 Gary Bradford was a healthy 2-year-old until 2009, when what first appeared as seasonal allergies developed into a much more serious health condition.
Gary Bradford was a healthy 2-year-old until 2009, when what first appeared as seasonal allergies developed into a much more serious health condition.
After spending time outside in the pollen-filled air on a spring day, Gary’s face swelled and he developed a rash on his arm.
Three weeks later, the symptoms became more severe as he developed high fevers, sores inside his mouth and muscle weakness that was so bad he couldn’t get up when bending down to pick up his favorite toy.
Gary’s parents took him to Seattle Children’s where he was hospitalized while doctors searched for a diagnosis. After three days, he was diagnosed with juvenile dermatomyositis (JDM), a rare autoimmune disease affecting three out of every one million children.
“His immune system was basically attacking his skin and muscles like they weren’t supposed to be there,” said Erika Bradford, Gary’s mother. “It was scary getting this diagnosis, but we were lucky to land at Seattle Children’s because they picked right up on it.”
A treatment helps Gary thrive
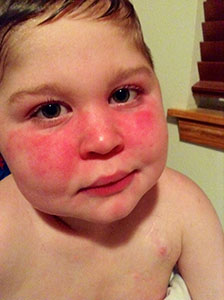
Patients with JDM often experience fatigue, skin rashes, fevers, swelling, abdominal pain, and muscle inflammation that cause muscle weakness and pain, making it difficult to walk and swallow. About 20% to 30% of patients with JDM, including Gary, also develop calcium deposits under their skin, which can be extremely painful.
Symptoms for many children with Gary’s condition improve and go into remission after about two years of treatment, said Bradford. This was not the case for Gary.
Nearly 10 years since his diagnosis, he still requires infusions every two weeks and will likely need these treatments throughout his life. That’s more than 260 infusions since he was diagnosed with JDM, and each takes eight to 10 hours to administer.
An infusion is a way to give treatments, such as medicine or blood products, through the vein by IV or a central line. At Seattle Children’s, infusions are offered to patients with health conditions like blood diseases, cancer, gastrointestinal problems, genetic disorders, immune system disorders and rheumatic conditions.
In more recent years, the Infusion Services team has also been integral in the administration of T cells as part of the immunotherapy clinical trials for patients with certain types of cancer.
“Gary’s treatments have made it so that he can walk, eat, go to school and do most of the normal things kids do,” said Bradford. “I truly believe if it wasn’t for Seattle Children’s, my son wouldn’t be here today.”
Expert care close to home

Over the last few years, Seattle Children’s has made a commitment to expanding infusion services at regional sites.
Infusions are offered to patients at Seattle Children’s hospital campus, at the Bellevue Clinic and Surgery Center, and at Seattle Children’s South Clinic in Federal Way.
To reach more patients, the South Clinic added two additional infusion chairs in June, doubling their capacity. The hospital campus and Bellevue also offer weekend hours, and all three clinics have evening hours available so children don’t have to miss much school.
For the regional sites, telemedicine is available four days a week, allowing the Infusion Services team to connect virtually with the on-call provider if any issues arise. This helps nurses feel more comfortable caring for higher acuity patients, said Lisa Guenser-Onstot, supervisor of Infusion Services.
“With the support of our amazing team of family service coordinators, we’ve made a big push over the last year to get patients to have infusions closer to home,” said Guenser-Onstot. “In addition to keeping up with increasing patient volumes, traffic can be challenging causing patients to sometimes miss their infusions. Many of these patients could get to Bellevue or Federal Way more easily than coming to Seattle.”
The Bradford family fits that description.
Gary and his family live in Bonney Lake, Wash., nearly 50 miles from the hospital campus. On average, Bradford says she and Gary would spend a total of four hours driving to and from infusion appointments every two weeks. For most appointments, Gary would stay overnight as an inpatient because the car trip and lengthy treatment were too exhausting.
“My two other children missed their mom and were asking when I was coming home,” said Bradford.
When she learned the South Clinic was opening, she was eager for Gary to receive treatments much closer to home.
“It has been a really big blessing and has changed our lives,” said Bradford.
It now takes the family less than an hour roundtrip to get to and from Gary’s treatments, meaning no more hospital stays every other week.
Gary, now 11, is a social fifth grader who enjoys spending time with his friends and playing sports. Bradford credits Gary’s care team at Seattle Children’s for making that possible.
“Since Gary is going to fight this condition all his life, I’m so glad we have Seattle Children’s,” she said. “The people there are like family.”

