 It was during a 20-week ultrasound that Sarah Ouellette got life-changing news: Her baby would be born with a serious heart defect.
It was during a 20-week ultrasound that Sarah Ouellette got life-changing news: Her baby would be born with a serious heart defect.
“They didn’t know if my baby would survive,” Ouellette said. “But I knew deep down that I wanted to fight for my child’s life.”
Feeling lost, Ouellette sought out a second opinion.
“I contacted Seattle Children’s, and it was there that I learned a lot more about my baby’s diagnosis. They made me feel more at ease.”
Ouellette connected with Seattle Children’s Fetal Care and Treatment Center, where she was introduced to Dr. Bhawna Arya, director of fetal cardiology, who guided her every step of the way.
Greyson had a diagnosis of pulmonary atresia with intact ventricular septum, a heart condition where only half of the heart has formed.
According to the Centers for Disease Control and Prevention, congenital heart defects (CHDs) are the most common types of birth defects, and babies born with these conditions are living longer and healthier lives. CHDs affect nearly 1% of, or about 40,000, births per year in the United States.
A scary moment, then good news
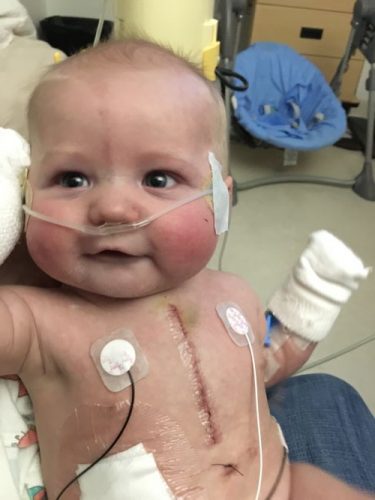 After months of preparation, at 39 weeks, Greyson was born.
After months of preparation, at 39 weeks, Greyson was born.
Everything went well during delivery, and he was immediately transported Seattle Children’s for care.
At just 2 days old, Greyson went in for his first visit to the catheterization laboratory or cath lab. A cath lab provides information on how well the heart works, identifies problems and allows for procedures to open blocked arteries.
As frightening as it was to have Greyson go in for his first cath lab, Ouellette was confident that all would go well. Just a few minutes later, an overhead announcement boomed over the speakers: “code blue.” It was coming from the cath lab.
“That was one of the worst moments of my life,” Ouellette said. “Fortunately, within a few minutes of doing CPR, he was stabilized.”
Then even better news came. It was determined that Greyson wouldn’t need to go through surgery. He just needed to have a stent placed.
“During the cath procedure, we determined whether he needed a transplant,” Arya said. “His coronary arteries, which provide blood to his heart, were looking good, so we put a stent in his ductus arteriosus which is a vessel that allows blood to travel from the body artery to the lung arteries without having to open his chest or do bypass surgery.”
At 8 days old, Greyson was released from the hospital and was sent home with a home monitoring program called CHAMP (Cardiac High Acuity Monitoring Program) that helps monitor a child’s oxygen saturation and daily weight. The information is recorded to help provide the care team with early warning signs and help make sure a child is growing and developing well.
At 6 weeks old, Ouellette noticed something odd with the pulse oximeter, and Greyson wasn’t acting quite like himself. Through CHAMP, Ouellette was able to provide necessary information to the care team to help them figure out what was happening with Greyson’s health.
“It turned out we needed to be admitted to the hospital,” Ouellette said. “We spent a few weeks with Greyson getting a cath and going through some minor complications.”
First surgery and research comes to the rescue
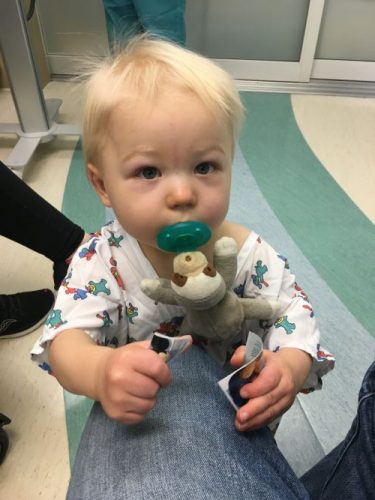 In November 2018, Greyson was finally prepared to undergo his first open heart surgery.
In November 2018, Greyson was finally prepared to undergo his first open heart surgery.
“He needed an early Glenn procedure, which is an operation that redirects blood flow from the upper body to the lungs,” Arya said. “It went well, but he also needed a stent placed prior to going home from the hospital.”
A stent helps keep your arteries, the blood vessels that carry blood from your heart to other parts of your body, including the heart muscle itself, open.
“The Glenn provided stability for Greyson,” Ouellette said. “It got him to a place where he could breathe better.”
As time went by, Greyson’s health remained stable.
Then in June 2020, during a routine cardiology appointment, doctors noticed he had a blood clot.
“To get rid of the blood clot, it would take giving him a shot twice a day, which was so stressful for us and Greyson,” Ouellette said. “Fortunately, we were introduced to a clinical study led by Dr. Agustin Rubio, where Greyson could go on an oral anti-coagulant called Eliquis.”
Greyson was accepted into the study, which eventually helped his blood clot.
Giving Greyson a normal life
 Although Greyson has experienced so much in his 2-and-half years of life, he acts like any other child his age.
Although Greyson has experienced so much in his 2-and-half years of life, he acts like any other child his age.
“He’s considered to be very lucky,” Ouellette said. “He’s reaching all of his key milestones which I couldn’t be more proud of.”
Dr. Matthew Files, one of Greyson’s providers at Seattle Children’s Heart Center, has witnessed the family’s journey over time and sees a hopeful future for Greyson.
“Greyson’s family are an example of why my job is very rewarding and engaging,” Files said. “They were so involved and wanted to know as much information as they could to make sure Greyson had the best outcome possible.”
The Ouellettes have become very active in the community by raising awareness and supporting other families who are going through the same situation as they did.
“It’s rare and impressive to see parents get beyond supporting their own children to advocating for other children and families,” Files said. “They have raised money for care packages to help make other patient families not feel so isolated. They are also continuing to advance both Greyson’s outcome and other children’s through a combination of participating in research and raising awareness through their advocacy. They have worked to raise awareness by joining local and national groups.”
Arya is also awed by Greyson’s family and the ongoing work they’re doing to get the word out about pediatric heart conditions.

“To know that Greyson has already been through so much with his heart and his family is able to give him a normal and good quality of life is just amazing,” Arya said. “The prenatal care packages that Sarah puts together for families are heartwarming. Seeing the reactions families have to receiving the packages before birth and then being able to use them once their baby is born, it makes them feel like someone else has been there and is with them throughout the process.”
As Ouellette prepares for Greyson’s next surgery, she remains hopeful.
“I want to see him get married, travel the world and have his own family,” Ouellette said. “I want him to have the same opportunities as others. I stay optimistic, otherwise I’d be in a very dark place, which is why I’m continuing to fight for more research funding and providing support to other families that have gone through what we’ve gone through.”

