
Grace Carney was 16 years old when she first began falling. Before long, she was falling every day. It got so bad that she had to rely on other people — family members at home and aides at school — to help her walk.
For Grace, this was the latest in a lifetime of medical setbacks, many of which stem from neurofibromatosis type one (NF1), a genetic disorder that causes tumors to grow all over the body, including under the skin and on the nerves.
To improve Grace’s ability to walk, a doctor in Spokane recommended a major orthopedic surgery. But as the Carneys prepared for that surgery, an MRI result flipped everything upside down and brought them to Seattle Children’s, where Grace received an innovative medical treatment that changed her life and could do the same for countless others with NF1.
No good options
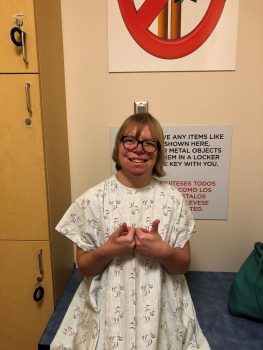
Grace’s personality is as big as her smile. She can tell you everything you ever wanted to know about The Super Pops, she owns almost every toy in the Littlest Pet Shop line and she loves the Magic Tree House books. Grace, who is now 18, has such a bright disposition that it’s startling to learn about all the challenges she’s faced.
Grace began having seizures at birth and spent time in a Neonatal Intensive Care Unit in Spokane. She took anti-seizure medication for eight months and saw a neurologist for years. She was also born with a large tumor on her left foot.
After a biopsy at age 3, she was diagnosed with NF1, which affects approximately 1 in 3,000 people and typically presents during childhood. While the tumors associated with NF1 (called neurofibromas) are usually benign, they can significantly impact the patient’s quality of life — especially plexiform neurofibromas, which grow on the nerves.
Over the years Grace saw a variety of specialists, spent hours in MRI machines and had numerous surgeries, including on her foot, eyes and heels. She even had a pinky toe amputated when the tumor in her foot forced the toe so far out of alignment that wearing shoes became agonizing.
Grace is also cognitively delayed; she is in special education and works with a speech therapist.
When Grace began falling, X-rays showed the bones in her left leg were slightly turned. An orthopedist recommended a procedure in which surgeons would break and rotate her femur, tibia and hip. But knowing Grace had NF1, the orthopedist also ordered an MRI of her spine to make sure nothing else was contributing to the problem.
That proved a wise decision: The MRI showed a plexiform neurofibroma wrapped around the spinal cord in Grace’s neck and compressing the cord. That’s when Grace was referred to Dr. Samuel Browd, a neurosurgeon and director of Seattle Children’s Hydrocephalus Program.
“Her spinal cord was so compressed that Dr. Browd couldn’t believe she was walking,” Grace’s mother, Janet Carney, recalled. “He said Grace was one fall away from becoming quadriplegic. If she’d had that orthopedic surgery, it might have made her quadriplegic because of the tumor’s location.”
Unfortunately, the solution was to trade one risky surgery for another. Browd needed to operate on Grace’s spine — a procedure that would likely be the first of many.
“Once we’ve removed the tumor, kids with NF1 often need additional surgeries later for cervical spine stabilization and, sometimes, tumor recurrence,” said Browd.
“It was going to be a pretty scary surgery,” Carney said.
Grace would be hospitalized for a week, including at least three days in the Intensive Care Unit. With no other options available, the family prepared for yet another surgery.
Then, two days before Grace’s procedure date, the Carneys received an unexpected call that changed everything.
“A lot to lose, but also a lot to gain”
When Dr. Sarah Leary, neuro-oncologist and medical director of Seattle Children’s Brain Tumor Program, heard about Grace’s impending surgery and learned that Grace had NF1, she quickly called Browd and told him Grace might be a candidate for a MEK (pronounced mek) inhibitor.
MEK inhibitors are a family of drugs that slow or block the activity of specific mitogen-activated protein kinsase (MEK) enzymes, which are involved in cell production. MEK inhibitors are approved to treat melanoma and other types of cancer, but in recent years researchers have found them to be effective in treating some brain tumors and plexiform neurofibromas. These therapies seem to be particularly effective in children with NF1.
