Emily Talbot, 17, shares her story about her lifelong battle with a rare brain disease and how she has overcome the physical and mental health challenges caused by the condition through writing and performing music. Although I look like any other 17-year-old, people don’t know that I live in pain 24 hours a day. Since […]
Sometimes it is the simplest of moments that can bring a family with a child in the hospital the most hope. For Tony and Laurie Donati, such a moment occurred when a neurologist at Seattle Children’s Neurosciences Center handed their son Dominic Donati a pen and paper and asked him to write a sentence only […]
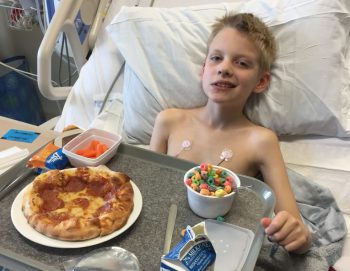
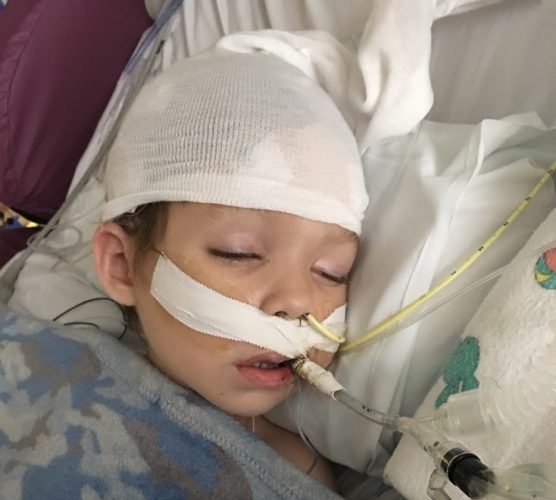
Parents David and Jennifer Cowan share how the rapid initiation of a special medical diet known as the ketogenic diet helped their son recover by leaps and bounds after he suffered from a rare, life-threatening form of epilepsy known as febrile infection-related epilepsy syndrome (FIRES). For more about how the ketogenic diet is used to […]
Doctors first started using the ketogenic diet to treat patients with epilepsy in the 1920s. While the diet has evolved over the decades to include less strict versions, and is gaining mainstream popularity for weight loss, children with epilepsy and other neurological conditions continue to benefit from its seizure-controlling effects. The ketogenic diet team at […]
Next time a workout has you winded, the inhibitory neurons in your brain may be to blame. This is according to new research from Seattle Children’s Research Institute that offers fresh insight into how the brain sets the pace of breathing. In a study published in the journal Nature Communications, researchers used laser light to […]
A new study published by researchers from Seattle Children’s Research Institute reveals how neurons in the brain fuel drug-seeking behavior following compulsive drug use. Their findings, published online in Addiction Biology, suggest inhibiting one group of neurons’ activity may prove to be a highly effective treatment for reducing relapse in recovering addicts. While the science […]
Eight years ago, Dr. Jeff Avansino, a surgeon at Seattle Children’s, and his wife, Dr. Amy Criniti, welcomed their third child – a boy named Luke. For the first few months of Luke’s life, he developed as expected. At about 6 months old, he started having spells of irritability. Avansino and Criniti, both physicians, thought […]
With 2018 in full effect, On the Pulse is taking a moment to hit rewind to share five stories that might have floated beneath the flurry of headlines in 2017. We invite you to take a look back at some of last year’s stories that inspired us and gave us hope. 1. A Mother’s Intuition […]
When 4-year-old Lillee Haynes runs through the doors of Seattle Children’s South Clinic for her speech therapy appointment and heads straight for a table covered in crayons, it’s hard to imagine that nearly two years ago she faced hundreds of epileptic seizures each day. “Her seizures happened so often that I installed a camera above […]
Seattle Children’s researchers will launch an innovative program in early 2018 aimed at shifting the culture of safety in youth sports and building concussion awareness during competitive play. The program, called One Team, emphasizes community engagement in conducting brief pre-game safety huddles involving coaches, officials, parents and athletes, with a goal of addressing both sportsmanship […]