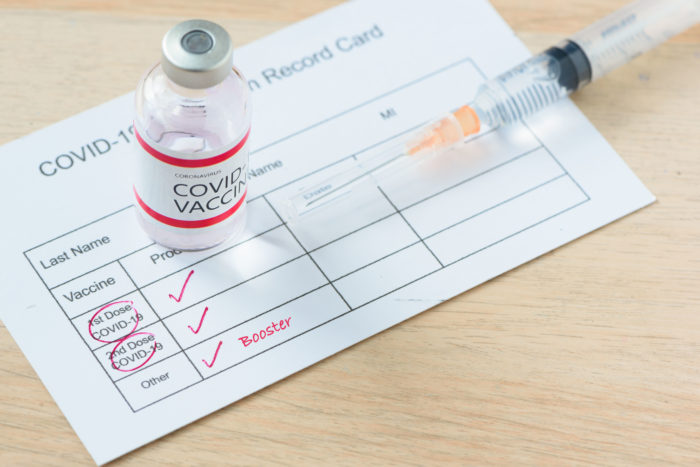
Beginning today, Seattle Children’s is offering the new Pfizer COVID-19 bivalent vaccine booster. It will be available to patients, community members and workforce members. We will begin offering the new bivalent Moderna vaccine booster later this week. The Centers for Disease Control and Prevention (CDC) recommends the updated COVID-19 boosters from Pfizer-BioNTech for people ages […]
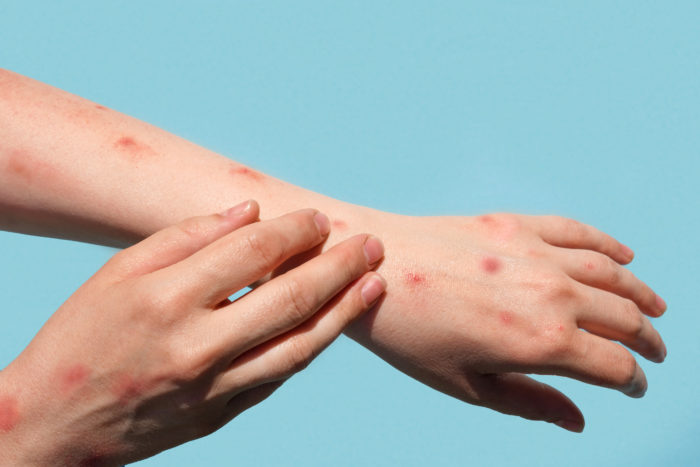
With cases of the monkeypox virus (MPV) being reported across the country, many parents have questions about how to keep their kids as safe as possible. The MPV infection can cause an illness that includes rashes and other symptoms like fever, chills, headache and exhaustion, among others, and is passed by close, prolonged skin-to-skin contact. […]
With a heat wave expected to impact Washington this week, many families across the state have health questions and concerns in mind. Dr. Tony Woodward, medical director of emergency medicine at Seattle Children’s, provides the following advice for parents and caregivers about how to beat the heat as well as keep their kids safe this […]
As warmer temperatures continue to increasingly draw crowds to the water, it’s important to keep safety in mind, especially when children and teens are involved. Dr. Linda Quan, a pediatric emergency medicine physician at Seattle Children’s spoke with KUOW where she shared her five most valuable pieces of water safety advice for parents and caretakers.
Children between the age of 6 months and 4 years old are now eligible to receive the COVID-19 vaccine. For families who have long awaited the opportunity to vaccinate this age group, it’s a sigh of relief. “It provides another layer of protection that we have been seeking for a long time now,” parent Michael […]
On June 21, Seattle Children’s became one of the first locations in the country to offer COVID-19 vaccinations to children ages 6 months to 4 years old. This was a day that Seattle Children’s staff has long worked toward, as Seattle Children’s doctors were also involved clinical trial research for COVID-19 vaccines for this age […]
Over the past eight years, Seattle Children’s has worked diligently across Washington to protect youth from firearm tragedies and improve safe firearm storage practices Lara Sim, Seattle Children’s Director of Community Health and Isabell Sakamoto, Program Manager of Suicide and Injury Prevention at Children’s bring you this post as part of our Keeping Kids Healthy efforts. […]
Dr. Annika Hofstetter and Dr. Matthew Kronman spoke with On the Pulse to answer questions parents may have about the flu vaccine this year.
Seattle Children’s Education Department provides free services for students who will be in the hospital for at least one week. The teachers are certified by the state of Washington in both general and special education. They’re experts at supporting kids and their families when children and teens are suddenly out of school and as they […]
Whether you’re in the “I need school to start now!” camp or the “Summer just started” camp, the fact is that the new school year is approaching quickly. Every year, back-to-school time is met with emotions ranging from excitement to nervousness or fear, but this year that’s even more true for students and families. Dr. […]