The following is part 1 of a two-part series on ECPR, a combination of CPR and ECMO offered at Seattle Children’s Hospital to save the most fragile patients’ lives. Here, we tell Hannah Mae Campbell’s story and how ECPR saved her life. In part 2, we’ll discuss how Seattle Children’s has spearheaded a first-of-its-kind ECPR simulation program this year to improve the process that allows the hospital to save patients in a time of crisis.
 Today, Sept. 24, marks a remarkable milestone for the Campbell family – the end of a long, tumultuous journey that began the day their daughter, Hannah Mae Campbell, was born. It’s the anniversary of the day Hannah received a new heart, and a chance at life two years ago.
Today, Sept. 24, marks a remarkable milestone for the Campbell family – the end of a long, tumultuous journey that began the day their daughter, Hannah Mae Campbell, was born. It’s the anniversary of the day Hannah received a new heart, and a chance at life two years ago.
Hannah’s journey begins
When Jennifer Campbell of Everett, Wash., was pregnant with Hannah she prepared as much as she could and followed all the prenatal guidelines to a tee. This was her first baby and she, as all parents do, wanted her little girl to be perfect.
Once Hannah was born on May 18, 2012, Jennifer and her husband Jon remember how the joy of seeing their little girl for the first time quickly turned into terror. Hannah was lethargic, her hands and feet were blue and her heart was rapidly pumping at 253 beats per minute. The room at the local birthing center quickly filled with doctors and then Hannah was taken to the neonatal intensive care unit (NICU). Twelve hours later, Hannah was transferred by ambulance to Seattle Children’s Hospital.
“I was an absolute mess,” said Campbell. “When I saw her in the NICU I thought I was going to be sick. As a first-time mom, I had pictured having this healthy little girl and here my daughter had tubes and wires everywhere.”
At Seattle Children’s, Hannah was first diagnosed with supraventricular tachycardia (SVT), a rapid heartbeat that can be common in newborns, and hypertrophic cardiomyopathy, a thickening of the heart muscle. One week later, with both conditions under control with medication, Hannah was able to go home for the first time.
Two weeks after being home, during a routine check-up, Jennifer was shocked to learn that Hannah’s heart had doubled in size and Hannah was taken back to Seattle Children’s. In an effort to try to control Hannah’s irregular heartbeat, she underwent an ablation surgery and had a pacemaker implanted, but it failed to steady her heartbeat.
Disappointing news, but the worst was yet to come.
“The worst night of my life”
A few days after her surgery, Hannah seemed to be doing better and Jennifer decided to go home for the first time to get some rest and see her two stepsons. Hannah’s medical team gave her a pager just in case of an emergency. At 10 p.m. that night the pager went off.
“I instantly had a pit in my stomach as I knew something was terribly wrong,” she said.
Jennifer listened in shock as she was told that Hannah had gone into cardiac arrest and the team was doing CPR in an attempt to save her life.
“My daughter was dying,” Jennifer recalls. “We immediately jumped in the car and flew down to the hospital as fast as we could. It was the longest car ride of my life.”
Much to their dismay, once they arrived they learned that Hannah was not stabilizing. Her heart was failing. But, there was still hope.
At Seattle Children’s, when a patient doesn’t respond to CPR, parents have the option to put their child on extracorporeal membrane oxygenation (ECMO), a machine that functions for the heart and lungs when the organs fail or need to rest. This combination of ECMO and CPR is known as ECPR and it saves many children each year. Because of Seattle Children’s expertise with ECMO, the hospital has been named a Center of Excellence by the Extracorporeal Life Support Organization (ELSO).
“Not much has changed in how we’re able to treat heart disease, but technology like ECMO and our ability to perform ECPR has vastly improved outcomes for children,” said Dr. Yuk Law, director of Cardiac Transplant and Heart Failure Service at Seattle Children’s, who was also one of Hannah’s cardiologists.
In standard ECPR protocol, Hannah was put on ECMO while CPR was still being performed; a decision Jennifer says is the reason her daughter is still alive today.
Hannah then needed a new heart, but she first had to become strong enough to come off the ECMO machine before she could be listed for transplant.
To everyone’s relief, Hannah’s heart and lungs started to improve after three weeks. She was taken off ECMO and added to the transplant list. The countdown for a new heart began, but again it was unclear if Hannah would make it to transplant. “We just put it in God’s hands,” Jennifer said. “And our wonderful nurses kept our hopes up.”
