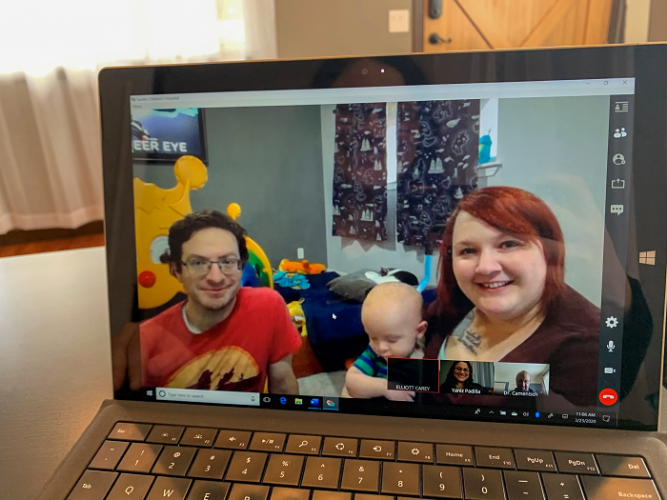
 Jessica Carey’s family has received care for her twin sons at the Seattle Children’s Autism Center for about four years. She transitioned to telehealth in February due to the COVID-19 pandemic.
Jessica Carey’s family has received care for her twin sons at the Seattle Children’s Autism Center for about four years. She transitioned to telehealth in February due to the COVID-19 pandemic.
Telehealth refers to a broad spectrum of remote technological healthcare services, which may include non-clinical services, while telemedicine is the practice of delivering clinical care from a distance via technology.
“At first the idea of telehealth seemed daunting because it’s a lot of work for parents, but it’s actually a really nice way to be able to move practice to home from a clinical setting while still receiving support from a professional,” Carey said. “It also saves on travel time and expenses which is really positive.”
Since many appointments were cancelled or postponed, she added, “Being able to at least see our providers at Seattle Children’s helps keep consistency in my boys’ days.”
Carey is just one of thousands of families who have recently experienced Seattle Children’s rapidly expanded telehealth services to ensure children get the medical care they need during an era of travel restrictions and “Stay Home, Stay Healthy” orders to stop the spread of the coronavirus.
According to Seattle Children’s Dr. Yaniz Padilla, clinical psychologist, this is especially the case for families receiving care through the Autism Center.
“Families of children with autism have preferred continuing to receive services via telehealth instead of pausing services,” she said. “Telehealth has allowed us to walk parents through daily activities in their home and help provide needed structure. With this technology, providers can coach the parent through difficult situations, giving them the opportunity to apply clinical techniques in real time.”
Telehealth firsts during COVID-19

Seattle Children’s piloted home telehealth visits in April 2018 with a select number of patients, a few specialties, and plans to scale telehealth slowly with a strategic plan. The plan called for rolling out platforms, technology, infrastructure and to standardize clinic equipment and processes. But the COVID-19 pandemic catapulted telehealth, telephone care and telework options to an expedited timeline. Starting in March 2020, Seattle Children’s switched many in-person visits to telephone calls, and by April 2020 clinics across the system were using telehealth visits with at- home videoconferencing in earnest.
Seattle Children’s rapid expansion of telehealth included training staff, acquiring and deploying technology and software services, and implementing telehealth options across various clinical services – both inpatient and outpatient. By mid-April, Seattle Children’s was seeing 76% of ambulatory patients via telehealth.
“Telehealth is here to stay,” said Russ Williams, Seattle Children’s chief operating officer. “We were already working on it and got an unexpected leap forward due to COVID-19. Our families want it, and our goal is to have our clinics fully open and a robust telehealth program for our outpatient specialty care.”
According to Williams, patient visits reflected the rapid spin to telemedicine and telephone ambulatory care. During the first three weeks of April there were 2,234 telemedicine sessions in our outpatient clinics, up from 237 in January 2020; and there were 3,822 telephone care calls, up from 17 in January.
During the month of April nearly 80% of all visits were provided via telehealth.
Telepsychiatry: Early adopter
In less than 10 days (between March 10-18), Seattle Children’s Psychiatry and Behavioral Medicine team converted 95% of in-person, outpatient mental health appointments to telehealth.
Seattle Children’s manager of ambulatory psychiatry, Dave J. Hall, worked diligently to get the more than 100 outpatient psychiatric providers trained to provide mental health services via telehealth. The mental health clinics he manages usually see more than 750 patients per week and despite the massive juggling act to pivot from offering in-person appointments to conducting therapy from a provider’s home to a patient’s home, he sees this as a tipping point for telepsychiatry.
“COVID-19 has led us to embrace a technology that has existed for years but was underutilized,” Hall said. “As our providers become more proficient facilitating telehealth services, this might be the moment that transforms how we provide mental health care in the future.”
