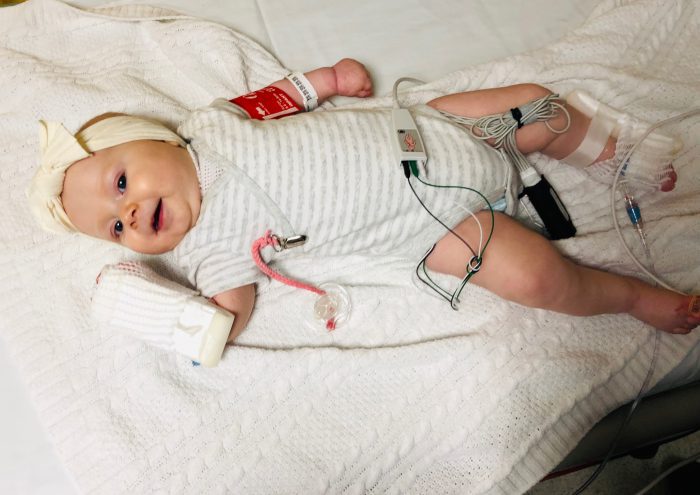
Tuesdays are 2-year-old Malachi Stohr’s favorite days. Every Tuesday, rain or shine, Whitney Stohr and Malachi bundle up and wave to the garbage men as they empty the garbage bins at the end of the driveway. Malachi and Whitney then take a walk around the neighborhood, following the big green truck along its route. Malachi […]
On May 7, 2018, Whitney Stohr slumped to the ground in the corner of her son’s room in Seattle Children’s Pediatric Intensive Care Unit. Her son Malachi, who was born with a severe form of spina bifida, had undergone a tracheostomy days before. When he woke up after the procedure, his pain was so intense […]
It’s been over three years since Maxford Brown woke up one morning not feeling well. Neither Maxford nor his family had any idea that it would mark the beginning of a life-changing journey with a rare, but serious neurological condition called acute flaccid myelitis, or AFM. “I suggested it might help for him to lay […]
Grace Carney was 16 years old when she first began falling. Before long, she was falling every day. It got so bad that she had to rely on other people — family members at home and aides at school — to help her walk. For Grace, this was the latest in a lifetime of medical […]
Childhood tics and movement disorders come in all shapes and sizes. Tics can range from a subtle nasal sniff or throat clearing to a more severe head snap or vocal outburst. Tics that start in elementary school and continue during adolescence are also common. According to Dr. Dararat Mingbunjerdsuk, a neurologist that specializes in movement […]
Tara Nadella shares her personal experience as the sibling of a patient at Seattle Children’s and explains why she approaches life with a lens of inclusion. Updated March 4, 2022: Thank you to our community of donors for your outpouring of sympathy, support and interest in celebrating the life of patient Zain Nadella, who recently […]
In the largest genetic study of the most common birth defects of the brain diagnosed during pregnancy, researchers from Seattle Children’s Research Institute say their findings evolve our understanding of brain development. The findings will also change the information given to expecting parents when cerebellar malformations, such as Dandy-Walker malformation and cerebellar hypoplasia, are detected […]
When Arabella Smygov was diagnosed with spinal muscular atrophy (SMA) type 1 at 3 months old, the first recommendation Dr. Fawn Leigh, a neurologist at Seattle Children’s, gave her parents, Sarah and Vitaliy, was to wait on searching for information about SMA online. This is because up until a few years ago, SMA type 1 […]
The lopsided smile on Makenzie’s face said it all. She had just thrown up, and her dad, Shawn Childs, was helping her get cleaned up in the bathtub. “My husband yelled for me to come into the bathroom and then asked Makenzie to smile,” Jamie Childs, Makenzie’s mom, said. “The smile was devastating. It was […]
At 5 months old, Tyler Cassinelli, now 3, was battling both liver cancer and intractable epilepsy. When he was at Seattle Children’s preparing to undergo cancer treatment, Tyler had a seizure that stopped his breathing. “It was one of the scariest moments of my life,” said Jane Cassinelli, Tyler’s mother. “We could see his stats […]