Seattle Children’s is proud to announce that this week, Forbes ranked the hospital #10 on its list of “America’s Best Employers” for 2016. Seattle Children’s is also the third highest ranked company in the “Healthcare & Social” category. Other top-ten companies include Google, Costco Wholesale, SAS and JetBlue Airways. To create the list, Forbes surveyed more than 30,000 U.S. […]
Children with type 1 diabetes and their families have to do several calculations throughout the day to stay healthy. Did my daughter check her blood sugar before breakfast? Does she need an extra snack because she has gym class? Is there someone at school to help my child check her blood sugar? Type 1 diabetes […]
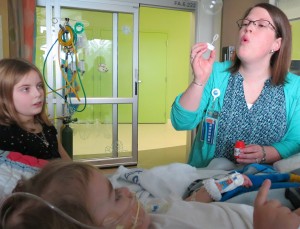
Madeline Holt is a bubbly, positive 3-year-old who likes to cuddle, listen to music, play with blocks and cars, and, in typical toddler fashion, do what she wants to do when she wants to do it. She is also strong and determined to beat all odds stacked against her. At age 1, Madeline was diagnosed […]
Amie Lusk couldn’t have known it at the time, but she started on her career path the day she got caught sleeping in the book nook of her fourth grade classroom. For weeks, she had been hiding her fatigue and sneaking naps in the nook. But that day a classmate found her, woke her up […]
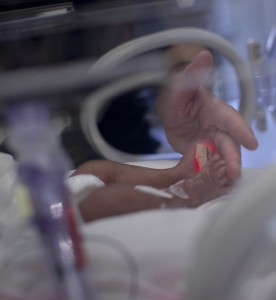
Every new mom hopes to have a healthy baby who enters the world right on time. But unfortunately, deliveries don’t always go as planned, and some babies arrive too soon. Preterm birth, which according to the CDC occurs when an infant is born before 37 weeks of pregnancy, affects about one out of every 10 […]
Transplant day is a joyous milestone for children and families who’ve been through a difficult illness. But the healing does not end when the new organ is in place—in fact, that is when the real work begins, according to Dr. Jodi Smith, Medical Director for the Kidney Transplant Program at Seattle Children’s. “One of the […]
For a child, having to wear a bulky, fiberglass cast around an arm or leg might not sound like a fun treatment option, especially when they need to wear it for up to six weeks. So doctors at Seattle Children’s are doing what they can to make the experience a little more fun. “What color […]
When I was 16, I spent 10 days at Seattle Children’s in the Inpatient Psychiatric Unit (now called the Psychiatry and Behavioral Medicine Unit, or PBMU). I fought it. I hated it. I couldn’t get out of there fast enough. Looking back three years later, I can tell you that those were the most important […]
This summer, Seattle Children’s hosted a reunion for patients who have one unique experience in common: Extracorporeal Membrane Oxygenation (ECMO) played in key role in saving their lives. Patients, families, doctors and nurses gathered to celebrate the 25th anniversary of Seattle Children’s use of ECMO, an advanced life-support therapy that can replace heart and lung […]
When Seattle Children’s Family Advisory Council opened nominations for the 2015 Family Choice Awards, patients and families responded with more than 200 names – each one belonging to a staff or faculty member who made an indelible impression for all the right reasons. With great difficulty, the advisory council whittled down the nominations to select […]