 Carolina Castañeda and Jesus Farias were driving home from a family outing with Olivia, their newborn daughter, when they heard her making a strange noise. As first-time parents, they thought it might be normal. However, when Olivia continued making the sound, the couple began to worry. They stopped the car, took Olivia out of the car seat, and noticed that her body had gone limp.
Carolina Castañeda and Jesus Farias were driving home from a family outing with Olivia, their newborn daughter, when they heard her making a strange noise. As first-time parents, they thought it might be normal. However, when Olivia continued making the sound, the couple began to worry. They stopped the car, took Olivia out of the car seat, and noticed that her body had gone limp.
“Her hands and legs just stopped moving,” said Castañeda. “I didn’t know what was normal, but it did not look normal at all.”
Castañeda was startled to see Olivia’s blue lips and her eyes rolling back. The couple rushed their daughter to the nearest hospital in Yakima, trying to keep her awake. When they arrived, Olivia’s eyes were closed.
“Nurses ran around the desk and took her out of my arms – they didn’t even ask questions,” said Castañeda. “It all happened so fast.”
Doctors told the family that Olivia’s body had worked so hard to stay alive that her vessels were shutting down. When Olivia finally opened her eyes and looked around, Castañeda said she remembers feeling at peace, like everything was going to be okay.
The hospital flew Olivia to Seattle Children’s from the Yakima airport. The family was told that a helicopter would have been too slow for Olivia, in her condition.
The new parents were shocked to learn that their 2-week-old baby was in cardiogenic shock due to critical congenital heart defects and she would need surgery from Seattle Children’s Heart Center.
“Everything was scary,” said Castañeda. “She was my baby, she was my firstborn.”
Severe symptoms
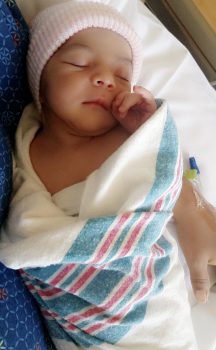
Olivia arrived at Seattle Children’s in an extreme state, with low blood pressure and significant difficulty breathing due to respiratory failure. She needed an intravenous line and a breathing tube for resuscitation. Olivia’s heart was enlarged, prompting an echocardiogram that showed it was functioning poorly. Her liver, lungs and kidney were significantly affected, and she had acid in her blood.
Shortly after undergoing further testing, the family learned that Olivia had coarctation of the aorta, or extreme aortic narrowing. This condition develops before birth and makes the aorta, the main blood vessel that comes from the heart and supplies blood to the entire body, constricted so that it is shaped like an hourglass. Blood pressure increases above the narrow spot, placing strain on the heart, which starts to fail.
While coarctation of the aorta can be diagnosed prenatally, a significant coarctation that is undiagnosed at birth leads to inadequate blood flow to the lower half of the body, which means that the liver, kidney and gut suffer. The heart tends to function poorly, since it has to work against more resistance to get blood to the lower body.
Olivia also had a small aortic arch, which further restricted the flow of blood to the organs below her chest.
Further adding to her condition, Olivia was born with a muscular ventricular septal defect (VSD), a hole in the wall of the heart between the two lower chambers where the blood leaves the heart. Normally, blood cannot pass between the left and right ventricles. But when there is a hole between the sides of the heart, some oxygen-rich blood leaks from the left ventricle into the right ventricle and goes back to the lungs. The hole causes the heart to work harder to pump blood to the body and leads to additional blood flow to the lungs. As a result of the extra work, the heart can get bigger.
Repairing the heart by stopping it
Doctors needed to wait until Olivia was in a more stable condition before attempting to repair her heart. In the ICU, Olivia was given a medicine called prostaglandin to open up the ductus arteriosus, the blood vessel between the pulmonary artery and aorta, to bypass the obstruction in her aorta. Then, Olivia needed a ventilator to help her breathe and additional medicine to support the heart and other organs.
Within five days, Olivia’s condition improved, and the Heart Center team moved forward with surgery to reconstruct the aortic arch and treat the aortic coarctation.
“It is rare to see a child as sick as Olivia was, but the ICU team successfully resuscitated her and got her to surgery,” said Dr. Muhammad Nuri, a cardiac surgeon at Seattle Children’s who performed surgery on Olivia. “In order to access and repair the aortic arch, we stop the function of the heart and the lungs while continuing to supply blood to the rest of the body with a technique known as cardiopulmonary bypass. That’s why we need some recovery beforehand, because it can be especially taxing on those organs.”
