
At 5 months old, Tyler Cassinelli, now 3, was battling both liver cancer and intractable epilepsy. When he was at Seattle Children’s preparing to undergo cancer treatment, Tyler had a seizure that stopped his breathing.
“It was one of the scariest moments of my life,” said Jane Cassinelli, Tyler’s mother. “We could see his stats on the monitor dropping, and doctors came rushing in.”
Doctors quickly intubated and revived Tyler. Five months later, his cancer was in remission. However, he continued to have unpredictable and life-threatening seizures that multiple medications failed to stop.
Genetic testing revealed that Tyler had a mutation of the HCN1 gene. Children with this rare abnormality are at risk for traumatic epilepsies, said Dr. Nino Ramirez, director of the Center for Integrative Brain Research.
“It was difficult to hear that Tyler was expected to have a lifetime of hard-to-control seizures due to a genetic disorder,” said Cassinelli.
In addition to the mutation, Tyler had a brain malformation called focal cortical dysplasia, a common cause of intractable epilepsy. Testing showed Tyler’s seizures were coming from an area on the left side of his brain. Brain surgery to address the problematic lesion could help, and what’s more, his brain could also enable researchers to unlock some of the mysteries of the genetic mutation.
“Tyler’s situation was unique and extremely desperate,” said Ramirez. “There is great clinical interest worldwide in better understanding the HCN1 mutation, and Tyler’s brain could provide a rare window into its role in epilepsy.”
Hard-to-control seizures
After Tyler had his first seizure, they became more frequent and severe over time. The convulsions affected the right side of his body and made him unconscious. To stop his seizures, Tyler needed intubation and continuous IV medication, which he could only receive in Seattle Children’s pediatric intensive care unit. He was flown emergently to Seattle nine times.
“It was hard because we never knew if it would be a 60-second or two-hour seizure that would need medical intervention,” said Cassinelli. “Every seizure felt like a big deal.”
Having two different causes of epilepsy made it challenging to decide whether Tyler should have brain surgery. If Tyler had surgery, he might still have seizures due to the genetic abnormality, said Dr. Stephanie Randle, a neurologist and epileptologist.
“However, Tyler got to a point where his epilepsy was so life-threatening that we needed to try surgery,” said Randle. “The procedure might not cure his epilepsy, but it might prevent the severe, life-threatening seizures he was experiencing.”
The family met with neurosurgeon Dr. Jason Hauptman, who explained the possible benefits of surgery.
“Tyler has intractable epilepsy that we located in a specific area of his brain,” said Hauptman. “We could safely remove it to potentially help his seizures.”
His family ultimately decided surgery was the best option. Hoping to help further researchers’ understanding of Tyler’s disorder, Cassinelli and her husband also decided they would donate part of his brain tissue resected during surgery to Ramirez’s lab at Seattle Children’s Research Institute.
Because Tyler’s liver tumor was treated successfully in part due to research advances, his parents knew firsthand the importance of research in finding cures.
“When researching HCN1, I found that little was known about the abnormality,” said Cassinelli. “If donating Tyler’s brain tissue could accelerate research that could help other kids with HCN1, we definitely wanted to help.”
From the operating room to research lab
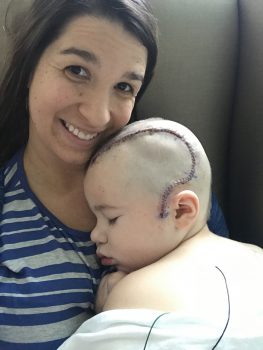
In February, Hauptman performed a temporal lobectomy on Tyler. He surgically removed the part of Tyler’s brain that was one source of his seizures. Hauptman said it was clear that the brain tissue he removed was abnormal. It was firmer with abnormal folds on the surface, indicating the area may have developed differently.
“Tyler did incredibly well,” said Hauptman. “His recovery was uneventful and rapid. In my experience, young children like Tyler recover the fastest after brain surgeries.”
The same day of Tyler’s surgery, philanthropic funding allowed a team of researchers to transport his donated brain tissue to the laboratory for immediate testing. Being able to examine live brain tissue is critical when examining changes in its electrical and chemical activity, which can trigger seizures. Seattle Children’s developed a procedure that preserves the brain tissue for 24 hours using a specific solution, making it available and accessible to the nerve recordings.
