Laura Licea joined Seattle Children’s in July 2023 as vice president (VP) of Perioperative and Procedural Services and associate chief nursing officer. She brings a fresh perspective and an extensive background in the operating room (OR) from her previous roles at organizations such as UCSF Benioff Children’s Hospitals. Licea’s goals include Seattle Children’s becoming a center […]
In August 2020, just after her third birthday, Aisley began to experience concerning symptoms: headaches in the back of her head, a lack of appetite and vomiting. After a visit to her pediatrician, Aisley was sent to Seattle Children’s for an urgent neurology visit, where she passed the exam with “flying colors,” showing no signs of trouble. Still, Dr. […]
Rachael and her husband had saved for years to buy their first home, where they hoped to settle and raise their family. With a two-year-old boy and a baby on the way, they excitedly made an offer on a house in Bellingham and scheduled an appointment to sign the last of the papers. While they […]
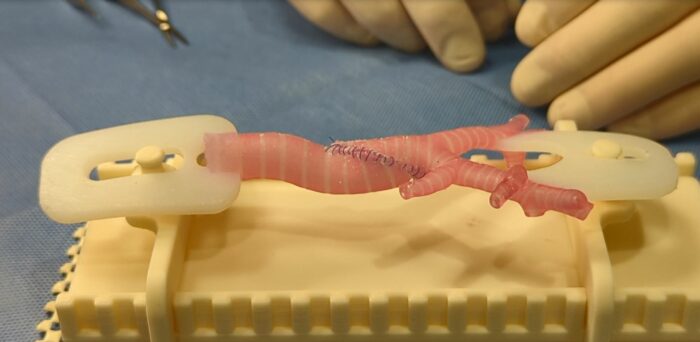
Seattle Children’s Doctors Use 3D Printing to Help Train International Care Teams on Complex Surgery
Healthcare organizations are increasingly looking to incorporate the use of 3D-printed models to help improve outcomes for pediatric patients in need of very complex surgeries. Doctors at Seattle Children’s are now utilizing 3-D printed models created in the hospital’s Innovation Lab to train international care teams in a highly specialized procedure, known as a slide […]
In 2019, Samantha and Kyle Hatch received wonderful news: Samantha was pregnant with identical twins. The couple already had two kids, Ben and Penny, and envisioned all of the roughhousing, road trips and happy mayhem that comes with four children. But everything changed when a routine ultrasound showed that one of the twins, William, had […]
Each year, Seattle Children’s Craniofacial Center treats hundreds of children with craniosynostosis, a condition most families have never heard of, yet can affect approximately 1 in every 2,500 babies in the United States. That was the case for Kali Dempsey’s family, of Camano Island, WA, in early 2017. “We were sent to Seattle Children’s when […]
After a family trip to Finland last summer, Jasmine’s family became increasingly concerned about some unusual symptoms she was experiencing. What started as occasional numbness in her lip or left side of her face last spring had progressed to twitching, which the family later learned were increasingly strong seizures. Her family had been proactive in […]
9-year-old DeAngelo “DJ” has his dreams for the future all planned out. “DJ tells everyone that he wants to become a pediatric surgeon or a pediatric gastroenterologist one day,” explained Angela McCulloch. “He says that he plans to go to school at the University of Washington and work at Seattle Children’s to help kids like […]
It’s been 12 years, but Brandy Epling still chokes up at the traumatic memory of her firstborn’s birth. It was a difficult pregnancy, with preterm labor forcing a 33-day stay at a southwest Washington hospital for the mom-to-be, followed by months of bedrest. Ultrasounds revealed the baby’s brain was a bit bigger on the left […]
When Jiana was born in August 2021, she appeared to be a typical, healthy newborn baby. “I still remember her pediatrician called her a textbook baby,” recalled Latika, Jiana’s mom. Unfortunately, that normalcy was short lived. On her first day home from the hospital, Jiana’s parents noticed their daughter was twitching. “We were first-time parents […]