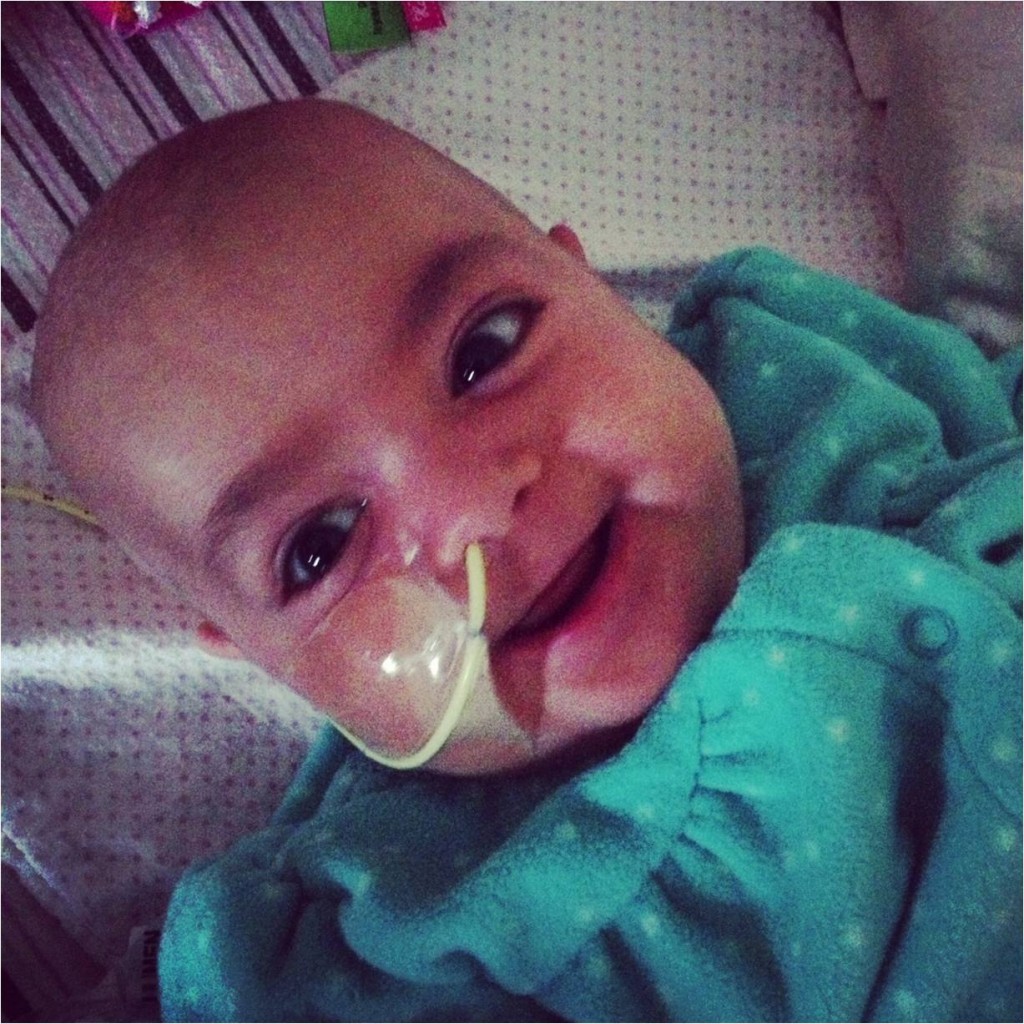
Depression occurs in up to 14 percent of kids ages 13 to 17 and can lead to risky sexual behaviors, substance abuse or even suicide. Unfortunately, few teens utilize mental health services that can help manage depression symptoms. But a study by Seattle Children’s Research Institute suggests parents play a strong role in helping teens […]
On the Pulse
Like many of his patients, Tim Brei, MD, lives with spina bifida, a birth defect of the spinal cord. He understands the challenges facing his patients and their families because he faces them, too. After 24 years at the Indiana University School of Medicine, Brei moved west in August 2013 to join the Developmental Pediatrics […]
In 2014, the Seattle Children’s Research Institute will implement life-saving projects, begin new studies to keep children safe and continue searching for ways to prevent and cure diseases that threaten some of our youngest patients. We are celebrating the New Year by highlighting some of the work that has researchers excited about 2014. Looking forward […]
At age 4, Natalie Merlo was diagnosed with a facial condition that left her feeling self-conscious and very different from other people. While growing up, she even avoided having her photo taken. Through the work with her care team at Seattle Children’s Craniofacial Center, Natalie has gained confidence, has happily accepted who she is and […]
UPDATE: The competition continues Seahawks fever is still in the air! As of Jan. 24, Seahawks fans have raised more than $257,000 for UCSF Benioff. And 49ers fans have raised more than $157,000 for Seattle Children’s. Thank you 49ers fans and Seattle’s 12th man for supporting our patients and families. With the support of the […]
