Montana teen becomes first patient at Seattle Children’s to receive the HeartMate II ventricular assist device (VAD) and a heart transplant while being supported with an implantable VAD. He is also the first patient at any pediatric hospital in the Pacific Northwest to leave the hospital with a VAD while waiting for a heart transplant.

Adam Kingsbury went to see his family doctor for what he thought was a bad cold. It was there that Adam, a 16-year-old from Stevensville, Mont., was diagnosed with asthma and sent home with a prescription for an inhaler and orders to take it easy.
After a few weeks, Adam’s symptoms didn’t improve. He was having trouble breathing so his mom took him back to the doctor where it was discovered that Adam had an abnormal heart rhythm. At age 5, Adam was diagnosed with myotubular myopathy, a condition that makes the heart muscle weak. Because of this, his care team knew it was extremely important to find out what was causing the abnormal heart rhythm right away.
The clinic called Seattle Children’s Montana-based pediatric cardiologist Bruce Hardy, MD to examine Adam’s heart. An echocardiogram revealed that Adam was suffering from cardiomyopathy, a condition which causes the heart to lose its pumping strength. Adam’s heart was failing and he would likely need a heart transplant. Within three hours of seeing Dr. Hardy, Adam and his mom, Kate, were on a medical transport plane to Children’s main campus in Seattle where Adam’s condition could be best treated.
“In a matter of hours, I went from thinking I was having issues with asthma to learning that I may need a heart transplant. It was a lot to take in and it really made me reflect on life,” said Adam. “Ironically, this all happened the day before I planned to meet my dad and brother at Glacier National Park for a camping trip.”
“Adam’s mom called me just before they boarded their plane to Seattle as I was getting ready for our camping trip,” said Adam’s dad, Chad, who lives in Boston. “She said, ‘change your flight and come to Seattle, Adam’s heart is failing and we’re on our way to Seattle Children’s Hospital now.’ That was the last thing I expected to hear.”
When Adam arrived at Children’s, he was immediately taken to the Cardiac Intensive Care Unit where his treatment by the Children’s Heart Center team began.
For the first two weeks, Adam’s care team treated him with medications that they hoped would make his heart stronger and possibly decrease his chances of needing a transplant. However, this was not the case.
Adam’s heart got progressively weaker and his kidneys started to fail. A new heart became the only option for saving Adam’s life. The problem was Adam needed a heart immediately and one wasn’t yet available.
It was at this point that Adam was added to the heart transplant waiting list with the United Network for Organ Sharing (UNOS), the group responsible for distributing organs in the U.S.
A bridge between a failing heart and a new heart
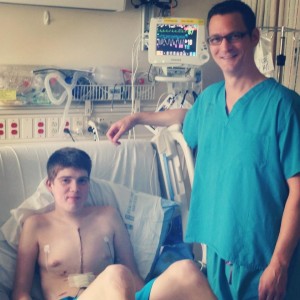
Adam’s care team determined he was the perfect candidate for a VAD to support his heart while he waited for a heart transplant. The VAD, made by Thoratec Corporation and called the HeartMate II, is a fully implantable device that can be used to support patients with severe heart failure.
The device would soon become Adam’s life bridge between his failing heart and new heart. It would serve the functions of a healthy heart by pumping blood through Adam’s body until he received a transplant.
“Adam, his dad and I met with the care team and together we decided the HeartMate II was Adam’s best option,” said Kate. “He was dying and this was our best chance of saving him.”
In addition to saving his life, the HeartMate II would also give Adam an opportunity to be discharged from the hospital while waiting for a new heart. This would make Adam the first patient at any pediatric hospital in the Pacific Northwest to leave the hospital with a VAD while waiting for a heart transplant.
Adam becomes Children’s first patient to receive the HeartMate II
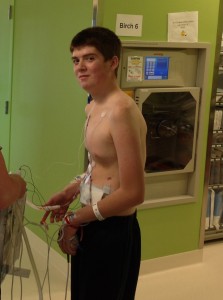
On July 8, Adam became Children’s first patient to receive a HeartMate II VAD implant, and also the first patient at any pediatric hospital in the Pacific Northwest to receive the device spanning the states of Alaska, Hawaii, Idaho, Montana, Oregon and Washington.
Adam’s VAD surgery took three hours. The surgery was performed by Michael McMullan, MD, surgical director of Children’s Cardiac Transplant program and director of Mechanical Cardiac Support, and Jonathan Chen, MD, division chief for Pediatric Cardiothoracic Surgery and co-director of the Heart Center.
“Adam did very well in surgery and the HeartMate II VAD began working immediately as planned,” said McMullan. “It provided enough blood flow to his body to keep him alive.”
“Before the surgery, I was tired most all of the time. Upon waking up from surgery, I had more energy and just felt better all around aside from the physical pain that comes along with having heart surgery,” said Adam.
Over the next few weeks, Adam’s care team monitored his heart to make sure it was responding well. Adam and his family also received the training they would need to eventually leave the hospital with the VAD.
Adam leaves the hospital and attends a baseball game while waiting for a heart transplant

