
Children who need a heart transplant face a frightening waiting game before a donor heart becomes available. They must live with a failing heart for months, or even years, as clinicians strive to keep them healthy enough for transplant. Nationally, these patients face the highest waiting list mortality in solid-organ transplantation medicine, with 17% of children dying while waiting for a heart transplant.
Thankfully, Seattle Children’s has one of the best waitlist mortality rates among pediatric heart transplant centers, as reported to the United Network of Organ Sharing. The hospital also treats some of the region’s most complex, advanced heart disease and heart transplant cases and has one of the highest 3-year patient survival rates in the country.
“We are proud to be ranked among the best pediatric heart transplant centers in the country,” said Dr. Yuk Law, medical director of the Cardiac Transplant/Heart Failure Service at Seattle Children’s. “We have created a team of skilled experts who have dedicated their careers to treating heart failure and transplant cases.”
From Hawaii for a heart
Julie was well enough to go to school on Monday, but her symptoms worsened throughout the week.
“I noticed in P.E. that I was getting really out of breath and running really slowly,” said Julie. “I wasn’t my usual self.”
Each day, Julie would feel better in the morning, but progressively got worse throughout the day. Her parents took her to see their pediatrician just before Thanksgiving. In her doctor’s office, Julie fainted and was immediately transported to Kapi’olani Children’s Hospital.
“We still didn’t know what was happening at that point,” said Julie’s mom Lori. We just thought she was dehydrated. We thought everything would be fine.”
Julie was diagnosed with acute cardiomyopathy, severe dysfunction of the heart muscle. The damage hurts the heart’s ability to pump blood and can lead to congestive heart failure. She would need a heart transplant and had three choices for continued care: UCLA, Stanford, or Seattle Children’s.
“Our cardiologist assured us that the collaboration he had with Seattle Children’s and Dr. Law would make the best fit,” Lori said.
The best place to wait
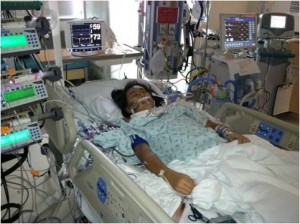
Once Julie arrived in Seattle in late December, she still had to wait for a donor heart to become available. Seattle Children’s was the best place for her to receive care in the meantime.
“We have excellent multidisciplinary care,” Law said. “We have developed a very specialized and well-supported heart failure program that is unique in pediatrics.”
For Julie, the safest way to get her to a heart transplant was with a Thoratec HeartMate II ventricular assist device (VAD). The VAD pumps blood through the body for the heart and allows the heart muscles to rest and recover. Patients with this kind of VAD are able to leave the confines of the hospital while waiting for a transplant.
“Without the VAD, Julie would have been stuck in a hospital bed waiting for a transplant,” said Dr. Michael McMullan, surgical director of Heart Transplantation at Seattle Children’s. “The VAD allowed her to rehabilitate at home. It made her healthier, allowing her lungs and kidneys to work better while she waited for a heart became available.”
Getting her heart

Thankfully, patients at Seattle Children’s often don’t wait long for a heart transplant. The average time a child waits for a heart transplant in the United States is seven months. At Seattle Children’s, the median wait time is just three and a half months. This could be because Seattle Children’s transplant team accepts a wider range of hearts than other centers.
“The longer a child must wait for a heart transplant the greater the chance of complications or death,” Law said. “At Seattle Children’s, our expertise allows us to safely accept larger or smaller hearts, or hearts that are further away. If you have a patient with type O blood, some centers will only transplant a donor heart that’s also type O. We will accept O, AB, A or B for infants, who typically wait the longest for a donor heart. That increases donor availability dramatically.”
Exactly one week after being discharged from Seattle Children’s, Julie’s family got the call – they had an offer for a heart.
“I was in disbelief!” Julie said. “I thought my dad was playing a joke on me. I didn’t think I’d be lucky enough to get a heart so quickly.”
Julie came out of surgery around 3:30 a.m. on Feb. 12, 2014 with a new heart, less than 6 weeks after she’d been added to the transplant list.
Stronger every day
Julie and her family spent a couple months at Seattle Children’s before traveling back to their home to Hawaii. Today, she is healthy and living a normal, active life.
“We’re so thankful our doctor recommended Seattle Children’s,” Lori said. “From the nurses to the doctors, everyone we met has been compassionate and caring. Even though our situation may have been hard at times, Seattle Children’s kept us in the best possible state.”
Watch more of Julie’s story and see how she’s doing today back in Hawaii in the video below:
More than 5,000 children depend on Seattle Children’s Heart Center each year. If you’d like to help support the Heart Center, visit our donation page and specify that you’d like your gift go to the Heart Center Fund.
Resources:
- Heart Transplants at Seattle Children’s
- Seattle Children’s Heart Center

