 When Cassie Fannin was 19-weeks pregnant with her first baby, she couldn’t wait for the ultrasound that would reveal her child’s gender. During the appointment, she and her husband, Michael, were delighted as they watched their beautiful baby wiggling around on the ultrasound screen.
When Cassie Fannin was 19-weeks pregnant with her first baby, she couldn’t wait for the ultrasound that would reveal her child’s gender. During the appointment, she and her husband, Michael, were delighted as they watched their beautiful baby wiggling around on the ultrasound screen.
Fannin asked the technician, “Is it a boy or girl?”
But the technician’s previously cheerful expression now suggested something was wrong. “I’ll need to check with the doctor,” the technician said while hurrying out of the room.
Moments later, a doctor gave Fannin and her husband the devastating news that changed their lives.
“I left that appointment a completely different person”
Fannin’s ultrasound revealed she was having a girl, but it also showed the baby had a congenital diaphragmatic hernia (CDH) — a hole in the left side of her diaphragm that allowed her stomach, intestines and a portion of her liver to slip into her chest cavity and prevented her left lung from fully developing.
“They told us CDH has a 50% survival rate,” Fannin said. “To say it was a shock is an understatement. We went from being ecstatic about finding out we were having a girl to absolutely devastated in a matter of seconds. I left that appointment a completely different person.”
The doctor offered very little information about CDH but pushed the Fannins to decide if they wanted to continue their pregnancy.
“It was pretty bleak,” Fannin said. “I remember the doctor telling us that if she survived, her quality of life would be very poor. We didn’t know what to do. We were totally lost.”
Finding answers
That’s when the Fannins were referred to Seattle Children’s Prenatal Diagnosis and Treatment Program and met Dr. Kim Riehle, a lead surgeon in the program.
While it is a rare condition, Seattle Children’s providers have cared for hundreds of infants with a CDH, and our pediatric surgery team is one of the most experienced in the nation. With such unique expertise, Seattle Children’s has one of the highest survival rates in the nation for children born with a CDH.
When Fannin and her husband at down with Riehle, they finally found the answers they were desperately seeking.
Riehle described in detail what a CDH diagnosis would mean for their daughter — who they named Summer.
She recommended Fannin give birth at the University of Washington Medical Center and then transfer Summer to Seattle Children’s Neonatal Intensive Care Unit (NICU) before undergoing surgery to close her hernia.
Most notably, Riehle said Summer’s chances of surviving were about 85%.
“She gave us hope,” Fannin said. “Michael and I had been married less than a year and, in many ways, I still felt like a kid myself. I wasn’t sure what I was doing. Kim was one of the first people to make me feel like a mom. She made me feel confident in my instincts, strong in my convictions and reminded me that this was my child and I could handle absolutely anything for Summer.”
The hardest part
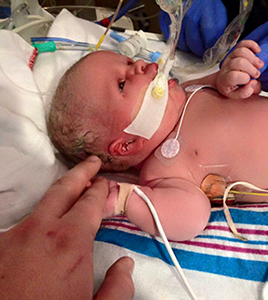
Fannin gave birth to Summer at 39 weeks, on Jan. 23, 2015. As soon as she was born, Summer was taken away to be revived and intubated, but Fannin got to see her briefly before she went to Seattle Children’s.
“When I was finally able to touch her, she opened her eyes and wrapped her little fingers around mine,” Fannin remembers. “We knew each other immediately. She was absolutely perfect.”
For the first few days of her life, Summer was cared for in Seattle Children’s NICU. She had pulmonary hypertension and difficulty maintaining normal oxygen and carbon dioxide levels. After four days, Riehle said she was strong enough for surgery.
“The hardest part was watching her go back to the operating room,” Fannin remembers. “Kim gave us all the information she could, but I still knew some CDH babies didn’t make it.”
Summer’s surgery involved bringing her stomach, intestines and liver into her abdomen. Riehle then covered the hole in Summer’s diaphragm with a synthetic patch to keep the two body cavities separate.
“We got updates throughout the surgery, like ’We finished our prep,’ ‘We’re going to begin now,’ ‘We’re halfway through the surgery,’” Fannin remembers. “That really helped calm our fears.”
Thankfully, Summer’s surgery was a success. After six weeks in the hospital, she was finally able to go home.
“For six long weeks we called Seattle Children’s home,” Fannin said. “We became a family there. In so many ways, leaving was bittersweet. We were leaving behind a life we started, expert care and friends we made within the walls. But moving on to live the life we had planned all along was like nothing I can put into words. We were nervous and excited and ready to be a family of three.
Beyond surgical expertise

While Summer’s hernia was repaired, she still required significant follow-up care from various specialists in Seattle Children’s CDH Program — a multidisciplinary team that cares for CDH patients before birth, through their surgery and into adolescence.
CDH is a complex disease that affects many interconnected organ systems: lungs, heart, GI tract, brain and others,” Dr. Rebecca Stark, CDH Program director, said. “Having a team of specialists working together has led to better patient outcomes.”
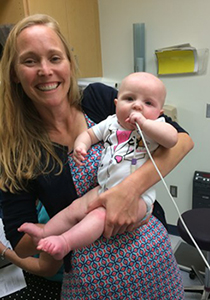
Fannin says the follow-up care Summer receives is one of the primary reasons she recommends Seattle Children’s to other families with a CDH diagnosis.
“Despite everything she’s been through, Summer loves going to Seattle Children’s,” Fannin said. “She loves her doctors and everyone who has helped create this wonderful space for children like her.”
A bright future
Summer still faces health challenges caused by her CDH, but Fannin says she is thriving.
Now 6 years old, Summer adores her little brother, attends virtual kindergarten and will soon try playing soccer, despite her left lung’s limited function.
“Summer is an energetic and compassionate human being,” Fannin said. “I can’t imagine our life without her. It would be easy to wish away some of the hard times, but I don’t know that I would. She is so amazing exactly as she is and makes me proud every single day.”

