
Wanting to do something different to address the alarmingly high number of newborn deaths in low income countries, Dr. Rachel Umoren, a neonatologist at Seattle Children’s, turned to virtual reality (VR).
As mobile phone-based VR programs became increasingly accessible, Umoren thought the emerging technology could offer a better way to equip health care providers with the skills necessary to save babies’ lives in low- and middle-income countries with high neonatal mortality rates.
Her case was compelling: with mobile VR training, providers could learn and easily maintain new skills at their own convenience, on their own smartphone, and with game-based automated feedback that is ideal for learning. With its on-demand availability, she believed mobile phone-based VR training could effectively translate into clinical practice better than current training methods.
“Mobile technologies are ubiquitous in low and middle income countries, yet they are relatively untested at disseminating health care information or training in these settings,” Umoren said. “I wanted to see how we could apply innovations in virtual reality to address the pressing issue of neonatal mortality.”
Virtual reality offers new way to train providers

The Electronic Helping Babies Breathe (eHBB) VR application Umoren developed, with support from the Bill and Melinda Gates Foundation and several national and international partners, is simple. By attaching a small pair of VR glasses to a smartphone or using a low-cost VR viewer like Google Cardboard™, the provider is led through the skills necessary to resuscitate a newborn when the baby is unable to breathe on their own. According to Umoren, birth asphyxia, a condition that results when the baby’s brain and other organs are deprived of oxygen and nutrients before, during or after birth is a leading cause of death and disease in newborns.
“Neonatal resuscitation training reduces newborn mortality, but programs that rely on in-person classes and knowledge transfer through others are often inconsistent and ineffective in low-resource settings,” Umoren said. “The initial gains made through training rapidly decay because providers lack continued opportunities to hone their skills.”
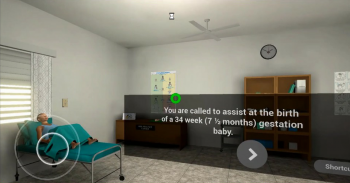
In the VR simulation, which Umoren created in collaboration with the LIFE Project at Oxford University, requires the user to provide neonatal care in one of three scenarios upon entering the delivery room. There is one scenario where the baby needs resuscitation, another where the baby only requires some resuscitation and a final scenario where the baby is born healthy and crying, just needing routine care.
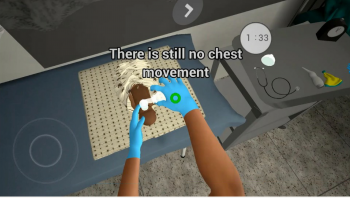
The eHBB VR simulation follows a widely-disseminated, evidence-based neonatal resuscitation curriculum developed by the American Academy for Pediatrics called Helping Babies Breathe. Animated simulations coach the provider through each scenario, prompting them to make choices to get to the next step. The virtual environment responds by changing to show the result of the choice selected. Since emergency resuscitation procedures like using a bag and mask to help the baby breathe need to be started within the first minute after birth, often called “The Golden Minute”, the goal is to get through all of the steps as quickly as possible.
Features, such as the color of the room, the baby’s blanket or whether there is a sink or a bucket of water for washing hands, are randomized for variety. A personalized debrief at the conclusion of each scenario gives feedback on what the provider did well and where there is room for improvement. The training program can be downloaded, so a reliable Internet connection is not needed for repeat uses.
“Beyond training future health care providers, the hope is that it will save lives,” Umoren said. “That babies in distress who need to be resuscitated by providers who have had this training will survive.”
Nigeria and Kenya first to test virtual training
Umoren, a member of the Center for Child Health, Behavior and Development and director of Neonatal Education & Simulation-Based Training (NEST) at Seattle Children’s and the University of Washington School of Medicine, presented data from a national survey of Nigerian pediatric providers and usability studies with the VR simulation conducted in partnership with the University of Lagos and National Hospital Abuja in Nigeria at the 2019 Paediatric Association of Nigeria Conference and the 2019 International Meeting for Simulation in Healthcare.
The results showed that while the current use of simulation-based training in Nigeria is low, there is uniform acceptance of VR simulation as a training modality, resulting in a statement being issued by the Paediatric Association of Nigeria that called for Nigerian pediatricians to integrate and promote simulation based education in pediatric treatments and management.
She is now working with partners at the University of Lagos, Nigeria and Alupe University, Kenya to enroll about 300 health care providers from 20 facilities on a trial testing the simulation’s impact on neonatal resuscitation performance. The randomized trial will compare provider groups receiving the VR simulation with groups receiving a video training or standard in-person training. A mobile platform from Indiana University, called mobile Helping Babies Survive (mHBS), will capture data from each game session, in-person simulation, and observed newborn resuscitation, storing it for later analysis in a health information database so that researchers can identify which areas of the curriculum were better reinforced by the VR simulation.
One particular area that interests Umoren and others involved in health care simulation training is determining if VR can aid the provider in activation – that is getting a trainee to move forward quickly in the simulation. She explains how the VR simulation may help overcome challenges with activation by offering visual prompts that a new action is needed and encourage the user to move forward when they get stuck on a step.
“We want to reinforce the correct approach, so that means not allowing the user to make so many wrong choices that the baby dies during the simulation,” she said. “Rather, we want to keep providers on the right track, hard-wiring their knowledge of the correct steps to successfully resuscitate the baby.”
Early evidence encourages researchers
While the researchers eagerly await the data from the trial to determine if the tool is effective in facilitating resuscitation training at the sites in Nigeria and Kenya, both the data from the usability studies and healthcare worker receptiveness to the new training modality are encouraging.
Umoren tells the story of a UW biomedical engineering student with no neonatal resuscitation experience who first demoed the virtual training and then went down to a standard simulation lab. While exploring the features of the manikin which included the ability to cry, she noticed that the student placed the hat on the manikin as soon as it started crying, mimicking the next step in the virtual simulation.
When Umoren asked the student why she did that, she responded, “Just like in the training, so that the baby doesn’t get cold.”
“I was amazed to see how the skills introduced in the virtual training immediately translated to real-world practice,” Umoren said. “It’s just one example, but it displays why I think all of our partners have been so receptive and excited to have the opportunity to help develop and test this training.”
Resources
- WATCH: Video demo of the eHBB virtual simulation
- NEST Program Helps Pediatric Providers in the Region Breathe Easy
- Seattle Children’s Neonatology Program
- Seattle Children’s Level IV NICU

