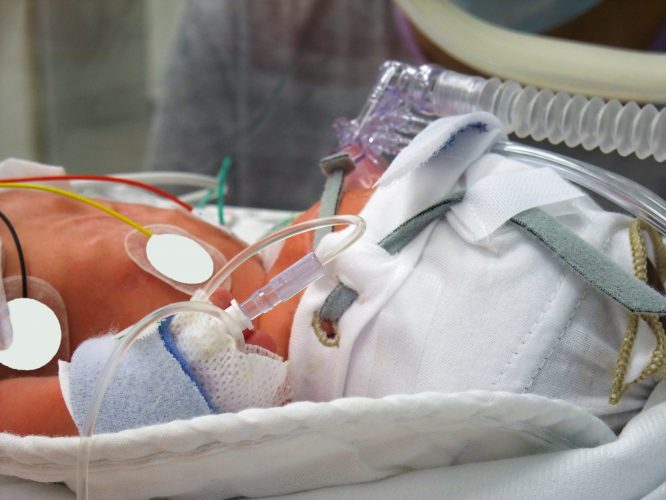
Bronchopulmonary dysplasia is a long-lasting form of lung disease affecting babies born prematurely. Their lungs are not fully formed and are sometimes damaged, and they need extra oxygen through a tube placed into their nose or more support to survive, grow and develop.
BPD also is called chronic lung disease of prematurity. The number of newborns with BPD has risen as more and more babies survive being born many weeks before their due date. An estimated 10,000 to 15,000 newborns develop BPD in the United States each year.
In this Q&A, Dr. Gregory Redding, division chief of the Pulmonary and Sleep Medicine Division at Seattle Children’s and professor of pediatrics at the University of Washington, shares details on Seattle Children’s expanding Bronchopulmonary Dysplasia Program.
Q: Why is Seattle Children’s expanding its BPD Program?
Our Pulmonary and Sleep Medicine Program treats more than 12,000 patients each year, and a growing number of newborns born very prematurely develop symptoms of bronchopulmonary dysplasia. Our expanding BPD program offers a multi-specialty continuum of care that spans from inpatient neonatal intensive care to home. Our BPD team includes specialists from neonatology, cardiology, pulmonary, critical care, nutrition, occupational and speech therapy and several other ancillary services. Our growing research program is discovering better ways to diagnose and treat pulmonary conditions such as BPD.
Q: What’s unique about Seattle Children’s BPD Program?
Seattle Children’s has a remarkable brain trust of people who have significant experience in treating the sickest children. For example, our transport team of doctors, nurses and respiratory therapists are national leaders in safely moving very sick babies by ground and air from other hospitals to Seattle Children’s.
Our nationally recognized Pulmonary Programs care for babies, children and teens with complex needs, including children dependent on ventilator support for years. And, we have the only extracorporeal membrane oxygenation (ECMO) program in the region, as well as a mobile ECMO machine for babies who need a machine to do the work of their heart and lungs.
Seattle Children’s also belongs to the Children’s Hospitals Neonatal Consortium, a national group of specialists who focus on current and emerging trends in neonatal care. Members are Level IV NICUs that work to improve treatment and outcomes for very high-risk infants.
Q: Is there a research component to Seattle Children’s BPD Program?
Yes! Seattle Children’s physician-scientists do research in their laboratories and in the clinics to improve care and quality of life for children with BPD. Our patients have the option to take part in research studies of promising new treatments.
- Robert DiGeronimo, Steve Welty and Laurie Eldredge do research with patients to better understand the treatment and outcomes of babies with BPD.
- In the lab, Laurie Eldredge studies the role of airway lung cells which might predict who will develop BPD.
- Sara Berkelhamer conducts research on newborn lungs.
- Delphine Yung and Kendra Smith work to create new treatments for pulmonary hypertension, which affects many babies with BPD.
Q: How will this program affect the way BPD is treated in the future?
Seattle Children’s has worked to create a culture and infrastructure to nurture innovations, share them with patients and introduce them into clinical practice. We’re not satisfied with the status quo and realize there are opportunities through research and new clinical programs to advance care compared to what it is right now. Today’s state-of-the-art care won’t be the state-of-the-art care in two, five or 10 years. From refining surgical techniques to testing new treatment strategies, we lead efforts to improve care so every child can live their life to the fullest.
Providers can email our BPD team or call 206-987-7777 or 866-987-7777 (toll-free) about patients who need attention right away.

