Seattle Children’s Emergency Department (ED) is an extremely busy place. In 2012, our ED team saw over 36,000 patients. Visits have increased 30 percent since 2003. We exceed recommended capacity every day during our busy season, from November to March.

To handle current volumes, the team cares for emergency patients in three distinct and physically separate spaces – an often inconvenient and inefficient situation for families and staff.
However, on April 23, our ED will move into its new home in Children’s Building Hope expansion. The new ED increases capacity, expands the size of patient rooms, provides adjacent radiologic access and enhances staff visibility and communication. It also improves the way patients and families flow through the space and how caregivers respond to their needs.
“Our current Emergency Department wasn’t built to accommodate the number of patients we’re seeing today,” said Tony Woodward, MD, MBA, chief of emergency services at Seattle Children’s. “A larger facility with more treatment rooms and improved clinical workflow will reduce wait times and make a trip to the ED a far less stressful experience for patients and their families.”
More rooms, better communication and visibility
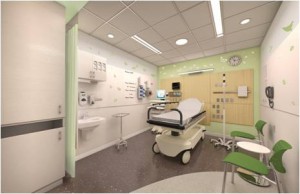
The new ED, designed with input from staff and families, will include 38 exam rooms – 17 more than our current ED. Each room is spacious, which enables parents to stay close to their children and allows medical teams the space they need to provide the best care possible for patients in routine and emergency situations. The additional capacity and improved efficiency will also help to decrease overall wait times and length of stay prior to discharge or hospital admission.
The new radiology center located in the ED also makes it more convenient to get medical imaging, ultrasound and fluoroscopy tests.
While many EDs are arranged with patient rooms that line long halls, our new space is extremely open. To improve visibility, teamwork and communication, and to reassure families that help is always near, patient rooms have large glass doors. Caregivers will be stationed in central work stations where every room is visible.
Alcoves outside each room will provide families and caregivers space to confer. In addition, supplies will be stored close at hand to eliminate wasted travel time.
New model of care

After years of planning, and with input from families and staff, we’ve also improved how patients and families will move through the ED to ensure they receive timely care.
In the new ED, families will receive medical attention as soon as they arrive, and be moved to evaluation and treatment as efficiently as possible. Here are the ways this will happen:
- Changes to the intake & registration process: A registered nurse – rather than a registration specialist – greets families when they arrive. The nurse assesses the patient’s condition before a medication intake coordinator (MIC) – the person who collects the patient’s medication history – shows them to a room. Involving the nurse and MIC at the start of the process reduces potential delays in beginning treatment. Full registration will take place in the room after the primary care team sees the patient, eliminating another possible delay.
- Doing the “The Dance” with each patient: It can be time-consuming and frustrating for patients and families to explain their situation to each person involved in their care. A new process called “The Dance” will bring the entire primary care team into the patient’s room at the same time. The goal is for the team and the family to know the plan and put it into action as early as possible, without the family having to repeat their story multiple times.
- Earlier initiation of care: If a primary care team is not available immediately to see a patient, an “early initiation team” – consisting of a senior level resident or nurse practitioner and a nurse – will work with patients for the first part of their visit. Based on a uniform set of clinical standards, the early initiation team will decide whether to begin tests or provide pain interventions before handing off care to the primary care team. Parents involved in the design process said it was more important to initiate care as early as possible rather than wait for the primary care team to become available.
- Care team zones: Nurses will be assigned to support specific zones of rooms, allowing for better communication with patients and families as well as among the care team. The zones, along with an electronic tracking board, will help care teams better understand which staff members need extra support and who’s available to assist others.
Additional Resources
To learn more about our new ED and the entire Building Hope expansion check out these resources:
- Building Hope Construction Page: https://www.seattlechildrens.org/construction/
- Building Hope, Part 1: Top Ten Features of Cancer Inpatient Unit: https://pulse.seattlechildrens.org/top-ten-features-building-hope-cancer-inpatient-unit/
For Media
If you’re a member of the media and would like to learn more about Children’s new ED, please contact Children’s PR team at 206-987-4500 or at [email protected].

