
A single blow to 18-year-old Miguel Navarro’s shoulder turned his world upside down. He was boxing with his friends one afternoon when he felt a snap. He took a hit to his shoulder and immediately knew something was wrong.
“That punch altered my world,” said Miguel.
Miguel went to the emergency room where he found out he fractured his humerus, the long bone in the upper arm. Unfortunately, that wasn’t where his medical journey ended. While undergoing imaging, doctors noticed something amiss, and so Miguel underwent a myriad of tests. At the time, doctors thought what they saw in his imaging results could be a benign tumor.
On Dec. 12, 2017, Miguel was told the tumor wasn’t benign. He had osteosarcoma, an aggressive type of bone cancer.
Miguel’s world stopped. He was in the middle of his senior year of high school and thought he had his life figured out. He dreamed of joining the Air Force Academy. Unfortunately, his diagnosis derailed his plans.
A new path
In January, instead of heading back to school, Miguel was checking in to Seattle Children’s Cancer Care Unit. He had a grueling journey ahead of him, one that started with 10 weeks of chemotherapy.
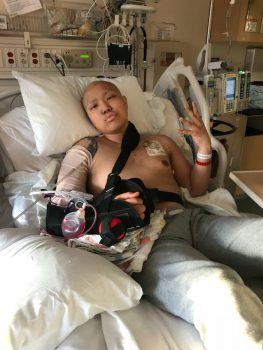
“Cancer guided me on a new path,” said Miguel. “I kept reminding myself that there’s always someone going through worse. I’ve been very blessed. I held on to that notion.”
Seattle Children’s Bone Tumor and Sarcoma Clinic provides care for children, adolescents and young adults with bone tumors and soft tissue tumors. Treatment for bone and soft tissue tumors can be complex, and so it’s important to be cared for by a team of experts who individualize care and treatment options to meet the unique needs of every patient. The team consists of oncologists, orthopedic surgeons, nurse practitioners, pathologists, musculoskeletal radiologists, radiation oncologists, pediatric anesthesiologists, social workers, registered dietitians, child life specialists, physical therapists and specialists in orthotics and prosthetics.
“Our program is designed for patients like Miguel,” said Dr. Katie Albert, a pediatric oncologist at Seattle Children’s. “We’re an experienced and comprehensive sarcoma center with an incredible level of expertise to coordinate complex care. Our goal in the beginning, middle and at the end of treatment is always to cure the disease and get these kids back to their lives.”
Miguel spent nearly a month inpatient on the Cancer Care Unit. Seattle Children’s became a familiar place. Every round of chemotherapy brought him back to hospital.
“I felt like I was in the hospital more than I was out of the hospital,” said Miguel.
Building Miguel a new shoulder
In April, after undergoing 10 weeks of chemotherapy, Miguel was scheduled for surgery to remove the tumor in his shoulder. Dr. Matthew Thompson, an orthopedic surgeon in the Bone Tumor and Sarcoma Clinic, performed the operation.
“Since the tumor was located in his shoulder joint, he needed an extensive surgery,” said Thompson. “We needed to remove the entire tumor and reconstruct his shoulder using a custom shoulder implant designed specifically for Miguel.”
Essentially, Thompson was tasked with building a new shoulder for Miguel. Using 3-D models, the implant was designed to fit his bone and help preserve as much normal function in his arm as possible.
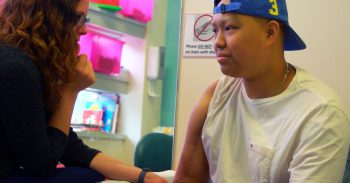
Before the operation, Miguel told Thompson about a goal he had for after the surgery. He said one day he wanted to be able to drive a stick shift car again.
“When you’re driving, you feel like you’re in control,” said Miguel. “It’s an escape.”
Since being diagnosed with cancer, Miguel’s life had seemed anything but in control, and the goal resonated with his care team. They were determined to make his goal a reality.
“I think it is always easy to get caught up in hopeless optimism in wanting what is best for our patients. Wanting to match Miguel’s persistent positivity and joviality. But, we were realistic in planning Miguel’s difficult surgery,” said Thompson. “First and foremost, we needed to remove the tumor and prevent it from coming back. This would be difficult because of its proximity to many critical structures and its extent, but my hope was that we’d be able to preserve the limb with enough function that it would contribute to a long and fulfilling life for Miguel. Since one of the things that makes life fulfilling for Miguel is being able to drive a stick shift, we wanted to make that possibility our goal.”
On the road to taking back the wheel

Through everything, Miguel has held onto the hope that things would be okay and that one day he’d be able to get behind the wheel again.
“You have to have a bright outcome in your mind, or it consumes you,” said Miguel.
The surgery in April was a success. Doctors were able to spare his arm while also removing the entire tumor in his shoulder. After surgery, he needed another 20 weeks of chemotherapy.
On Aug. 14, Miguel completed his last round of chemotherapy. Now, he’s solely focused on the road ahead, which includes intense rehabilitation to regain movement in his arm. After the surgery, Miguel was only able to move three fingers. Today, he’s relearning to tie his shoes and can bear the weight of a cup of coffee in his right arm.
Miguel’s care team remains optimistic about his ability to reach his goal. Every week, he continues to push himself. He hopes his story will be inspirational to other people.
“I’ve never doubted I’d get better,” said Miguel. “I want to set a good example for the next generation. I want them to know if they set their minds to something, then they can accomplish it.”
He recently graduated high school and plans to pursue a career in social work so he can help children at Seattle Children’s on the Cancer Care Unit.
“I’m blessed to be alive,” said Miguel. “Now, I want to be hope for someone else.”
Doctors and researchers at Seattle Children’s are working to improve treatments and outcomes for children with bone and soft tissue tumors, giving patients access to the latest options under investigation for their diagnosis.
A phase 1 clinical trial at Seattle Children’s is testing CAR T-cell immunotherapy in children and young adults with relapsed or refractory solid tumors. The trial is called STRIvE-01. In this trial, a patient’s own T cells are reprogrammed to recognize and target the protein EGFR, which is expressed by many childhood solid tumors, including sarcomas.
For more information visit T-Cell Immunotherapy for Solid Tumors (STRIvE).

