
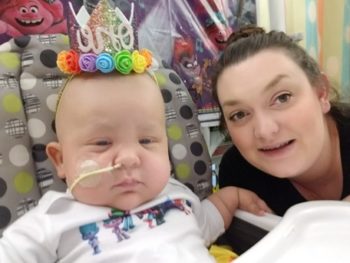
Two years ago, Meagan stood in a hospital room at Seattle Children’s cradling her 1-year-old daughter, Harper, against her chest. Her fiancé, Josh, huddled close to them and kissed the thinning hair on top of their baby’s head.
A feeding tube was routed through Harper’s nose and her eyes were brimming with tears. Exhausted, she snuggled into her mom’s arms as a photographer took their picture.
Meagan and Josh feared those would be the last photos taken of their baby girl.
“It was a roller coaster”
Six months before, Harper became seriously ill. After multiple visits to their pediatrician in Yakima, Meagan took her to an emergency room where blood tests revealed Harper had leukemia.
“It was shocking,” Meagan says. “Thirty minutes later we were on an emergency flight to Seattle Children’s.”
The family didn’t return home for nearly two years.
The type of leukemia Harper had — acute lymphoblastic leukemia (ALL) — is typically harder to treat and has lower survival rates when it occurs in infants who are less than a year old.
Harper’s case was exceptionally challenging. She didn’t respond to standard chemotherapy, even after providers added a medication designed to sensitize her leukemia to the treatment.
Her care team, which included Seattle Children’s High-Risk Leukemia Program, believed a stem cell transplant would give Harper the best chance of surviving, but they had to eliminate the majority of her leukemia cells first.
Drs. Kasey Leger and Brittany Lee, Harper’s primary oncologists, started her on a novel immunotherapy medication, called blinatumomab, which effectively destroyed many of her ALL cells.
Unfortunately, two weeks later, the team discovered some of Harper’s ALL cells had morphed into a different blood cancer — acute myeloid leukemia (AML). This rare occurrence, called lineage switch, occurs in less than 5% of infant ALL cases.
“It was a roller coaster,” Josh says. “She didn’t do anything they expected her to do. It felt like every day we had to come up with a new plan.”
Drs. Leger and Lee gave Harper a different kind of chemotherapy that destroyed the new AML cells. Still, some of her ALL cells remained, so the team gave Harper blinatumomab again which finally suppressed her cancer enough for her to have a stem cell transplant just before her first birthday.
The team had done everything they could to get Harper healthy enough for a stem cell transplant, hopeful it would be the treatment that finally cured her. Tragically, Harper’s leukemia was back less than a month later.
“When leukemia comes back so soon after transplant, patients have very few treatment options, if any,” says Dr. Corinne Summers, Harper’s stem cell transplant specialist. “Many patients will not survive long term.”
Harper’s parents were terrified they were going to lose her.
“Her bone marrow was packed with leukemia,” Josh remembers. “You could tell the life was slipping out of her and she just looked like it was going to be the end.”

They struggled to decide if they should continue treatment.
“How do you know when enough is enough?” Meagan says. “When do you say, ‘We can’t do this to her anymore?’ Harper couldn’t tell us how she was feeling, so it was all our decision.”
A turning point
Meagan and Josh worked closely with the care team to decide what to do next.
“Those conversations were emotional for all of us,” says Dr. Lee. “Thankfully, we had a close, trusting relationship with their family and were able to give recommendations that reflected what they wanted for their daughter and what they felt was most important.”
After much consideration, Meagan and Josh decided Harper was strong enough to continue treatment.
Drs. Leger and Lee filed a compassionate use request with the Food and Drug Administration to give Harper an investigational chemotherapy drug called venetoclax. Unfortunately, the treatment didn’t work.
Collaborating with the family, the team decided to try giving Harper blinatumomab one more time. There was no evidence suggesting the medication would work so soon after a bone marrow transplant and with such a high burden of leukemia, but within a week it eliminated 98% of Harper’s cancer cells.
