
There were only a few weeks to go in Jennifer Schow’s seemingly normal pregnancy when her world turned upside down.
She noticed she’d been gaining weight suddenly, more than she thought was expected. Her doctor said everything seemed fine, but something didn’t feel right.
Feeling uneasy, she and her husband got a second opinion and the news they received confirmed their fears.
“I could see the baby’s face on the ultrasound screen,” said Schow. “I joked that it looked like her ear was missing.”
The ultrasound technician became quiet and said she’d be right back. That’s when Schow knew there was something seriously wrong.
Coping with devastating news
After testing and a week of waiting, Schow and her husband received a diagnosis. Their baby had Treacher Collins syndrome, a rare genetic condition that affects the development of a baby’s bones, jaw, skin and face muscles before birth. It occurs in about one of 50,000 newborns, and while the severity of the condition varies, babies born with the condition often have problems breathing, chewing, swallowing, hearing and speaking.
Initially, Schow was told her baby may not survive.
 One week after the diagnosis, on Oct. 19, 2006, Hannah came into the world kicking and screaming.
One week after the diagnosis, on Oct. 19, 2006, Hannah came into the world kicking and screaming.
“We were so happy,” said Schow. “We knew if she was kicking and screaming that she had a chance.”
Hannah was born with small ears (microtia) with no openings, a small jaw, a cleft palate and was missing bones in her face, including cheek bones. She couldn’t breathe on her own, so doctors put a tube in her windpipe called a tracheostomy. She was also given a feeding tube. Hannah spent 73 days in a hospital before she was sent home for the first time.
“There is a wide spectrum for children with Treacher Collins Syndrome,” said Dr. Richard Hopper, surgical director of Seattle Children’s Craniofacial Center. “Some children need very little medical treatment, while others need extensive surgeries. Hannah’s case was severe.”
Treatment for children with Treacher Collins syndrome requires the skills and experience of a multidisciplinary craniofacial team, so the family traveled from their home in Idaho to meet with experts at Seattle Children’s.
Seattle Children’s Craniofacial Center is the largest, most comprehensive craniofacial center in the country, and one of a select few centers in the U.S. that has every discipline necessary to provide customized care to meet the needs of any patient with a craniofacial diagnosis.
“We were determined to find the best care for Hannah,” said Schow.
The journey to find a novel treatment
Over the course of Hannah’s life, caring for her complex medical needs got easier to manage, but she was limited by her inability to breathe without a tracheostomy.
 “For children with a tracheostomy, the burden on a family is immeasurable,” said Hopper. “Parents are constantly worried that something will go wrong because they are prone to complications and infection. Hannah wasn’t able to do the things girls her age should be able to do, like camping or swimming. Removing the tracheostomy would be life-changing for both Hannah and her family.”
“For children with a tracheostomy, the burden on a family is immeasurable,” said Hopper. “Parents are constantly worried that something will go wrong because they are prone to complications and infection. Hannah wasn’t able to do the things girls her age should be able to do, like camping or swimming. Removing the tracheostomy would be life-changing for both Hannah and her family.”
Unfortunately, the standard treatment for Treacher Collins which only changes the lower jaw were unsuccessful in opening Hannah’s airway. Hannah was running out of options.
It seemed that Hannah might never be free from her tracheostomy or feeding tube. It plagued Hopper, so he and his team created a solution: subcranial rotation distraction, a new technique never before done at any center in the world.
“I knew there had to be a better way to help kids like Hannah, and our team was determined to find a solution,” he said.
Using his expertise in distraction surgeries, where devices are used to help a child’s body grow new bone, he devised a complex plan to use unique movements with distraction to rotate Hannah’s entire face below her skull as one piece and open her airway.
“It’s not similar to anything else we do,” he said. “During surgery the entire face is separated from the skull base and the two jaws are locked together. We create a metal hinge at the top of the nose which allows the distraction devices to rotate the entire face and unlock the breathing space behind the jaws and nose. Think of the airway like a narrow tunnel. Treatments in the past have only been able to remove single speed bumps within the tunnel, but air still gets held up somewhere else. Essentially, subcranial rotation distraction takes the whole roof of the tunnel and opens it. The airway results are something we hadn’t seen before”
Not only would the procedure help Hannah breathe without a tube in her neck, but the procedure would also give her something else she’d always dreamed of: cheek bones to protect her eyes.
A new technique, a pioneer

“It was a hard decision, but we trusted Dr. Hopper and the team to try the new technique,” said Schow. “We just wanted what was best for Hannah.”
In August 2015, Hannah underwent the first, and most complex surgery, in a series of three surgeries to complete the procedure.
“First, she needed a halo and her mouth would be wired shut,” said Schow. “Hannah was old enough to know what was in store for her. She practiced trying to talk with her mouth shut to prepare. She stayed so positive. She’s just incredible.”
The first procedure went smoothly. Over the course of the next month, her entire face was slowly rotated forward using a special tool that attached to the external metal devices surrounding her face.
Once her face was in the new position, she underwent a quick procedure to release the wires around her jaw to let her mouth open and close. She wore the devices for nearly three months allowing the bone to heal before they were finally removed in a third and final surgery. Her cheek bones were then placed using bone grafts from her skull.
A dream come true
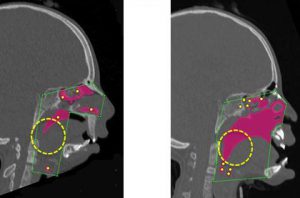
Next up, it was time to address Hannah’s airway and the removal of her tracheostomy – a milestone Schow wasn’t sure would ever be possible.
“Getting her tracheostomy removed had been our hope since she was 2 weeks old,” said Schow. “Living with a tracheostomy is all she’s ever known. Without it she can swim under water, go to sleepovers or play softball for the first time. It’s a dream come true.”
In developing this technique, Hopper was also thrilled with the results he saw in Hannah.
“We knew Hannah’s face would change, but we didn’t think the changes would be so dramatic,” said Hopper. “Although the focus of the procedure had always been on her airway, the end result was a great cosmetic difference. This surgery will be a paradigm shift for how we treat children with severely restricted airways.”
A bright future
In total, Hannah’s undergone 12 surgeries and countless hospital stays. Schow said, through it all, Hannah never lost her optimism.
“I feel it’s my mission to tell the world what a wonderful human being she is,” said Schow. “She was born with Treacher Collins syndrome, but that doesn’t define her. I want to teach the world, you shouldn’t judge a book by its cover. People with Treacher Collins syndrome may look different on the outside, but they are smart, loving and talented. I want to share Hannah’s story because she’ll inspire people.”

Today, Hannah may see a slightly different face staring back at her in the mirror, but that face is smiling, new cheekbones and all. For the first time, she’s seeing herself without a tracheostomy.
For Hopper, who is now sharing his new technique with other surgeons across the world, knowing Hannah can simply be a kid, without limitations, is what makes his work so rewarding.
“Hannah is a pioneer,” said Hopper. “She’s paved the road for future patients that will benefit from this procedure. Even though it’s a big thing to go through, the benefits have opened up a new life for her, and I am so pleased she can now do all the things that she loves.”
For more information about Treacher Collins syndrome, or to speak with Seattle Children’s Craniofacial Center about a second opinion or to make an appointment, please call 206-987-2208.
Resources:
- Seattle Children’s Craniofacial Center

