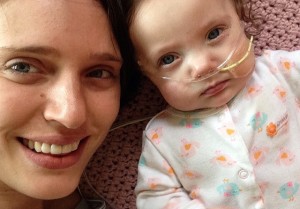
Everything went perfectly when Amanda Erickson’s first baby was born. Bennet arrived right on time on March 11, 2012, healthy and eager to nurse.
Exactly two years later – on March 11, 2014 – Bennet’s sister, Juliette, came into the world. This time, says Erickson, “it was an adventure birth.”
In other words, nothing went as planned.
Juliette had been diagnosed before birth with a serious heart problem, and Erickson planned to deliver at the University of Washington Medical Center so her baby could get to Seattle Children’s right away.
“We knew she wouldn’t be able to breathe on her own,” says Amanda.
But nobody expected Amanda to go into labor two and a half months early. As an ambulance rushed her from Silverdale, Wash., to Seattle, Seattle Children’s sent a second ambulance – with neonatal experts and life-saving equipment – to accompany it in case the baby came before she reached the hospital.
Erickson got to the hospital in time. But when Juliette was born, the delivery team found a surprise: in addition to her heart issue, she had a tumor, called a teratoma, in her mouth.
Before Erickson even had a chance to meet her infant daughter, Juliette was rushed to the Neonatal Intensive Care Unit (NICU) at Seattle Children’s. Amanda didn’t expect her own needs to be the focus of anyone’s attention. But she was still a new mom dealing with new-mom issues, so she was surprised – and relieved – to get a visit from a lactation consultant soon after she arrived.
“I was craving for Juliette to nurse,” says Erickson. “But she was a tiny baby with a big tumor in her mouth.”
Juliette was so fragile that Erickson couldn’t even pick her up until she was 20 days old. Even then, the tumor prevented her from latching on and nursing. But with support from the lactation team, Erickson was able to get breast milk to Juliette just as soon as her daughter could tolerate it, and to keep her milk supply strong and steady to sustain Juliette as she gained strength and grew.
Natural experience, unnatural surroundings
“Breastfeeding can be stressful in the best of circumstances – you add another whole layer of stress on top of it when the baby is sick,” says Jennifer Enich, a dietitian and lead lactation consultant at Seattle Children’s.
Enich’s five-person team visits with every nursing mother in the hospital as often as the mom needs them. They work with up to 18 nursing moms each day, some for quick check-ins and some for intensive, two-hour assessments.

The consultants help demystify breast pumps and troubleshoot supply problems. They answer questions and serve as resources as these new moms have one of the most natural of human experiences in the most unnatural of surroundings.
Some moms, like Erickson, need help establishing and maintaining a milk supply for a baby who is unable to nurse. Others can’t produce milk quickly enough for their new babies, and others struggle with infections and other complications of breastfeeding.
Many babies who are too sick to nurse at the beginning of life lose their instinct to latch on and suck by the time they are physically capable of doing so. Lactation consultants help the moms of these babies keep their milk supplies healthy while physical and occupational therapists work with the babies to help them coordinate the complex tasks of sucking and swallowing.
Enich says that the moms she meets are surprised to learn that Seattle Children’s has lactation experts on staff.
“They expect Seattle Children’s to meet the needs of their baby, but they have no idea that we have services to meet their needs, too,” she says.
“I had so many questions, and I would have been lost without help from these experts,” says Erickson.
Big changes coming with the new kitchen
In addition to supporting new moms, the lactation team – which is part of the Nutrition Department – helps ensure the safety of stored breast milk. The group is deeply involved in developing a formula/milk room in the new kitchen, which is under construction in the basement of the Forest zone of the hospital.
Currently, any breast milk that is not immediately consumed is marked with the baby’s name and medical record number and stored in freezers on units where the baby is staying. But there’s just not enough space, says Jennifer.
The new formula/milk room will change that; all breast milk not consumed immediately will be barcoded; fortified or pasteurized, if necessary; stored; and sent out from this central location. Not only will there be ample storage space, but barcoding the breast milk will allow it to be closely tracked.
“It will help ensure that the milk always gets to the right baby, the mom’s supply is always known, less milk is wasted and milk always goes home – or is donated – when a baby is discharged,” says Enich.
Seattle Children’s is also exploring a relationship with the Northwest Mother’s Milk Bank in Portland, Ore. – the closest milk bank to Seattle – to help make sure excess milk doesn’t go to waste and gets to babies who need it.

“We would love to be a milk depot or local distribution center for the Portland bank,” says Enich. “In the long run, we would like to establish a milk bank in Seattle to serve not just babies hospitalized here, but all babies in the community.”
A good eater goes home
Juliette was never able to nurse. But thanks to her mom’s steady milk supply, she was able to get nutrition custom-made for her through a nasogastric tube until she was old enough and well enough to start eating other foods.
“She still loves her milk, but she also eats anything and everything she can,” says Erickson. “That makes her mom’s heart happy.”
Resources:
- Seattle Children’s Neonatology Program

