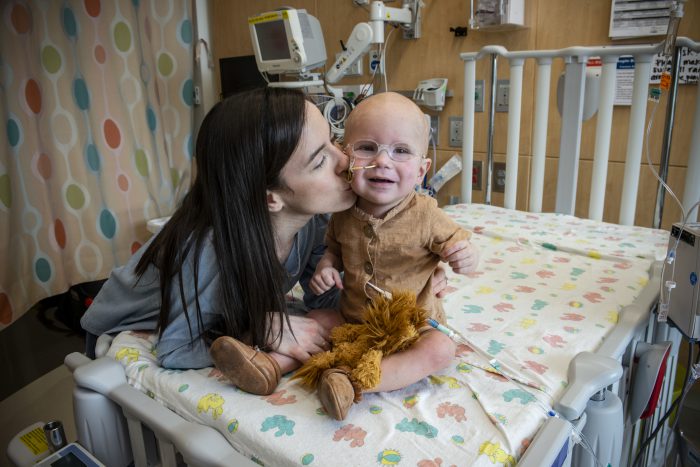
Marilee Killpack describes the birth of her fourth son, Abram, as “magical.”
After a typical, full-term pregnancy, Abram was born in Provo, Utah, weighing 9 pounds. He seemed to be healthy and strong, with one exception: He had petechiae all over his body — red dots that appear on the skin when tiny blood vessels break.
Providers suspected the marks were bruises from his quick birth, but blood tests revealed his platelets were extremely low and his immune system was not making enough antibodies to fight infections.
Abram was taken to the neonatal intensive care unit at his local hospital for platelet and immunoglobulin infusions. Still, his blood counts continued to drop. The family was transferred to a nearby children’s hospital where providers determined he had mononucleosis, which they suspected was causing his immune deficiency.
“They said he would be fine in a few months and sent us home,” Killpack remembers.
But Abram was not fine. He developed severe, uncontrollable eczema when he was 3 weeks old.
“His body was shredded,” Killpack said. “We tried everything — lotions, oils, anything we could think of — but nothing worked. He was screaming; he was in so much pain.”
When providers saw Abram’s skin, they immediately sent a sample of his blood for genetic testing. They suspected he might have a rare, life-threatening disorder called Wiskott-Aldrich syndrome (WAS).
A mysterious diagnosis

WAS is an inherited immune disorder in which a protein deficiency causes low platelets and dysfunctional white blood cells. Patients with WAS have an increased risk of bleeding and infections. They often have eczema and can have an increased risk of developing autoimmune disorders and some types of cancer.
The disease is rare, affecting just one in 250,000 children, and is only symptomatic in boys.
Killpack had never heard of WAS, so she began searching for information online. What she found terrified her: The life expectancy was 3 to 5 years. No treatment was mentioned.
“I remember falling to the floor crying,” she said. “I was devastated.”
For weeks, the family prayed while waiting for the test results. The diagnosis confirmed their fears; Abram had WAS. But there was a treatment — bone marrow transplant.
“Our only option”

The Killpacks were relieved, but soon learned just how complicated and arduous bone marrow transplantation is.
The family first had to find a donor who was a genetic match to Abram, ideally a sibling. Then, Abram would need chemotherapy treatments to destroy his own stem cells and make room for the donor cells. He would likely endure significant side effects.
Dr. Aleksandra Petrovic, a pediatric transplant specialist and researcher at Seattle Children’s Research Institute’s Center for Immunity and Immunotherapies, says bone marrow transplants for primary immune deficiencies, like WAS, are not as common as those performed on cancer patients. Consequently, there are no standard treatment protocols. Patient outcomes depend largely on the treatment center’s depth of experience.
“The key is to give these patients sufficient chemotherapy to allow for successful transplant, while minimizing long-term side effects,” Petrovic said. “This is especially critical because our WAS patients are so young, typically between 1 and 2 years old.”
The Killpacks’ local children’s hospital had only ever performed three transplants on boys with WAS.
“The more we learned about bone marrow transplantation, the more nervous we became,” Killpack said. “But it was our only option. So, we began searching for hospitals that had treated more kids like Abram.”
Who do you trust with your child’s life?

The Killpacks were willing to travel anywhere to give Abram the best chance at a cure. Their search ended after one conversation with Seattle Children’s immunologist Dr. Hans Ochs.
“He spent an hour on the phone with me,” Killpack said. “It was the first time I spoke to someone who had a deep knowledge of my son’s disease. He said there had been about 30 transplants for WAS patients at Seattle Children’s, so we decided to come see the hospital.”
Once the Killpacks saw the hospital and met the transplant team, they were convinced — this was the team that could save their son.
But, getting treatment in Seattle meant Killpack would spend months away from her husband and three other children.
“I knew it would be so hard to be away from them,” Killpack said, “But I also knew this was the right place for us.”
A compassionate guide for a difficult journey 
The family had to wait a year for Abram’s transplant to be sure he was strong enough to survive it. In April 2019 at 15 months, he was finally ready to journey to Seattle.
Seattle Children’s providers thoroughly assessed Abram for two months to make sure he was stable before treating him with chemotherapy.
Four days later, Abram was infused with his 7-year-old brother Copeland’s stem cells.
Abram experienced fevers, breathing and feeding difficulties, high blood pressure, vomiting, fatigue and rashes. But through it all, Seattle Children’s transplant team kept Abram safe.
“I am blown away by the care we received,” Killpack said. “The staff communicated with one another to make sure they were all on the same page, used their available resources to benefit Abram and brought in specialists to address every concern that came up. To be so consistently cohesive is not an accident.”
Abram’s new stem cells engrafted 19 days after transplant. His treatment was successful.
“Seattle Children’s has many years of experience caring for patients with rare immune disorders like WAS,” Petrovic said. “Our multi-disciplinary approach is critical in getting patients, like Abram, through transplant safely.”
Striving for better treatment

While bone marrow transplantation cures approximately 90% of patients with WAS, researchers at Seattle Children’s are studying alternative therapies that would be less harmful.
Dr. David Rawlings, director of the Center for Immunity and Immunotherapies and head of immunology at Seattle Children’s, has spent the last decade working to establish a gene therapy treatment to correct the genetic defect that causes WAS.
Petrovic is working with Rawlings to open a clinical trial that would test the safety and benefit of this new therapy. If it is successful, patients would be treated with an autologous transplant using their own genetically modified stem cells.
This kind of transplant would require less chemotherapy, resulting in fewer long-term effects, including graft-versus-host disease. Additionally, there would be no risk of rejection because patients would be receiving their own cells.
“I hope gene therapy becomes an option for future patients,” Killpack said. “One day, I might have a grandchild with WAS, and I wouldn’t want them to have to go through this.”
The miracle
 Abram was strong enough to leave the hospital 36 days after his transplant.
Abram was strong enough to leave the hospital 36 days after his transplant.
Killpack found herself crying as she said goodbye to their nurses, providers and staff.
“We are so grateful to everyone who rallied together to save Abram,” she said. “He is thriving, and I’m hopeful it will continue. We are not out of the woods yet, but it feels like we’ve experienced a miracle.”