Many providers and patients welcomed the transition to technology and adapted easily to the new format. For example, Dr. Tyler Sasser, Seattle Children’s child clinical psychologist, was facilitating two separate groups of 10 families in which two-hour sessions are offered through an 18-week course. They were about half way through the course when COVID-19 hit.
“Telehealth was immediately appealing to me. It’s great for people who live out of the region and for those who don’t have flexibility in their work schedule,” Sasser said. “Telepsych has to become the norm.”
Sasser was one of the first at Seattle Children’s to offer telehealth for group sessions. He had already been doing telehealth through the pilot program, so he was comfortable with the technology. After testing several telehealth platforms, he learned Zoom for Healthcare has a tool that enables breakout sessions where he can assign members of the group to huddle into smaller groups for activities. This was valuable for group sessions so everyone has an opportunity to participate in topic discussions.
“Ethically, it’s the right thing to do,” said Sasser. “We need to be available to provide care for our patients wherever they are, especially during a time like this.”
While Seattle Children’s has been able to transition existing patients into telehealth, families in Washington State seeking to establish care can use the Washington’s Mental Health Referral Service for Children and Teens to find a provider in their network.
Cultivating TeleEquity
Seattle Children’s has come a long way in a short timeframe, but there is more work to do according to telehealth medical director Dr. Mark Lo. There are various barriers to telehealth, equity being one of them.
In the case of telehealth, the ability to pay is only a piece of the equation. Although telehealth can save time traveling, looking for parking and time away from work, it assumes the patient has a private space with access to the internet.
“We know not everyone has access to digital devices or wifi capability, so we are looking at ways to overcome those barriers. It’s a challenge,” Lo said.
One of the ways Seattle Children’s is working to improve equity and access to telehealth is through a new program at the Odessa Brown Children’s Clinic (OBCC).
“At this point, all of healthcare is playing catch-up to telemedicine,” said Vu Tran, a nurse practitioner at OBCC. “The biggest limitation for many is the lack of hardware – the computer or mobile device with a built-in camera and a microphone – that makes it possible for us to speak and visit with our patients.”
Lo and his team are working with Tran to establish telehealth “kiosks” at OBCC for patients and families who may not have access to equipment, the internet or the space at home for private visits. These kiosks will be set up in empty visit rooms at OBCC to provide a location for patients and families to have telehealth visits with their providers at another Seattle Children’s location or who may be completing telehealth visits from home due to COVID-19.
“By utilizing and expanding telemedicine, we can continue to serve all our families in an equitable way to meet them where they need it,” Tran said.
For those able to access telehealth services at home, a telehealth pilot program has completed more than 270 visits across OBCC’s medical and mental health services.
“Feedback from families has been positive overall. Families appreciate the ability to connect with their provider safely during this time and also like that Zoom is relatively user-friendly and familiar,” said Anisa Khaleel, OBCC business operations manager.
OBCC has also been using Zoom for Healthcare to connect with patients who typically visit the Sickle Cell Clinic at OBCC; these are some of the most medically and socially complex patients and families.
“We hope to continue this model of care into the future as it allows us to connect with families who would like to visit us in clinic but find it difficult due to busy family schedules, lack of childcare for siblings or transportation issues,” Khaleel said.
While telehealth doesn’t resolve all of the barriers, it does address many of them.
“Telehealth takes geography out of the equation, and we can provide our standard of care to pediatric patients no matter how far away they are,” Lo added.
Dr. Shaquita Bell is credited as the physician champion for this work at OBCC. She helped onboard providers to Zoom and her leadership was integral to getting telemedicine up and running quickly.
The future of telehealth
Now that telehealth visits are available for any pediatric health condition that can be treated remotely at Seattle Children’s, Lo has been thinking a lot about what innovations resulting from the pandemic will remain once things begin to return to normal.
“Even though I am one of telehealth’s biggest proponents, I recognize it isn’t always the best option for complex patients who need hands on care. There are still many cases where we need a physical exam or vital signs to make important care decisions,” Lo said.
Still, he believes telehealth has the potential to positively impact many areas beyond patient care – from decreasing transportation for the betterment of the environment to reducing costs associated with parking, gas and the extra time needed to go to an in-person appointment.
“It’s neat to see all the specialties trying telehealth out,” Lo said. “With all the innovation happening amidst the rapid adaption and adoption, I believe this will stand out as one of the most remarkable moments in our telehealth efforts.”
Starting in June, Seattle Children’s will use MyChart for telehealth visits. This change is to ensure visits are HIPAA compliant, but it also improves workflow for patients, families and providers. Solutions are needed and are being discussed for families that decline to use MyChart, the small population of foster parents and for those select confidential patients.
Nearly all Children’s specialties are performing some level of telehealth and have processes in place to accommodate patients.
Resources:
- Seattle Children’s Telemedicine
- Seattle Children’s Telehealth Program Offers Modern-Day House Call With a Twist
- Like Mother, Like Daughter: Sharing a Craniofacial Care Team and Condition