Browd called the Carneys and explained this medical option, telling them, “I think it’s worth a shot.” Though nervous about the therapy, the Carneys leapt at the opportunity to save Grace from going through another surgery.
After they made that decision, things moved quickly. Within days they met Dr. Aimee Sato, neuro-oncologist and medical director of Seattle Children’s Neurofibromatosis Program, and Lauren Finamore, nurse practitioner in the NF Program. Sato recalls that in addition to having trouble walking, Grace had tingling in her arms and some weakness in her left leg.
In early October, Grace began taking a MEK inhibitor called trametinib — a daily oral medication convenient for outpatient use. The NF team closely monitored her via monthly clinical exams and MRIs. Because of Grace’s physical condition, they feared their intervention may have been too late.
“Grace was in a very challenging and clinically dangerous situation,” Sato said. “Typically the patients we’re intervening on are more stable. Grace had a lot to lose, but also a lot to gain.”
The proof is in the walking

Grace’s grandmother and great aunt were the first to notice a difference.
“Within the first two weeks Grace was on the medication, they swore she was walking better,” Carney said. “And I said, ‘You guys are wrong — it can’t work that fast.’” Carney changed her mind, however, when she saw Grace no longer needed help to walk.
The team at Seattle Children’s noticed other changes after just one month. “Her left leg was stronger,” Sato said. “She also didn’t have any of the sensory changes in her upper extremities.”
One of Grace’s favorite things is going for boat rides on Spirit Lake in Idaho. Their vacation house is a quarter-mile uphill from the lake, and the trek had become a struggle for her. The family was planning to buy a golf cart to shuttle her back and forth, but not anymore: Today, Grace has no problem powering up the hill.
Grace’s MRIs showed improvement within two months — first the tumor stopped growing, then it began to shrink.
“Each time she gets an MRI I hold my breath because I hope to continue to see improvement,” Sato said. “So, when I do see it, it’s absolutely thrilling.”
And as for the falling?
“She has not fallen once since she’s been on the medication,” Carney said.
For the first time, a non-surgical option
On April 10, 2020, the FDA approved a MEK inhibitor called selumetinib for treatment of NF1 — the first medical treatment ever approved for the condition.
April 10 also happens to be Grace’s birthday.
Seattle Children’s Brain Tumor Program began offering MEK inhibitor therapy off-label to patients in 2017, and the NF Program has used MEK inhibitors as a standard treatment for plexiform neurofibromas since the program was founded in 2018. In that time, Sato and her team have placed approximately 30 patients on MEK inhibitors; most of those patients have seen their tumors stabilize or shrink.
Seattle Children’s results align with current research, which shows that MEK inhibitors can shrink tumors and provide clinical benefits like Grace has experienced. More research is needed, though, to determine whether MEK inhibitors can eliminate tumors.
Leary is hopeful about the positive impact the NF Program can continue to have on those living with NF1.
“I’m excited that we can not only contribute but potentially lead the way,” she said. “We’re at a turning point that gives many kids the opportunity to try medical therapy first.”
Sato agrees. “It’s exciting because we’re able to help patients in a way that we weren’t able to before,” she said.
Hope for Grace and others

Grace has been on the MEK inhibitor for approximately nine months. While the results are overwhelmingly positive, the treatment has caused some side effects, including an acne-like rash on her face, swelling in her left foot and some hair loss. Despite the side effects, Carney says Grace’s improvement is worth it.
“Seeing her able to do so much more gives me hope because, even before knowing about the tumor in her spine, we were preparing for her to potentially end up in a wheelchair,” she said.
Grace will remain on trametinib for two years total. Depending on how things progress, she may switch to selumetinib. Sato hopes the tumor continues to shrink and will remain stable after Grace eventually stops taking the medication.
The primary goal, however, is for Grace to avoid another risky surgery. The future isn’t certain, but thanks to MEK inhibitors, Grace and many other patients with NF1 now have options.
“It’s much better for these kids if we can manage them medically rather than operate,” Browd said. “My hope is that MEK inhibitors put me out of business for these types of tumors.”