“Family is a critical piece of the team, Dr. Leger says. “And Harper is fortunate to have amazing parents who were at her bedside 24/7 and had a beautiful way of advocating for her. They challenged us to leave no stone unturned and partnered with us throughout her treatment to keep figuring out a way forward.”
The power of research
With Harper’s leukemia under control, the team searched for a way to wipe out any remaining cancer cells and keep her disease from coming back. Doctors in Children’s Cancer and Blood Disorders Center lead national research groups such as the Children’s Oncology Group, so they have access to trials around the world. However, Harper’s care team found the best treatment for her was at Seattle Children’s Hospital, in partnership with Seattle Children’s Therapeutics.
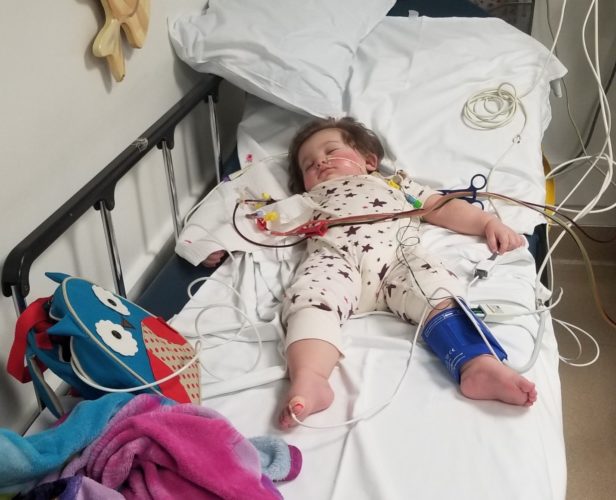
Harper was enrolled in one of Children’s T-cell immunotherapy clinical trials. The treatment involves re-programming a patient’s T cells (a type of white blood cell) to target and destroy their cancer cells.
After her T-cell therapy, Harper was finally in remission.
Meagan cried with relief when she found out. “Harper would not be here right now if it wasn’t for everybody at Seattle Children’s,” she says. “From day one, they’ve been comforting and compassionate. They bend over backwards to keep families involved and helped us fight for our child.”
To keep her in remission, Harper was given six antigen-presenting cell “boosters,” which kept her reprogrammed T cells circulating through her blood longer. She received the last booster earlier this year and is still in remission today.
“Harper had a very unique disease in that her leukemia manifested as both ALL and AML,” says Dr. Leger. “Thankfully, we have team members with deep expertise in each of those diseases. Having internationally recognized chemotherapy, transplant and immunotherapy specialists on our team allowed us to be creative with her care when she needed to go beyond the standard pathways.”
The risk of relapse
Today, Harper is a joyful, boisterous 3-year-old who loves experimenting with musical toys and splashing around in her bath or kiddie pool. One of her favorite things to do is grab Meagan by the hair and squish their faces together.
Because of the treatments Harper received at such a young age and the extended time she spent in the hospital, Harper is behind on some developmental milestones like speaking and walking. Still, Meagan and Josh say she’s catching up.
“She’s starting to bloom and take off and it’s so nice to see,” Meagan says. “At the same time, we can’t get too comfortable. We know how relentless her disease is and that it could come back one day.”

Harper’s family encourages community members to support cancer research at Children’s so that new treatments can be developed for Harper and other kids like her.
“Without donors, Harper probably wouldn’t be alive right now,” Josh says. “The treatments she had were developed in just the last few years. If people don’t step up and donate, those programs aren’t there. Those drugs aren’t invented. Cancer treatment has come a really long way and that’s because of donors stepping up to make that happen.”
Learn more about Seattle Children’s High-Risk Leukemia Program and Cancer and Blood Disorders Center
Resources
- Acute Lymphoblastic Leukemia – Seattle Children’s Hospital (seattlechildrens.org)
- Acute Myeloid Leukemia – Seattle Children’s (seattlechildrens.org)
- High-Risk Leukemia Program at the Cancer and Blood Disorders Center (seattlechildrens.org)
- Statistics and Outcomes at the Cancer and Blood Disorders Center (seattlechildrens.org)
- T-Cell Immunotherapy Overview (seattlechildrens.org)

