
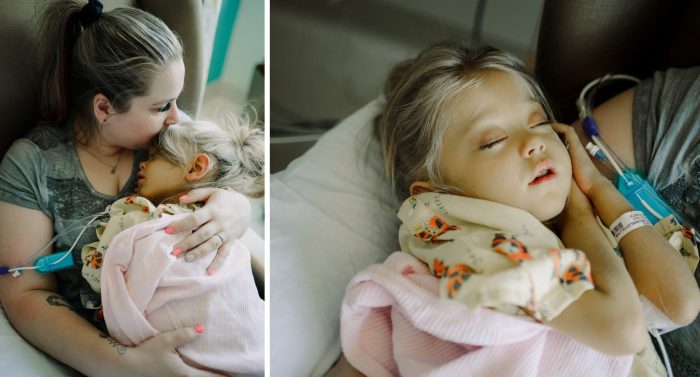
Janessa Felt watched helplessly as her 2-year-old daughter’s sunny disposition began to fade away. Charlotte’s bright smile and infectious laugh usually hid her struggle well, but that façade was cracking. Charlotte was getting sicker, which was evident by her yellow skin, the silver highlights in her hair and her large distended belly. Her piercing blue eyes were sadder than usual. She laid cradled and uncomfortable in her mother’s arms as fluid built up in her abdomen. Her liver was failing her.
Charlotte was admitted to Seattle Children’s a week earlier. Hospital stays weren’t abnormal for them, but this time was different.
“It is hard to watch your baby be so sick, hooked up to so many machines, and not be able to do anything,” Janessa said. “As a mother, you want to be able to take that pain away.”
Janessa didn’t know how much longer Charlotte would be able to wait for a miracle. She had been on the waitlist for a new liver for year already.
“It wasn’t scary until recently,” Janessa said. “Now, it’s clear she needs a new liver. We just want her to start feeling better. It’s heartbreaking to watch her go through this.”
A medical home
Charlotte has biliary atresia, a rare liver condition that occurs when a baby’s bile ducts do not form normally. About 1 in 15,000 babies are born with biliary atresia. She was diagnosed at Seattle Children’s at only 9 weeks old.
“Biliary atresia is the most common cause of children needing liver transplantation,” said Dr. Evelyn Hsu, medical director of Seattle Children’s Liver Transplant Program.
Seattle Children’s is the only pediatric liver transplant program in the Pacific Northwest, and outcomes for patients who receive liver transplants are among the best in the nation.
Seattle Children’s soon became a second home for Charlotte and her family.
“This is our place, and our doctors and nurses are our family,” Janessa said.
To survive, babies like Charlotte with biliary atresia need surgery. At only 2 months old, Charlotte underwent a procedure called the Kasai procedure where surgeons removed blockages in the ducts outside the liver and created a way for bile to drain from the liver into the intestines.
For a year, Charlotte did well. But the procedure wasn’t a cure. She became sick again, and on May 1, 2018, she was listed for transplant.
Advocating for change
A year is a long time to wait for life-changing news.
“Her life was at risk until the transplant,” Hsu said. “There is a lot of anxiety that comes with waiting. The fact is, there are more people waiting than there are livers.”
This year, about 50 children will die waiting for a liver. It’s a number that keeps Hsu up at night. She thinks about that number when she sees patients like Charlotte.
It’s for this reason Hsu is passionate about organ donation and allocation, and advocates for children on the waitlist. Currently, policy deems that livers be allocated to adults locally and regionally instead of critically ill children nationally. She hopes to change this to improve children’s access to organ transplants by prioritizing pediatric patients waiting for livers.
“After transplant, these children will go on to live full lives,” said Hsu. “At what point will we make kids a priority?”
A failing liver
As time passed, Charlotte’s liver got worse. One day she was seemingly fine, the next she’d spike a fever and they would find themselves once again at Seattle Children’s.
April 24, 2019 was one of those days. Janessa had called her trusted care team because Charlotte wasn’t feeling well again, and they came to Seattle Children’s Emergency Department.
“It seemed like something was off,” Janessa said. “That’s the great thing about our team – they are there whenever we need them.”
Her mother’s intuition was tingling, and for good reason. Charlotte needed a procedure to drain fluid from her abdominal cavity. She was soon admitted.
Usually, we have a bag packed every time we come to the hospital in case we have to stay,” Janessa said. “We bring enough for a couple days.”
This visit would be longer. They were told they’d be staying until the transplant.
A mix of emotions
On April 30, Janessa received the best news of her life.
Dr. Andre Dick, surgical director of Kidney Transplant at Seattle Children’s, waked into their room, a smile on his face. They had a match.

“When we got the news, I didn’t know whether to get sick or cry,” Janessa said. “It was finally our time. I couldn’t believe it.”
The next day, Charlotte was taken into the operating room, surrounded by the doctors and nurses Janessa calls their second family, to receive a new liver. That night was restless for Janessa.
“I was excited, but numb,” Janessa said. “We’ve waited so long for this day.”
Janessa said she was on pins and needles waiting for Charlotte to come out of surgery.
“Every time our phone rang for an update it took our breath away,” Janessa said.
Hours went by and Charlotte was finally out of surgery. She had a new liver.
Gratitude for the donor family
It’s been two weeks since Charlotte received a lifesaving transplant. Charlotte’s yellow skin tone has vanished, replaced by a color Janessa describes in one word: beautiful.

Dick, who performed the transplant, said Charlotte is doing very well. Charlotte has gone through some ups and downs after the inital surgery, but she’s recovering, and they can finally see the light at the end of the tunnel. They are finally home again.
To the donor family who saved her daughter’s life, Janessa said it’s hard to put into words the gratitude they feel.
“We’re deeply sorry for their loss,” Janessa said. “It breaks our heart that they lost their loved one. We are forever grateful for the amazing gift of life that the donor has given our daughter and family.”
Janessa is excited for Charlotte’s future. They can’t wait for her to get to be a normal toddler and for her bright future ahead.
“She’s alive today thanks to the transplant,” Janessa said. “She has a long life ahead of her now.”
To Charlotte’s care team, Janessa has a special message.
“They’ve changed our lives and saved Charlotte,” Janessa said. “We’ll always be incredibly thankful.”
To learn more about organ donation visit LifeCenter Northwest and Donate Life.

