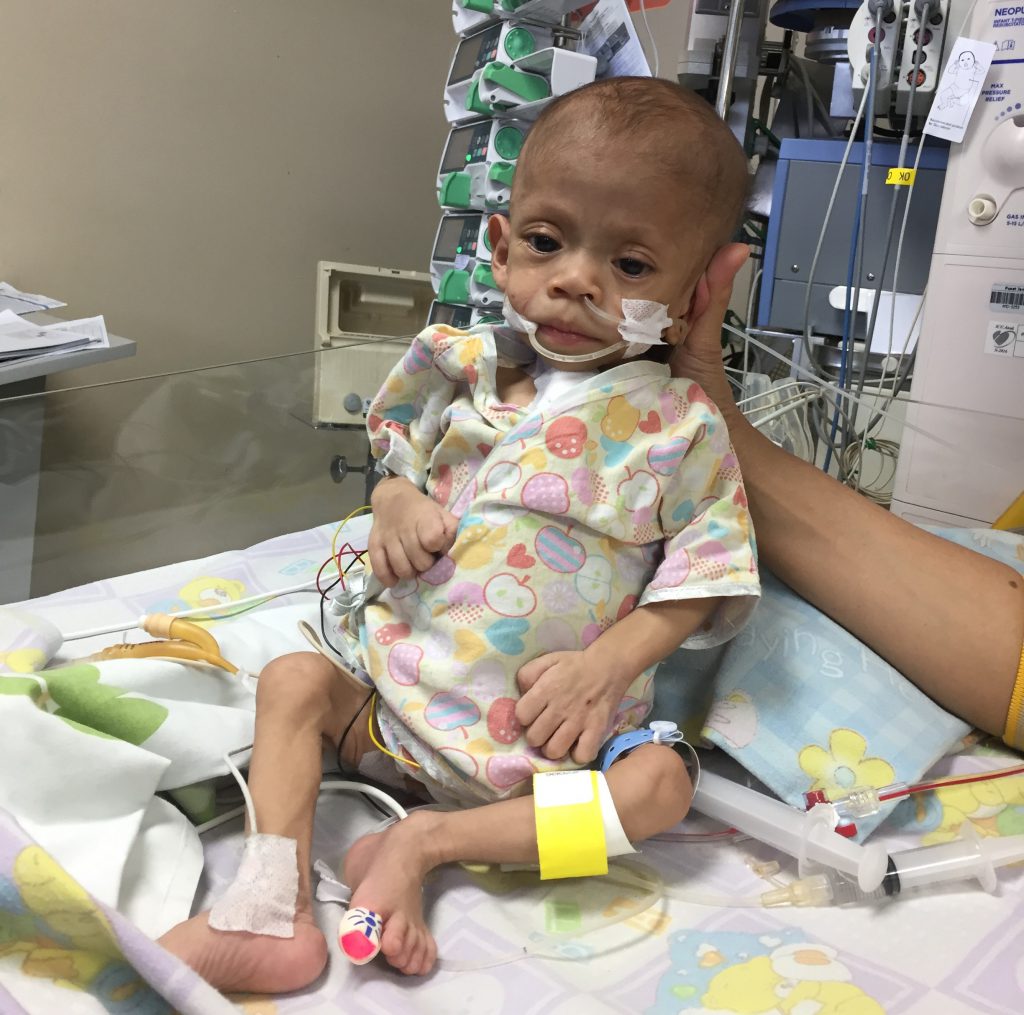
Babies who need heart surgery in the U.S. have access to advanced healthcare and doctors that get them into the operating room quickly, allowing them to fix problems early and give the babies a chance at healthy growth.
But in developing countries, babies wait longer for surgery for a variety of reasons: Fewer qualified doctors, late diagnoses of heart conditions, and capacity issues at hospitals that cannot accommodate all the infants who need surgery. As a result, babies with heart conditions in developing regions of the world are often sicker and weaker when they finally have surgery.
Dr. Eva Marwali, a pediatric cardiac intensivist at the National Cardiovascular Center Harapan Kita in Jakarta, Indonesia sees this happen to babies in her country. She teamed up with Dr. Michael Portman, a cardiologist at Seattle Children’s Research Institute, and in a study out in the Annals of Thoracic surgery, they identified an easy, economical way to speed recovery for babies at her hospital who need lifesaving heart surgery.
A simple, cheap hormone
Marwali and Portman found that giving babies 5 months or younger thyroid hormone during surgery and recovery reduces the time babies spend on ventilators in the intensive care unit after surgery. That simple change to treatment not only speeds the baby’s recovery time, but it also frees up ICU space and allows more babies to get surgery more quickly.
“The most exciting part of this work is that the thyroid hormone is very cheap and accessible, so we’re hopeful that this same technique could be applied easily in other regions of the world that face similar challenges,” Marwali said.