Adam was discharged from Children’s on August 8 to stay at the Ronald McDonald House until a new heart became available.
He and his mom did what they could to regain some normality in their lives. Adam being an avid baseball fan, ventured to Safeco Field for a Mariner’s game with his mom. His Stevensville friends surprised him with a “Get Well Soon” message on the Mariner’s big screen. They also attended an outdoor movie to watch “Sandlot” and Adam even shot some hoops at the park — all while being kept alive by the Heartmate II.
Adam’s transplant coordinator, Keli Morgan, was happy to see Adam get the opportunity to leave the hospital.
“The time between being added to the national heart transplant waiting list and receiving a heart can take months. The wait can be tough for patients and their families,” said Morgan. “To see Adam being discharged was truly remarkable.”
HeartMate II increases survival rates and improves quality of life

The HeartMate II was developed with the goal of providing circulatory support for a broad range of advanced heart failure patients for up to several years. It improves survival rates and a patient’s quality of life compared to other VADs.
Its small size and internal pump equate to an increase in mobility for the patient and a decrease in stroke risk. Its size and durability also make it suitable for a wider range of patients, including some children.
“The HeartMate II provides patients with a very high likelihood of getting to transplant, surviving transplant and doing well after transplant,” said McMullan.
It replaces the need for constant medical intervention, so some patients can even leave the hospital while waiting for their new heart. For the most part, patients can participate in their normal activities like going to school or going for a walk. Without the device, patients remain in the hospital dependant on medications until a new heart becomes available. The HeartMate II consists of four components – a pump, tube, control module and battery pack. The pump is inserted into the chest where it attaches to the heart and regulates the heart’s pumping functions. The tube connects the pump to the externally-worn display module, which is preprogrammed by the patient’s care team to control the vigor and rhythm of the pump. The battery pack is also worn outside the body. The pump is about the size of an iPhone, the display module the size of a six-inch Subway sandwich, and the battery pack is equivalent to the shape of a king-size Hershey candy bar.
To qualify for the device, a patient must be in need of a new heart due to significant heart failure. They must also have at least a 1.3 body surface – the size of an average 12-year-old.
A new heart
Adam’s new heart arrived quickly – a week after he left the hospital.
“I was at the Ronald McDonald House building a railroad set for some of the kids when we got the call that a new heart became available,” said Adam. “I called my dad to let him know so he could get back to Seattle.”
“I had total confidence that Adam’s transplant would be successful. Adam’s team had done an amazing job up to this point including with the VAD. The expertise and care of the Children’s team coupled with all the love, support and prayers from our family, friends and community, made me feel at ease about the whole process,” said Kate.
The heart transplant went as planned and without complication. McMullan performed the surgery with his partner, Lester Permut, MD.
“Adam woke up from surgery with pink cheeks which meant his heart was pumping blood like it was supposed to. Hours later he was joking with the nurses. At that point, I knew our prayers had been answered and Adam would soon get to go home,” said Chad.
On August 28, Adam was discharged from Children’s and plans to return to Stevensville before Thanksgiving. Until then, he will stay in Seattle with his mom while he receives outpatient care at Children’s.
While Adam recovers from his heart transplant surgery, he remains hopeful for the next phase of his life – returning to Stevensville to finish out his junior year of high school with his friends. Adam also looks forward to getting back to work as a courtesy clerk at Super1 Foods and working on his truck.
“Adam’s new heart gives him a chance at a normal life. I’ve been so proud of his maturity throughout the process and am excited to see what’s next for him,” said Chad.
Advice from Adam and his family
“I want families facing heart failure to know that things will get better after VAD surgery. I got used to the HeartMate II and regained some normality in my life while waiting for my new heart,” said Adam.
“My care team at Children’s was always so nice and friendly and my room in the Critical Care Unit was big and bright with a great view. I really enjoyed the TV service where I could play video games and watch on-demand movies to help pass the time,” he also said.
“My advice is to feel okay about relying on your community for support,” said Kate.
Super1 Foods, also Kate’s place of work, raised $10,000 with a hot dog barbeque event. Chad’s work, Harvard Business School, also helped raise money to support the family. Kate said their church was also a great support throughout the process.
“I didn’t realize so many people cared about us,” said Adam. “From the nurses, doctors and the rest of my care team at Children’s, to our community in Montana who sent cards, food, prayers and well wishes – I am thankful for it all.”
The future of mechanical heart assist devices: What’s next at Children’s
Children’s recently was selected as a test site for several new mechanical heart assist devices, sponsored by the National Institute of Health’s National Heart, Lung, and Blood Institute (NHLBI.) The trial, slated to begin in 2014, will focus on finding the most suitable devices for infants and young children.
According to the NHLBI, each year in the U.S., about 1,800 infants die as a result of congenital heart defects and another 350 develop heart disease, which leads to heart failure for many. Each year, approximately 60 infants and kids under the age of 5 who are placed on the heart transplant waiting list die before receiving one. Mechanically assisted circulatory support devices could be used to sustain these young patients as they seek to recover or wait to receive a heart transplant.
In addition to the HeartMate II, Children’s will continue to offer external VADs such as the Berlin Heart to very young children, and the Total Artificial Heart replacement for older children with life-threatening heart failure.
To arrange an interview with Adam, his parents, or a member of Adam’s care team, please contact Children’s PR team at 206-987-4500 or at [email protected].

