
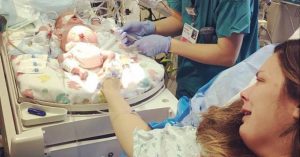
Brandi Harrington seized the first opportunity she had to touch her newborn son minutes before he was taken by ambulance to Seattle Children’s Neonatal Intensive Care Unit (NICU). She and her husband, Tyler Harrington, were told Oliver had a 1% chance of surviving.
Propped up in a hospital bed following an emergency cesarean delivery seven weeks before her due date, Brandi saw Oliver for the first time. Tubes and wires connected all but one part of Oliver’s little, swollen body to machines that supported and monitored his breathing, heart rate and oxygen levels.
Brandi reached for Oliver’s left foot, his only limb barren of medical equipment.
“When I touched his foot and said his name, he started moving his mouth,” Brandi said. “He would only do that to the sound of my voice.”
This moment of bonding only briefly interrupted an agonizing time of unknowns for the Harringtons. The Harringtons didn’t know if Oliver would live long enough for them to hold him for the first time.
They had no idea a mysterious mass the size of an adult’s fist was in their son’s tiny right lung, suffocating him and reducing his chances of survival by the minute.
Nor did they envision Oliver home with his two siblings less than a month later. Or that almost nine months later, he would be home to experience the Harringtons’ first Christmas as a family of five.
Complications lead to Oliver’s early arrival
Brandi was admitted to Tacoma General Hospital in her 32nd week of pregnancy with pre-term contractions and excess amniotic fluid, a condition called polyhydraminos. An ultrasound revealed fluid in Oliver’s lungs and the possibility he had hydrops fetalis, an abnormal accumulation of fluid in the fetus that can be life-threatening.
“We were told that he had a 50% chance of survival and that our son would be in the NICU for months if he survived birth,” Brandi said.
Oliver’s decreased respiratory function and heart rate prompted an emergency C-section two days later.
“As soon as they cut the umbilical cord, Oliver turned purple,” Tyler said.
Decisive action is taken to save Oliver’s life
Oliver struggled to breathe and the swelling in his body restricted his blood flow. Doctors thought the mass in Oliver’s right chest detected on an X-ray could be related to a diaphragmatic hernia, a hole in the thin muscle between the chest and abdomen that can lead to severe complications for the lungs and heart.
In an effort to save Oliver’s life, Tacoma General contacted Seattle Children’s NICU to consider him for a specialized artificial heart and lung bypass therapy called extracorporeal membrane oxygenation (ECMO).
As a physician’s assistant in the emergency department at Tacoma General with military medical experience, Tyler had a high-level understanding of the danger his son was in. But he maintained his composure as he shuttled between hospital rooms to show Brandi pictures of Oliver and update her on the fast-moving developments.
At less than 2 hours old, Oliver was transported with Tyler by his side in an ambulance 40 miles north to Seattle Children’s.
A hectic four days of discovery
Soon after arriving at Seattle Children’s, it was discovered that while Oliver did need surgery to remove the mass in his lungs, he did not have a diaphragmatic hernia and there was not an immediate need for ECMO. Doctors wanted to stabilize Oliver and allow him to overcome the stress of birth before reevaluating him for the chest surgery he needed.
“Oliver continued to struggle, but gradually got better his first night at Seattle Children’s with specialized treatment on a high frequency ventilator,” said Dr. Robert DiGeronimo, medical director of the Seattle Children’s NICU. “There was still a concern that he would need ECMO, but he was stabilized and slightly improved with additional medications.”
Over the next three days, Oliver’s progress continued. Brandi joined Tyler at Seattle Children’s following two days of recovery from her C-section. The couple returned home after Oliver’s fourth day at Seattle Children’s to spend the night with their 2-year-old daughter Annabelle, and 1-year-old son, Samuel, who were being watched by Brandi’s parents.
“It’s heartbreaking to leave your child,” Brandi said. “But there was always someone in our room. We knew that people were talking to Oliver and loving him when we couldn’t be there at that moment.”
Day 5: Bringing the operation to Oliver
As Brandi and Tyler were preparing to return to Oliver’s side early the next morning, they were told Oliver’s progress had stalled and he needed immediate surgical intervention to remove the mass from his lung.
The margin for a decline in Oliver’s condition was miniscule. Anything but progress put his life at risk.
The high frequency ventilator keeping Oliver alive was difficult to move and Oliver was not stable enough to be safely moved to an operating room without it. So the operating room was brought to Oliver.
“The need for surgery became quite urgent,” said pediatric surgeon Dr. Daniel Ledbetter. “Oliver also needed the high frequency ventilator to stabilize his breathing and it was a risk to have him off that for hours during a major surgery.”
In a matter of hours, the surgical and NICU staffs embarked on a highly coordinated effort to ensure all equipment and personnel needed for Oliver’s surgery was brought to his bedside in the NICU.
”We took as much as we could to best replicate the operating room, including preparing for urgent scenarios like a blood transfusion, if needed,” Ledbetter said.
Ledbetter provided comfort and assurance for parents once again faced with the possibility of their son’s death.
“Dr. Ledbetter told me he was confident he could help my son,” Tyler said. “It really meant a lot to me.”
During the chest surgery, Ledbetter removed an abnormal piece of Oliver’s lung. A 4-by-3-inch rare tumor had overtaken the lower lobe of his right right lung, inhibiting the function of both lungs and putting pressure on his heart.
“Oliver did amazingly well during the surgery and once the mass was removed, he immediately started breathing easier, allowing him to start weaning off his medical support,” DiGeronimo said.
The road to a miraculous recovery quickly leads Oliver home
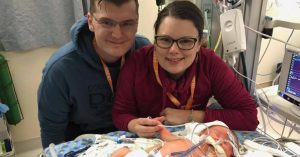
Two days after surgery, when Oliver was 9 days old, Brandi held him for the first time.
“All a mother wants to do is snuggle her baby and it’s really hard when you can’t,” Brandi said. “I still remember the first time I heard his voice. It was the most incredible thing.”
Oliver was rapidly recovering, and only six days after surgery, he was breathing on his own without a ventilator.
“It was pretty remarkable that Oliver was off the ventilator,” DiGeronimo said. “His body swelling also went away and you never would have guessed he was so sick.”
When Oliver was 17 days old, less than two weeks after the surgery that saved his life, he was transported back to Tacoma General so the Harringtons could be closer to home for the remainder of his hospital stay.
Oliver was discharged from Tacoma General when he was 4 weeks old, nearly three weeks before his expected due date.
A family whole for the holidays

As the Harringtons adjusted to their new normal at home as a family of five, Oliver had a few obstacles at first. He experienced some apneic spells and had severe reflux, but then he grew. A lot.
By the time Oliver was 6 months old, he weighed 23 pounds, was laughing hysterically at peek-a-boo, and could roll over.
In addition to being thankful to the care teams at Tacoma General and Seattle Children’s for saving their son’s life, the Harringtons credit their faith, church, family and friends for helping them navigate such a stressful period.
Now nearly 9 months old, Oliver has his first few teeth, babbles frequently and is fascinated by Christmas tree lights and decorations.
“We are more than thrilled to celebrate our first Christmas as a family of five,” Brandi said. “It is a milestone that we didn’t know we would experience, and we are so thankful to have Oliver as a part of our lives.”
Resources:
Reflections of my LIFE with Jesus – Brandi Harrington blog