Tyler’s live brain tissue provided researchers with the rare opportunity to do physiologic testing that could give clues as to what activity caused by the HCN1 mutation may contribute to seizures. The researchers worked into the night and had their first electrical recording of his brain at 4 a.m.
“We looked at the neurons to see if they were more excitable or not, and how the mutation affected the cell activity,” said Ramirez. “No one has ever been able to do this because very few patients with HCN1 are candidates for surgery. We saw a reduced electrical current, suggesting the mutation may inhibit the activity of the neurons contributing to seizures. This is the first time anyone has been able to see that.”
Accelerating cures

Ramirez said further genetic testing will complement the physiology studies. The researchers will sequence Tyler’s brain tissue to further shed light on how the mutation causes epilepsy and what factors make Tyler’s HCN1 mutation unique.
“In researching Tyler’s case, we are able to ask a unique set of questions, like why Tyler’s epilepsy appeared to only affect the left side of his brain though the mutation is present in cells throughout his brain,” said Ramirez.
In 2016, the human genetics team at Seattle Children’s used patients’ brain tissue to discover a new mutation that can cause intractable epilepsy. The same team in Dr. Ghayda Mirzaa’s lab is now performing genetic testing on Tyler’s brain tissue and will conduct future physiologic studies on the sequenced mutation.
Eventually, once they better understand the mutation, researchers hope to develop a specific, personalized treatment that could stop seizures in children like Tyler.
For Hauptman, Tyler’s case highlights the team-oriented approach providers and scientists take at Seattle Children’s, connecting its research and clinical programs to find cures. Instead of going from the laboratory to the patient, this research went from the patient to the lab.
“We tailored our clinical care and research specifically for Tyler, taking his epilepsy and genetic diagnosis into account,” said Hauptman. “The only way that we’re going to cure children with difficult-to-cure epilepsy is by employing this approach of treating it as not only a clinical question, but a scientific question as well. There’s no other way that we’re going to make the discoveries that may lead to improved therapies.”
And answering the scientific questions behind intractable epilepsy is made possible by philanthropy.
“Without the support of the community, we wouldn’t be able to advance our understanding of these rare, genetic mutations that can have such a devastating impact,” said Ramirez.
The exact same kid

Tyler was back at home only 48 hours after surgery. Today, he is pain-free, feeling better and back in preschool. He enjoys swinging and playing outside.
“Tyler’s recovery from the surgery was incredibly less extreme than his recovery from a prolonged seizure,” said Cassinelli. “He was the exact same kid he was when he went into surgery, and is doing better than we could have ever imagined. He’s a super happy, active kid for all that he’s been through. It’s a complete miracle.”
Since the procedure, Tyler has had some smaller seizures, but has not had any prolonged episodes that require him to be flown to the hospital.
“Tyler is such a sweet kid and is making great developmental gains,” said Randle. “With more time, we’ll have a better understanding of how well the surgery worked for him.”
Randle travels to Richland regularly to see Tyler at Seattle Children’s Tri-Cities Clinic. She is able to see Tyler more frequently instead of managing his care remotely.
“Dr. Randle has been an incredible advocate for Tyler in the past few years, and we are hugely grateful to her,” said Cassinelli. “It’s a huge benefit to have Dr. Randle see us at the Tri-Cities Clinic.”
From brain surgery to follow-up care, Cassinelli said Tyler’s care team has included her in every step of his journey.
“The care at Seattle Children’s is completely unparalleled to any other medical experience we’ve had,” said Cassinelli. “At every appointment, I’m asked for my opinion, since I know my kid best. I think the collaboration between our family and Tyler’s practitioners contributed to us accomplishing so much with Tyler.”
Seattle Children’s researchers are working to better understand the role that genetic mutations may play in conditions like epilepsy to accelerate the discovery of new treatments. Groundbreaking research, like the testing that occurred on Tyler’s brain tissue, would not be possible without philanthropy. This is one of the reasons behind the It Starts With Yes: The Campaign for Seattle Children’s. It Starts With Yes is a $1 billion initiative with a bold vision to transform children’s health. With your help, we will continue to provide financial assistance for families in need; expand necessary healthcare and research facilities; and invest in clinical and research programs to advance pediatric medicine.

