Paige Norris’s young life seemed to be sailing along with fair winds and sunny skies. At 10 years old she was an enthusiastic tennis player with lots of friends and a stellar academic life – two years ahead in every subject. But sometime in fourth grade her internal weather shifted, and she developed debilitating abdominal […]
Kathia Vega Flores will never forget the way her friends and family reacted when she came home from a month-long hospital stay at age 11: They did not recognize her. Kathia had been diagnosed with lupus, a lifelong disease that causes inflammation throughout the body. The medications used to control her disease caused Kathia’s body […]
At 12 years old, Pepper Snider knew something wasn’t quite right. After a bout of Mononucleosis (mono), Snider began feeling a sense of enjoyment from hunger and started to purposely restrict herself. Years later, a comment from an eighth grade classmate would put everything into focus. “Look at that roll.” It was the beginning of […]
Paul Wright dreamed of one day living in Seattle’s bustling downtown and working in one of the many sprawling skyscrapers. But as a boy, it seemed like a near-impossible dream. He was born with a physical disability, arthrogryposis, a condition that prevents joints from moving as much as normal. Doctors thought he would never walk […]
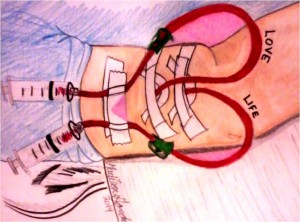
Congratulations to Seattle Children’s patient, 18-year-old Madison Gordon, from Goldbar, Wash., who won first place in the American Kidney Fund’s Calendar Kids Art Contest. Her artwork, which she calls “Love Life,” will be featured on the cover of the American Kidney Fund’s 2015 calendar. More than 4,200 people voted and selected Madison’s drawing to be […]
Meet Molly On Feb. 17, 2008, Erin and Bill Hamilton welcomed their daughter Molly into the world. She appeared to be a perfectly healthy, 9-pound baby girl, but a newborn screening test revealed Molly had cystic fibrosis. “We were devastated,” Erin said. “We didn’t know anything about cystic fibrosis and had no idea how this […]
In honor of Brain Tumor Awareness Month, former Seattle Children’s patient Nina Garkavi shares her experience of battling a brain tumor as a young adult. My name is Nina Garkavi and I am now 25 years old. I would have never thought I would be so closely connected to Seattle Children’s Hospital. My family moved […]
Last year at my son’s high school graduation, I was overcome by a flood of emotion. Not surprising you might say; all moms get choked up when they see their young adult in cap and gown, on the verge of an important life transition. I started thinking back to when Justin was just a preschooler, […]
Eighteen-year-old Ibrahim El-Salaam, aka “I-Bizzle,” was born with a blood disorder called sickle cell disease and has been coming to Seattle Children’s Hospital for as long as he can remember. His disease has required him to spend a lot of time in the Inpatient Cancer Unit at Seattle Children’s, which houses patients who require inpatient […]
Some moments are so significant the weight of them seems to hang in the air. I experienced this first-hand when cancer survivor Milton Wright III met the people who helped save his young life. You may remember Wright, the leukemia patient who achieved remission thanks to an immunotherapy protocol designed by Mike Jensen, MD, at […]