Neurosurgeons at Seattle Children’s Hospital have long suspected that epilepsy patients who have surgery earlier in life have better outcomes than those that wait. Now they have data to confirm their instincts.
In a study recently published in the Journal of Neurosurgery Pediatrics, lead author Dr. Hillary Shurtleff, neuropsychologist and investigator at Seattle Children’s Research Institute Center for Integrative Brain Research, found that early surgical treatment of focal seizures – those that affect only one area of the brain – in preschool aged children is highly beneficial. The results showed that surgery can reduce the amount of seizures and the number of medications patients are on while helping improve intelligence outcomes.
“In the past, surgery has often been viewed as a last resort that becomes an option only when the severity of a child’s seizures greatly impedes their ability to properly function,” Shurtleff said. “Brain surgery of course carries risks and there was an assumption in the field that potential loss of cognitive function from surgery would be worse than impairments that may arise from ongoing epileptic seizures. Now we know this to be untrue in specific cases, and have data to show that not intervening early can have worse outcomes.”
The study, titled, “Impact of Epilepsy Surgery on Development of Preschool Children: Identification of a Cohort Likely to Benefit From Early Intervention,” reviewed the data and medical charts of 15 Seattle Children’s patients who had epilepsy surgery between the ages of 2 and 6. The team was very purposeful in choosing a very select group because they realized that specific variables such as age at surgery, early surgery, short seizure duration, focal seizures associated with lesions, and small resections make a difference to outcome.
The study showed that patients with seizure durations of less than 6 months prior to surgery showed improvement from their pre-surgical cognitive baselines. In contrast, those with seizure durations of greater than 6 months prior to surgery had lower scores on the Wechsler Full Scale IQ and nonverbal intelligence scores.
“There is an inherent and understandable fear associated with brain surgery, and oftentimes parents and doctors choose to wait to see if less invasive treatments like medications will work,” said Shurtleff. “This study is important because it showed us that doing the surgery earlier can improve the future for these patients. We simply can’t continue to wait years to take this step.”
Bailey’s journey with epilepsy
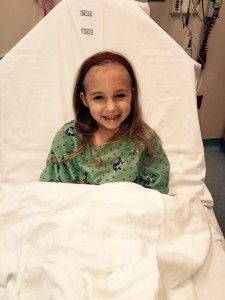
Epilepsy is more common in children than in adults, affecting nearly one in every 20 child under 5. The Moser family knows more about these statistics than they’d care to. Their 5-year-old daughter, Bailey, came to Seattle Children’s from Boise, Idaho, to have surgery to help treat her epilepsy.
Bailey’s mom, Leanna Moser, first realized her daughter was suffering from seizures when she was 4 years old. From that point on, Bailey was required to take five or more medications per day at the maximum dosage to keep her seizures at bay.
“Bailey was having 10 to 40 seizures per day,” said Moser. “The medications were helping a little, but we were constantly visiting our local ER and we were growing increasingly worried about her safety while having seizures. We knew deep down we’d eventually have to do something more to help her.”
Moser, a family nurse practitioner, began researching other potential options for her daughter.
“I started by looking into the best hospitals to treat epilepsy and asked our doctor for a referral to Seattle Children’s,” she said.
Upon arrival at Seattle Children’s, which is the only hospital in the Northwest that is a Level IV accredited Epilepsy Center, a MRI picked up a lesion that was likely causing her focal seizures. Dr. Jeff Ojemann, division chief of Neurosurgery and director of epilepsy surgery, saw Bailey as the perfect candidate for surgery because of the location of her lesion and her age. The Moser family agreed, and moved forward with the surgery.
 “We knew she was in the best hands possible, and we prayed so hard for a good outcome,” said Moser.
“We knew she was in the best hands possible, and we prayed so hard for a good outcome,” said Moser.
Bailey came out of the surgery in high spirits, even giving her mom a high-five.
“The surgery went so remarkably well and we couldn’t be more pleased,” said Moser. “Bailey looked bright eyed; the glaze from her constant seizures subsided. We really felt like we had Bailey back for the first time in forever.”
Today, Bailey has been weaned off the majority of her medications and rarely experiences seizures.
“Doing this surgery earlier in life can put kids on a better trajectory,” said Shurtleff. “At Seattle Children’s, we are lucky enough to be able to offer the highest-level of surgical care because we have a multi-disciplinary team, comprised of epileptologists, neurosurgeons, radiologists, neuropsychologists and others. We can’t be more pleased when we see these kids do well, and having this knowledge about early surgical intervention will help improve outcomes for future patients.”
Resources:
- Seattle Children’s Neurosurgery Program
- Seattle Children’s Epilepsy Program