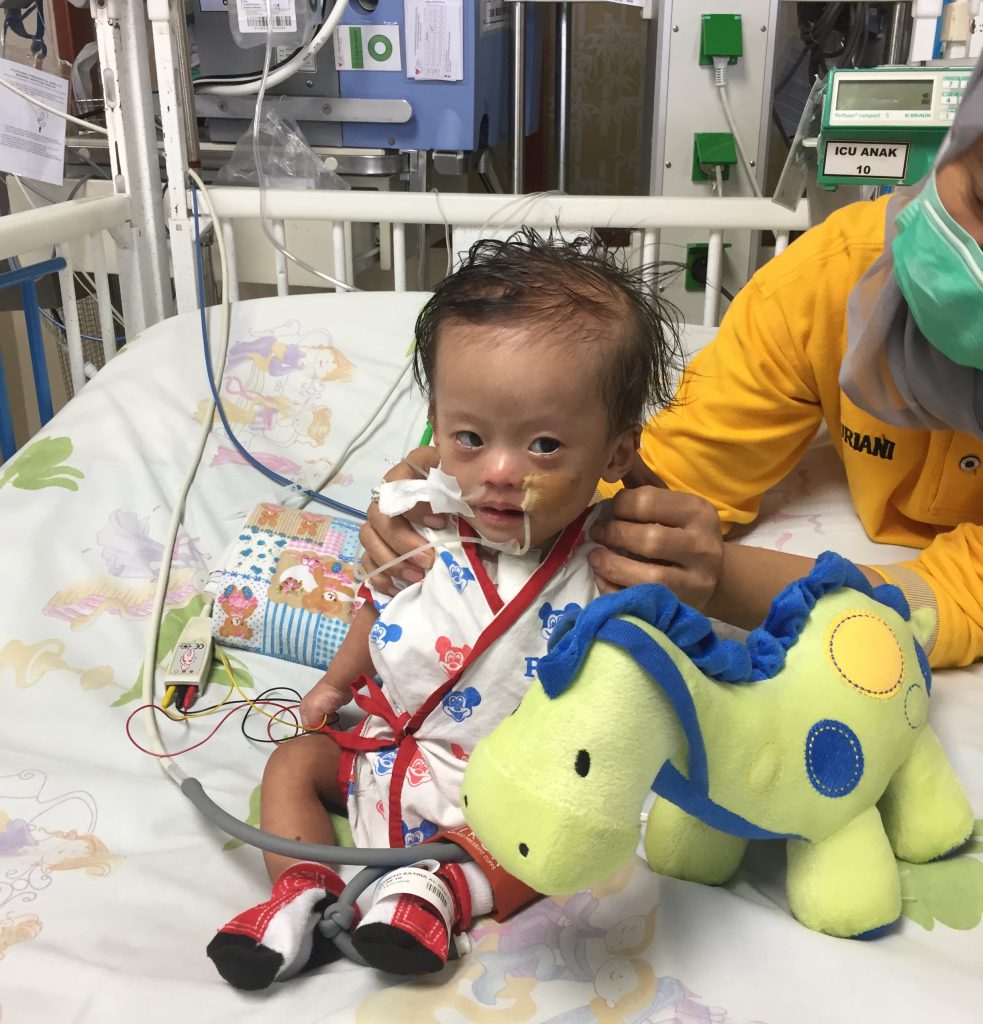
In developing countries, heart defects in a baby may not be evident right away due to healthcare access issues, and the babies often become sick and malnourished as a result of an undiagnosed heart condition. Once diagnosed, the babies often face a long wait for surgery to correct the problem. The babies also experience malnutrition due to being sick and trouble with feeding, so they have more severe drops of thyroid hormone than a baby who has a healthy weight.
Heart surgery causes stress on a baby’s chest and lungs, so babies recovering from surgery are placed on ventilators, often for days, to help them breathe and give their bodies time to recover. The thyroid hormone stimulates the heart and helps the body get rid of fluids, which speeds recovery.
“Thyroid hormone levels drop during heart surgery, so we replenished a hormone that helps the body shed fluids and stimulates cardiac function,” Portman, who has a similar study in progress for babies in the U.S., said. “There is a lot of fluid in the lungs after surgery and heart function is depressed, which together explain why the babies have to be put on a ventilator. By giving them hormone during and after surgery, we speed up recovery so they can get off the ventilator.”
Adding the hormone got babies off the ventilators an average of 15 hours faster, which when compounded, could result in significantly more space for other babies in need of surgery.
A need for heart surgery access
More than 40,000 babies are born with congenital heart defects each year in Indonesia, and 10% of infant deaths in the country are a result of congenital heart defects.
“Almost half of congenital heart defect cases require intervention and surgery,” Marwali said. “I estimate about 18,000 children born in Indonesia require surgery and need treatment in a cardiac center with adequate facilities.”
Hospitals in developing parts of the world do not have enough surgeons or facilities to care for the volume of patients they have.
“In Indonesia, the entire ICU area where all babies recover after surgery might only be as big as a single ICU room in the U.S.,” Portman said. “The staff work very hard with what they have, but they don’t have the same facilities and equipment we do in the U.S. If they can get babies off the ventilators safely and more quickly, they can use that valuable space for another baby in need.”
Children’s heart health collaboration across the globe

Marwali and Portman’s ongoing collaboration has resulted in this informative research, and it has given them both the opportunity to see each other’s experience in healthcare. Marwali has visited Seattle Children’s, and Portman toured her hospital in Indonesia and served on the academic board for her PhD degree.
The research milestone has special meaning for Marwali, who was inspired to become a physician thanks to her late father, himself a doctor and professor who encouraged her to pursue medical and scientific work in Indonesia.
“I see how the dire condition of a baby can be changed from severe to healthy thanks to the work we do,” Marwali said. “With this economical, easy solution, we are able to help these babies become healthy kids whose development after surgery will be vastly improved.”
Resources
- Annals of Thoracic Surgery: Oral Triiodothyronine for Infants and Children Undergoing Cardiopulmonary Bypass
- Dr. Eva Marwali, National Cardiovascular Center, Jakarta
- Dr. Michael Portman, Seattle Children’s
- Heart Center, Seattle Children’s

