
This summer, Seattle Children’s hosted a reunion for patients who have one unique experience in common: Extracorporeal Membrane Oxygenation (ECMO) played in key role in saving their lives. Patients, families, doctors and nurses gathered to celebrate the 25th anniversary of Seattle Children’s use of ECMO, an advanced life-support therapy that can replace heart and lung function when these organs fail or need to rest. ECMO is used for a range of life-threatening medical conditions and complications, and Seattle Children’s has been named a Center of Excellence by the Extracorporeal Life Support Organization because of its expertise with technologies such as ECMO.
“Seeing all the kids that ECMO helped save means the world to our doctors and nurses,” said Dr. Michael McMullan, Seattle Children’s Director of Mechanical Cardiac Support and Extracorporeal Life Support (ECLS).
Over the past 25 years, Seattle Children’s ECLS program has touched the lives of more than 700 families. Here we share the stories of a few of these patients – from a cheeky baby to a recent law school graduate – who came together to share their experiences and celebrate where they are today.
Jude Xenakis
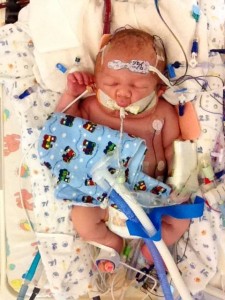
When Jude Xenakis was born in September 2014, it was clear immediately that something was wrong. He had severe meconium aspiration and could not breathe. Meconium aspiration can occur during delivery when a newborn inhales a mixture of meconium and amniotic fluid.
Standard interventions at the hospital where he was born at were not working, so he was transferred to Seattle Children’s. The staff immediately put him on ECMO to give his lungs a break so they could heal. He was on the machine for nine days.
At the ECMO picnic, Jude was in a baby carrier on his dad, Michael Xenakis. The cheeky 10-month-old was eyeing a piece of melon his big sister was snacking on.
“The staff at Seattle Children’s was so supportive while everything was happening,” Xenakis said. “We were lucky to have this program and the technology so close to home.”
Samantha Zimmerman

This summer, Samantha Zimmerman graduated from the Gonzaga University School of Law with honors, and to add an exclamation point to her achievement, she completed her degree early at the age of 23.
Samantha was born with a congenital diaphragmatic hernia (CDH), a condition that occurs when the thin muscle that separates the chest from the belly, called the diaphragm, does not form completely. Organs that should be in the belly can slip through the hole in the diaphragm into the chest. The organs can push on the baby’s lungs, impede breathing and cause high blood pressure.
As soon as mom Stacy Davis delivered Samantha, she was brought to Seattle Children’s and stabilized on ECMO for two weeks, a situation Davis described as “heartbreaking.”
Samantha is now a healthy young woman hoping to develop a career in healthcare law and policy.
“The doctors and nurses at Seattle Children’s are excellent at what they do,” said Davis. “I would tell families dealing with this now to have faith. It’s not easy to see your baby hooked up to machines, and you wonder if everything will be okay. Hang in there and keep your hopes alive.”
Bernardo Dusich de Griego

Bernardo Dusich de Griego, 24, played clarinet in middle school, participated in the Reserve Officers’ Training Corps (ROTC) in high school and enjoys doing jiu-jitsu. These activities require good lungs, something he would not have without ECMO intervention.
“We came from Albuquerque for the ECMO reunion,” said his mother, Rafaelita de Griego. “It’s great to meet the other families who went through this and spend time with the hospital staff who worked to save these kids.”
When Bernardo was still in the womb, ultrasound imaging showed he would be born with a congenital diaphragmatic hernia (CDH), the same condition Samantha was born with.
Griego was told her baby would have a 50% chance of survival. To increase those odds, she decided to travel from Albuquerque and deliver Bernardo in Seattle, where ECMO technology could help save his life. Bernardo was placed immediately on ECMO and stayed on the machine for seven days.
“For the first month and a half of his life I could not touch him because he was in intensive care,” said Griego. “I would tell families who are going through this to have faith and stay by your baby’s side. The waiting was hard on our family, but ECMO really made a difference.”
Natalie Razore

Michelle Razore had a nagging worry in her mind while she was pregnant with Natalie. Her concern? Pertussis, also known as whooping cough. It’s an infectious respiratory disease that can be deadly for babies.
“When I was pregnant, I asked my obstetrician about receiving the Tdap vaccine to protect myself from contracting pertussis and passing it on to my baby,” Razore said. “My doctor said I shouldn’t worry because the chances were very low.”
Unfortunately, her worst fears became a reality: At about 2 weeks old, Natalie contracted whooping cough. Her heart, lungs, and kidneys were failing. She was put on dialysis and ECMO until her heart and lungs were able to work on their own. She was in the hospital for 72 days, and when she went home on Christmas Eve, the staff at Seattle Children’s called her the Christmas miracle.
Natalie, now 4 years old, spent a good part of the reunion perched piggyback on Dr. Thomas Brogan, associate director of Seattle Children’s ECMO services, who oversaw her care.
“The families whose children were treated with ECMO have always been gracious to us,” said Brogan. “Their continuing support at events like this encourages us to work as hard as we can to care for their children.”
Having experienced how infectious diseases that are preventable with vaccines can put a newborn baby into a life and death situation, Razore is now an advocate for vaccines.
“Seeing your child on ECMO is the hardest thing a parent can go through,” Razore said. “We are so fortunate to live in a city with this technology. ECMO has saved many lives and our child would not be with us today if it weren’t for these incredible machines.”
Resources
• Seattle Children’s Heart Center
• From Heartbreak to Hope: Technology and a New Heart Save Hannah’s Life
• The Other Side of the Patient Bed: From Pediatrician to Frightened Parent
• Practice Makes Perfect: Improving a Life-Saving Process Through Simulation
• Lung Liquid Similar to One Used in Movie “The Abyss” Saves Infant’s Life, Doctors Encourage FDA Approval of Clinical Trials Seattle Children’s Heart Center
• VADs 101: Lifesaving Heart Devices