Thousands of children are diagnosed each year with hydrocephalus, a condition in which the body can’t properly drain the fluid that builds up around the brain. Physicians commonly treat hydrocephalus by implanting a shunt in the brain to carry the excess fluid to other parts of the body. Shunts save lives, but too often they […]
AJ Hwangbo was a happy-go-lucky 6-year-old without a worry in the world until mid-November when he developed a life-threatening heart condition. While specialists at Seattle Children’s Hospital helped AJ heal physically, the young boy struggled to bounce back emotionally. But, AJ’s joyful spirit returned after hospital staff arranged for him to meet his hero – […]
As the New Year approaches, we’re taking a look back at a post from last year to help families make SMART resolutions. Seattle Children’s Dr. Mollie Grow offers advice for making resolutions with your family that will last well into 2015. The new year marks a time for reflection and change, a time for new […]
The faster medical research moves the more quickly cures can be found for countless children’s diseases. But one of the greatest delays researchers face when trying to solve medical problems is finding enough patients to study. “Enrolling patients in a clinical trial to study a rare condition could take years,” said Mark Del Beccaro, MD, […]
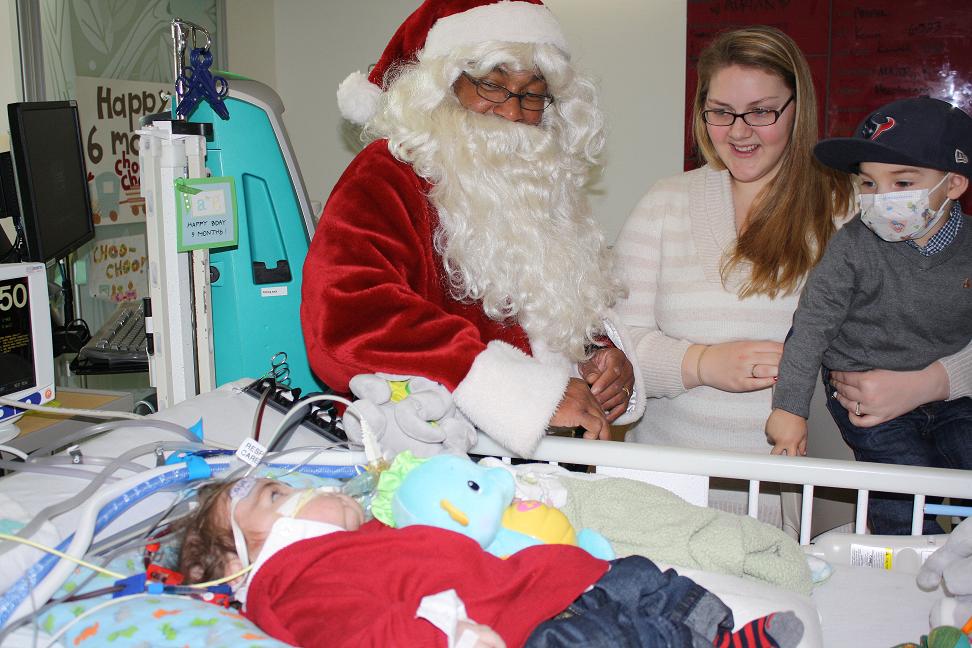
Being sick is never fun for a child, and spending time in a hospital can be especially difficult for families during the holidays. Children sometimes wonder if Santa will be able to find them come Christmas day. But at Seattle Children’s, there’s no need to worry. Every year, Santa makes a very special visit to […]