A new heart arrives

Days turned into weeks and the Campbells tried to keep their family’s spirits up. Their son, Cavan, had a ninth birthday coming up on Sept. 24 and after all they’d been through, they decided to treat him to tickets to a Seahawk’s game. On the evening of Sept. 23, they celebrated his birthday and he blew out his candles over cupcakes.
The next morning, Jennifer got the news she’d been waiting for – Hannah was getting a new heart.
With tears and a trembling voice, Jennifer recalls the emotion of hearing the news, “The hospital called and said, ‘Jennifer you need to come down to the hospital, she’s getting her heart today.’ I just lost it.”
Elated, she first bolted to her sons’ school to tell them the good news. Cavan looked up at her and said, “Mom, that’s what I wished for last night…for Hannah to get her heart.”
At 4 months of age, Hannah got a new heart. By the time of the transplant, her own heart had expanded to the size of an orange, compared to the walnut-sized heart of a typical infant. Hannah was also one of four patients who received a heart transplant within a five-day period in September 2012.
“It was the happiest day of our lives,” Jennifer said. “After so many ups and downs and preparing to say good bye to her so many times, we finally had a chance to get through this. After surgery, we were thrilled to see her pink for the first time because she had normal blood flow and we knew we didn’t have to worry anymore.”
While the Campbells’ were overjoyed for their daughter, they also felt sadness for the family of the heart donor who had lost a child and were grieving.
“To give part of the person they’ve lost to save another child – that’s absolutely amazing to me,” Jennifer said.
An answer is found
Hannah’s remarkable journey alone makes her unique, but it wasn’t until after her transplant that her family learned just how unique she was. After removing Hannah’s heart and further examining it, doctors made an interesting discovery that explained why Hannah’s heart was difficult to control. She had an extremely rare condition called diffuse rhabdomyomatosis where the heart is essentially ingrained with benign tumor cells that continuously grow. The condition is so rare that Hannah is the 4th child in the world to ever be diagnosed, and is the only known survivor.
In order to further educate the medical community about this condition and how it may present in a child, doctors at Seattle Children’s published a case study about Hannah’s experience in The Journal of Heart and Lung Transplantation in April 2014.
Hannah’s road ahead
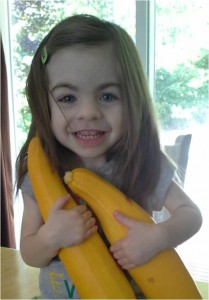 Hannah’s recovery after transplant went well and after 169 days in the hospital, she went home on Nov. 13, 2012, another tremendous milestone for the Campbell family, Jennifer said.
Hannah’s recovery after transplant went well and after 169 days in the hospital, she went home on Nov. 13, 2012, another tremendous milestone for the Campbell family, Jennifer said.
Because of Hannah’s experience, the Campbells are passionate about blood and organ donation and host a blood drive at their church every year on Hannah’s birthday. Hannah had 59 blood transfusions during her time in the hospital.
Now 2 years old, Hannah is an outgoing, happy little girl who is exceeding her developmental milestones and starting to talk.
“She is a beautiful, amazing girl who is a sassy and spunky and who loves everyone, always offering kisses and hugs to those she meets,” Jennifer said. “We wouldn’t have our daughter if it weren’t for ECMO and the heart transplant. We just feel so blessed and grateful to those who saved her life.”
Law was also very pleased with Hannah’s outcome and said it’s very rewarding to be able to save a patient like Hannah who he called a “miracle.”
“We were ecstatic that we were able to pull her through this journey,” said Law. “As doctors we strive to defy nature, and while sometimes we lose, we were able to save her so she could go on to be a happy, healthy little girl.”
Hannah’s heart surgeon who performed her transplant, Dr. Lester Permut, also reflects fondly on where Hannah is today.

“Our goal is to always treat children and their heart problems in a way that results in totally normal functionality and quality of life,” said Permut. “The situations Hannah faced carried many risks and it’s extremely gratifying that she has done so well and has gone on to be a thriving toddler.”
In looking back on this experience, Jennifer also has an important message for other parents who may be faced with a similar situation and must decide whether to put their child on ECMO.
“Putting Hannah on ECMO after CPR was a last-ditch effort, and while it’s a terrifying situation, I want other families to know that there is hope and you can come out on the other side,” she said. “Hannah is doing amazingly well and we’re so happy with where she is today.”
Resources:
- Seattle Children’s Heart Center
- Seattle Children’s Transplant Center
- Seattle Children’s Neonatology program