The team widened the aortic arch using a piece of Olivia’s pericardium, the membrane that covers the heart. Her aortic coarctation was repaired by cutting above and below the narrow part of the aorta, removing it and bringing the two parts together.
Recovery
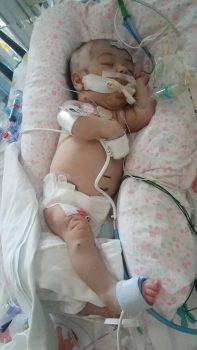
After the successful surgery, Olivia’s parents were flooded with relief.
“I remember giving Dr. Nuri a hug, because I felt like he was giving me my daughter back,” said Castañeda. “We felt so blessed and thankful.”
During the arch repair, the team found that Olivia’s VSD was inaccessible and located at the apex of the heart. They put a band across the pulmonary artery, which constricts the flow through the lung artery and reduces the effect of excessive blood flow to the lungs. In six months, they planned to remove the band and repair the VSD.
Three weeks after surgery, Olivia went home with a recovered heart.
Olivia’s family returned to Seattle Children’s in February 2018 to remove the band and repair the pulmonary artery. Doctors found that her VSD had closed spontaneously and did not need further repair. Four days after an open-heart surgery to remove the band and repair her pulmonary artery, Olivia returned home.
It is recommended that all children who undergo cardiopulmonary bypass under 1 year of age have neurodevelopmental testing. This is because the use of cardiopulmonary bypass in small children is associated with some deficits in fine motor, attention and cognitive skills.
When she turned 1, Olivia had her neurodevelopmental testing done as part of Seattle Children’s Cardiac Neurodevelopmental Clinic. The clinic, which is the only one of its kind in Washington state, evaluates and treats babies and children with complex congenital heart defects who had surgery before their first birthday, and provides close follow-up during their first 3 to 5 years of life.
The clinic found no developmental issues. According to her parents, Olivia is walking and talking like any other child her age, and enjoys playing with her grandparents’ dogs.
“We were told to expect some developmental delays, but I don’t notice any,” said Castañeda. “Olivia has been having therapy and everyone says she’s been doing just fine. She walked a week after a year, and will have full-blown conversations sometimes, even if we don’t always know what she’s saying. I think she’s really smart.”
“The most rewarding part about Olivia’s recovery is that she is doing well from a neurodevelopmental standpoint. The future looks good for her,” said Nuri. “We are trying to learn more about what happens to children after surgery. The Cardiac Neurodevelopmental Clinic is great because it gives us the feedback about how our former patients are doing.”
Care close to home

Olivia continues to be monitored by Seattle Children’s partner Children’s Village in Yakima.
Dr. Veronica Schmer, a cardiologist with Children’s Village, began seeing Olivia as an outpatient after the initial surgery. At the time, Olivia was taking blood thinning medication, since she had developed clots in some veins, and was being weaned off of pain medications.
“Administering heart medication is difficult for parents to handle, because the amount of medicine has to be as exact as possible and put into syringes,” said Schmer. “We followed her really closely, giving her family as much support as we could. Her mom did a great job. Initially, Olivia was on feeding supplements, but by the time I saw her, Mom had been able to remove the feeding tube and Olivia was breastfeeding.”
When Schmer saw Olivia earlier this year, Olivia was healed and no longer needed her cardiac medications.
“She is truly a success story,” said Schmer. “Her echocardiogram looked great, and the aortic arch repair has healed nicely. We’re all really pleased with how it’s turned out. The surgeon did a great job, and Mom’s hard work should be acknowledged as well. It’s challenging to have a baby with serious heart defects and it takes a lot of hope to push through with it.”
Though Schmer is retiring after years of working closely with Seattle Children’s, she has made sure that a Yakima-based provider takes over her position.
“I thought that was important,” said Schmer. “It makes a difference for the patient population here to know that there is a provider living locally.”
Castañeda said she wouldn’t wish the situation on another parent, but she is grateful to Olivia’s care team for healing her heart.
“It was a scary experience that nobody wants to go through, but I want to thank everyone at the hospital for being there for us and answering every question that we had,” said Castañeda. “Olivia is doing so well now. She is perfect.”
Resources
- Montana Twins’ Hearts Beat in Harmony Following Unexpected Surgery Days After Birth
- Born With a Hole in His Heart, Hybrid Procedure Helps Rowen Thrive
- Toddler’s Heart Rebounds After ‘Frankenstein’ Heart Procedure

