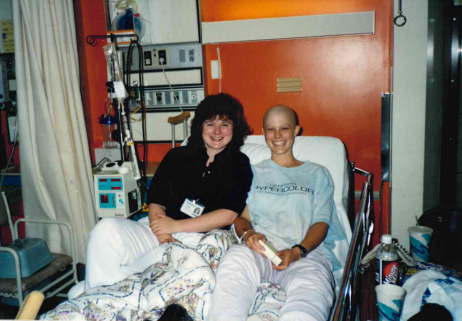Throughout this season’s viral surge, Seattle Children’s Urgent Care team has been hard at work caring for a high volume of patients throughout its four locations in Bellevue, Everett, Federal Way and Seattle. The sites are open 7 days a week, including holidays, and recently expanded their reach by offering virtual urgent care services to […]
On the Pulse
2023 is the Year of the Rabbit, symbolizing courage, kindness and good fortune. While specific celebrations vary across Asian cultures, including Vietnam where they’ll welcome the Year of the Cat, many practices emphasize family and reuniting with relatives. The new year is also a great time to recommit to healthy habits — and try some […]
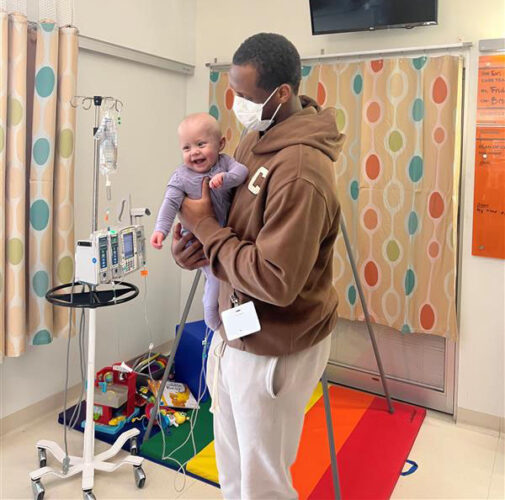
PART FIVE: From witnessing exceptional care and compassion given to children in their own lives, to receiving treatment first-hand, this weekly series features Seattle Children’s employees and the life experiences that drove them to pursue careers in healthcare. During a family vacation in 1993 at Lake Chelan, WA, 12-year-old Jesse Giordano started experiencing severe flu-like […]
Beginning Jan. 18, 2023, Seattle Children’s is offering telemedicine for urgent care services for the first time. Virtual Urgent Care will expand services beyond our four in-person urgent care locations in Seattle, Federal Way, Everett and Bellevue to any eligible patient in the state of Washington. This new service will bring care even closer to […]
Seattle Children’s has teamed up with primary care pediatricians in the Puget Sound region to implement a new approach to address the growing youth mental health crisis. Seattle Children’s Care Network (SCCN) and Seattle Children’s Psychiatry and Behavioral Medicine launched a Pediatric Integrated Behavioral Health Program in 2020 to provide children and their families with […]
As featured in Good Growing Studies consistently show that less than half of all school-age kids get enough sleep most weeknights. While the most recognized consequence of inadequate sleep is daytime sleepiness, children commonly manifest their sleepiness as irritability, behavioral problems, learning difficulties and poor academic performance. Some sleep disruptions are normal and are connected […]
Seattle Children’s patients and families were surprised this holiday season when some exciting visitors stopped by – Geno Smith, Seattle Seahawks quarterback, Michael Dickson, punter, Joey Hunt, center, and Jalen McKenzie, tackle. The players delivered teddy bears, signed autographs, played video games, and shared special moments with our patients and their families.
The new year is an ideal time for parents to renew their commitment to using positive reinforcement with their children. Positive reinforcement includes specific and immediate praise when spotting a child doing something kind or helpful. This kind of approach is also particularly beneficial if the action is the opposite of a problem behavior that […]
PART FOUR: From witnessing exceptional care and compassion given to children in their own lives, to receiving treatment first-hand, this weekly series features Seattle Children’s employees and the life experiences that drove them to pursue careers in healthcare. In 1991, Becky Greenway was a 17-year-old student facing chronic knee pain throughout her senior year of […]
As many families prepare for their annual holiday celebrations and family gatherings, this year’s plans look very different than last year for 3-year-old Harper and her parents, Meagan and Josh. In 2019 just a few months before Christmas, Harper was transported to Seattle Children’s on an emergency flight from Yakima, Wash. after blood tests in […]