Each week, poets Ann Teplick and Sierra Nelson arm patients at Seattle Children’s Hospital with a notepad, pen and thought-provoking prompts to help them discover the power, and therapeutic nature, of the written word. Some patients use writing to share their story or process difficult emotions, while others use it to ignite their imagination and […]
Twelve-year-old Alan Louie has been in and out of hospitals since he was a baby. Born with kidney disease and renal failure, Alan is no stranger to blood draws, medications and doctors. For him, it has always been a part of his family’s routine. He’s never viewed himself as being sick though, and it’s something […]
Julie Kobayashi, a 12-year-old girl from Hawaii, is Seattle Children’s third patient to receive the HeartMate II ventricular assist device (VAD), a device that allowed Julie to leave the hospital while waiting for a life-saving heart transplant. This is her story, from failing heart to transplant. Julie Kobayashi started feeling sick on a Saturday in […]
Meet Olivia Rickert and Michile Smith: Two generations apart, but linked forever by their special hands. When Olivia Rickert was still in utero, an ultrasound at 20 weeks revealed that she had inherited a genetic mutation passed down from her mother and maternal grandmother. In Olivia’s case, the mutation was expressed as a cleft (split) […]
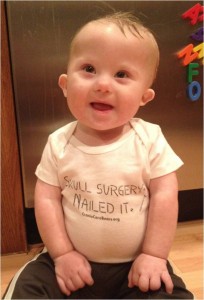
In honor of World Down Syndrome Day, Melanie Harrington shares excerpts from her blog, Our Journey Through Life – a rich chronicle of a baby’s fighting spirit and a mother’s courage to walk “the road less traveled” and arrive a better person. May 2012: Our world changes forever We get the call we’ve been dreading: […]
Thanks to a visit from a few very special cowboys, today is a day that 16-year-old Austin Dunlap will never forget. Dunlap, who is being treated for Acute Lymphoblastic Leukemia at Seattle Children’s Hospital, is a big fan of Professional Bull Riders (PBR). But due to his recent bone marrow transplant, he is unable to […]
If you happen to stroll through Seattle Children’s Hospital’s medical or surgical unit on a Tuesday, you’ll notice something’s a little different – the air feels a little lighter. You’ll likely hear sounds of music and laughter flowing through the halls, and you may even encounter a juggling act. The spirits of patients, families and […]
As a child, Christina Hughes had trouble paying attention in school. She was criticized for her outbursts in the classroom and constantly forgot her homework. Doctors diagnosed her with Attention Deficit Disorder (ADD), but her symptoms were never relieved by therapy. Her academics and social life suffered. “It was always hard for me to make […]
In honor of American Heart Month, we are sharing Gabrielle’s incredible journey from sick baby to healthy toddler. Christen Simon was 18 weeks into her third pregnancy when a routine ultrasound revealed the unthinkable: a serious birth defect. The daughter that Christen and her husband would call Gabrielle would need a heart transplant soon after […]
In honor of American Heart Month, we are sharing a series of stories about some of our incredible heart patients who have overcome the odds. Nobi Johnson was a seemingly healthy, charismatic and extremely athletic 13-year-old girl. She excelled at sports and was a star on the basketball court and soccer field. There was nothing […]