
For Leslie and Jeremy Barnett, Grayson’s black and white Converse Chuck Taylors represent a happy ending to a tough first chapter of life for their son, who weighed just 1 pound when he was born 18 weeks premature last November.
It took eight months and overcoming tremendous adversity for Grayson to grow into the tiny shoes he received the day before his 117-day stay in the Seattle Children’s neonatal intensive care unit ended.
“We were told that Grayson had this Mt. Everest of health challenges to climb,” Leslie Barnett said, recalling a conversation with Seattle Children’s and University of Washington neonatologist Dr. Maneesh Batra when her son was a few days old.
“At that point, Dr. Batra told us that Grayson wasn’t even hiking,” Barnett said. “He wasn’t on the mountain. He was still in his room trying to find his shoes.”
The analogy was a simple way for the Barnetts to put the complex challenges Grayson was facing into perspective for concerned friends and family.
So when Batra dropped off the Chucks, the message was clear and significant: Grayson was ready to begin the next stage of his journey and he had already beaten overwhelming odds.
Labor comes early and without warning
In developed countries, viability—the earliest point at which a fetus has a 50% chance of survival outside the womb—is between 23 and 24 weeks gestation.
So there was concern when Leslie Barnett unexpectedly went into labor with her twins 22 weeks into an otherwise healthy pregnancy. The care team at Kootenai Medical Center in Idaho exhausted all options to halt Barnett’s labor but early delivery proved inevitable.
Sadly, the Barnetts’ daughter did not survive birth. But doctors were able to briefly suspend labor and keep Grayson in the womb. Eight hours later, labor resumed and Grayson was delivered, intubated and taken immediately to the hospital’s Level III NICU.
Grayson was a micro preemie, the term used for babies born before 26 weeks gestation, or who weigh less than 1 pound, 12 ounces.
He weighed exactly 1 pound.
A challenging start for Grayson
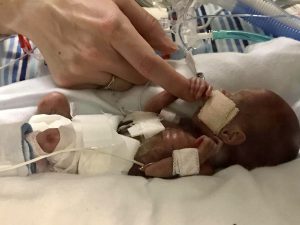
Each day of pregnancy is important in fetal development. Grayson missed more than 100 days of growth critical to strengthening his heart, lungs, brain, digestive tract and skin.
His chances of survival were at 5 to 10%.
“It is incredibly challenging for babies born that early because all the organs meant to be protected in the uterus during pregnancy are now exposed,” Batra said. “For providers, the complications with each organ system present their own challenges, even with the most advanced neonatal care.”
Barnett had extensive knowledge of the challenges Grayson would face. As a respiratory therapist in Kootenai’s NICU, she is often at high-risk deliveries to help newborns breathe.
“It was tough because I know what the complications can be from having such a pre-term baby,” Barnett said. “I know the quality of life could not be great and the likelihood of Grayson surviving was low.”
Heading to Seattle for more advanced care
Realizing how tiny and fragile Grayson’s lungs were, doctors referred him to the Level IV NICU at the University of Washington Medical Center (UWMC) in Seattle, where he had access to high frequency ventilators that were required to help him breathe. But concerns over moving him brought to light the type of complications that lay ahead of him.
Certain blood vessels in the brains of micro preemies are susceptible to rupture with even slight movements. Fear of this prompted doctors to delay Grayson’s transport to Seattle until he was stable.
After 36 hours, Grayson and his mother were flown 45 minutes by helicopter to Seattle.
“He did wonderful on the ventilators at UWMC,” Barnett said. “But we were told that he was in a bit of a honeymoon period.”
Days after Batra relayed his Mt. Everest metaphor to the Barnetts, Grayson’s blood pressure dropped. He had a perforated bowel that was leaking the contents of his intestines into his abdomen, threatening to send him into septic shock. He needed surgery and there was concern he would not make it.
When he was 5 days old, Grayson was transferred to the Level IV NICU at Seattle Children’s to receive specialized care for his surgical condition.
Grayson begins searching for his shoes

Grayson’s weight had dropped to a low of 13 ounces and he was too small and weak for surgery, so a soft rubber tube called a Penrose drain was used temporarily to drain the fluid from his abdomen.
“Grayson tolerated the drain really well,” Barnett said. “He was put on antibiotics and we played the waiting game until he was big enough and strong enough to handle surgery.”
Doctors wanted Grayson’s weight to triple before his surgery. But it wasn’t as simple as feed and grow. Any medication or nourishment had the potential to dangerously affect chemical, hormonal and blood cell count balances in Grayson’s body.
“Extremely premature babies are already at high-risk for a number of threatening health conditions,” said Dr. Robert DiGeronimo, medical director of the Seattle Children’s NICU. “But Grayson had an even more complicated course early on because of his intestinal issues.”
Finding his footwear
Over the next 117 days Grayson, his parents and his care team battled and found answers to every barrier and challenging diagnosis.
Grayson had more than 30 blood transfusions in response to several infections that attacked his weakened immune system. Direct injections were used to treat retinopathy, an eye condition that threatened his vision. A blood clot causing fluid buildup in his head was successfully treated. He had multiple IVs and overcame several other complications.
The Barnetts were a constant presence in the NICU, making sure they saw the care team at each stage of their son’s treatment.
“We wanted to be 100% involved in decision-making and care,” Leslie Barnett said. “The doctors and nurses fought so hard for him and included us in Grayson’s care. We felt that our opinion made a difference.”
Through it all, Grayson grew.
By mid-January, Grayson weighed 2 pounds and he was able to take his first meal—less than 1/8 of a teaspoon of breast milk. He eventually reached his target weight for surgery, and on Feb. 13, 2 centimeters of his intestine were removed.
Five weeks later, Batra dropped off the Chucks for Grayson.
“Grayson weathered so many challenges,” Batra said. “The Barnetts are a really special family who chose to focus on finding the shoes rather than just the mountain. I love the idea of Grayson slipping on his shoes and going on to live the best life he can.”
The following day, Grayson was stable enough to transfer back to the Kootenai NICU to recover closer to home.
“At that point, Grayson didn’t need anymore planned surgery and was no longer on a ventilator,” DiGeronimo said. “He was doing well and he was developing much faster than his corrected gestational age.”
Grayson returned to Idaho on March 23, his original due date.
From 13 ounces to 13 pounds

Grayson’s return to Idaho was a welcome relief to the Barnetts, who were able to rest at home after spending several months in motels and temporary housing provided by Ronald McDonald House. While Grayson responded well to his new environment, several setbacks extended his NICU stay.
On June 3, after 196 days spent in hospitals and countless moments of worry from his parents, Grayson went home for the first time.
“We lived off of hope for months,” Barnett said. “We just hoped. Hour-by-hour. Day-by-day. We lived in the moment.”
Grayson has continued to grow at home and is fast-approaching 13 pounds. He smiles, is hitting the developmental milestones for his adjusted age and can almost roll over all by himself.
He also has his Chucks and a dynamic array of footwear sent by supporters that ensure he’s equipped for any journey that may lie ahead.
“Grayson was a fighter from day one,” Barnett said. “We’re enjoying being at home with him and watching him grow.”
Resources:
- Trends in Care Practices, Morbidity, and Mortality of Extremely Preterm Neonates, 1993-2012, JAMA, Sept. 2015
- Outcomes for Extremely Premature Infants, Anesthesia and Analgesia, June 2015

