
At 19, Faye was not planning for parenthood. She was a freshman at Northeastern University in Boston, Massachusetts. She spent her days thinking about majoring in French and dreaming of working with the United Nations Refugee Agency, not about whether she wanted to be a mother one day.
But an unexpected diagnosis changed all that.
Six weeks into her second semester, Faye began having high fevers and visited the university’s health clinic. Providers suggested she had the flu and would feel better in about a week, but her symptoms quickly grew worse. A few days later, she woke up with a fever of 104 degrees.
Faye thought to herself, “I need to see a doctor now.” She took an Uber to Boston Medical Center’s Emergency Department and tested positive for mononucleosis. They kept her overnight because her white blood cell count was abnormally low.
“Luckily, the woman looking at my slides noticed what she thought were blast cells (primitive, undifferentiated blood cells, often found in the blood of people with acute leukemia) and sent them to the pathologist, who confirmed they were,” Faye said.
She was transferred to Boston Children’s Hospital, where she was diagnosed with high-risk B-cell acute lymphoblastic leukemia.
“I believe everything happens for a reason,” Faye said. “I feel like, this happened to me and my family because we are strong enough to get through it.”
The cost of treatment

Faye began chemotherapy at Boston Children’s and was transferred a month later to Seattle Children’s, where she would be closer to family.
She handled the treatment better than she’d anticipated, but after the second round she still wasn’t in remission like her doctors hoped she would be. They recommended she have a bone marrow transplant.
Seattle Children’s Cancer and Blood Disorders Center team hoped a transplant would put Faye in remission, but they expected it would also make her infertile.
The situation was difficult for Faye to reconcile at her age. Then, one day, her mom showed her a video of a cute kid playing the drums on Ellen.
“I thought to myself, ‘I can’t wait to have a kid.’ Then it occurred to me that I might not be able to have one, and I broke down,” she said.
The only option

Faye asked her care team if she could freeze her eggs, but her cancer was too aggressive; she couldn’t pause chemotherapy long enough to undergo the necessary ovarian stimulation and retrieval of her eggs.
“She was quite sick when she presented and needed to start chemo right away,” said Dr. Tyler Ketterl, medical director of Seattle Children’s Adolescent and Young Adult (AYA) Cancer Program. “Her chemo regimen was unlikely to affect her fertility, but the bone marrow transplant, with total body irradiation, would likely make her sterile.”
There was one option to preserve Faye’s fertility: She could freeze tissue from her ovary before her transplant.
Ovarian tissue cryopreservation is a method of fertility preservation in which a patient’s ovary — or portions of it — is surgically removed before cancer treatment and frozen until the patient is ready to use the tissue for family building.
Unlike egg freezing, ovarian tissue can be removed and frozen at any time, without interrupting chemotherapy or other cancer treatments. Surgeons will often couple it with another procedure, like a central line placement or tumor removal.
Freezing ovarian tissue is also currently the best choice for prepubertal girls who have no other fertility preservation options. Because women are born with all their eggs, the procedure can be performed on very young girls — even toddlers.
“There are no real age limits, other than the fact that it can be harder to get enough tissue from really young patients who have smaller ovaries,” Ketterl said.
Ovarian tissue cryopreservation may also benefit patients outside the cancer population, such as nephrology patients who receive high-dose medications that impact fertility; transgender patients; patients with Turner syndrome and patients who have non-malignant diseases that require a bone marrow transplant (such as sickle cell anemia).
For cancer patients, there is a risk that the preserved tissue could harbor cancer cells when it’s implanted back into the patient.
“For patients with leukemia, where we know there are circulating tumor cells, we will only perform ovarian tissue cryopreservation if the patient is in a deep remission,” Ketterl said. “There’s also an experimental method in which you can mature eggs outside the body. In that case, the ovarian tissue wouldn’t necessarily need to re-implanted. That science is moving along quickly.”
Ovarian tissue cryopreservation was considered experimental until December 2019, when the American Society of Reproductive Medicine (ASRM) declared there had been enough live births as a result of this method to remove the experimental designation.
“We’d been considering this method for our patients for years, but ASRM’s decision was a game changer,” Ketterl said. “We were ready, we just needed the right patient.”
The perfect first patient
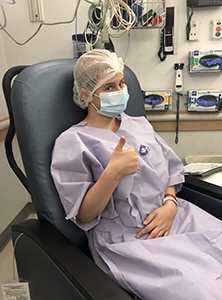
Ketterl presented the option of freezing ovarian tissue to Faye. She was initially overwhelmed with the decision that could affect the rest of her life. But in the end, she decided to go for it.
“I couldn’t imagine looking back in 10 years and regretting my choice,” she said. “I thought I would be devastated if I didn’t have the option to have my own genetic child one day. Having cancer, everything is out of my control. So, to have some semblance of ownership over myself and my future felt empowering and beneficial to my mental state.”
Being the first patient at Seattle Children’s to undergo ovarian tissue cryopreservation didn’t bother Faye.
“I felt like I would be selfish if I didn’t do it and possibly took the opportunity from other people who wouldn’t be comfortable being the first,” she said.
“The best place for cancer treatment”
Faye’s ovary was successfully removed without complications by Seattle Children’s surgeons Dr. Katherine Debiec and Dr. Kimberly Riehle. It was flown to Pittsburgh and arrived at the University of Pittsburgh Medical Center within 19 hours, where it was processed and frozen for long-term storage.
Ketterl hopes to offer ovarian tissue cryopreservation to more and more patients in the future. Since Faye, Seattle Children’s has performed the procedure for seven other patients.
“Patients report that the possibility of preserving their fertility is instrumental to coping before and after cancer treatment,” Ketterl said. “We have to keep striving to increase the options we have for our patients so we can address gender inequities and offer the fullest breadth of services.”
Research has also shown that for certain kinds of cancer, teens and young adults like Faye have better results when they are treated at a pediatric hospital like Seattle Children’s. In addition to fertility preservation options, the AYA program supports patients and their families with expertise in adolescent medicine and other supportive care like nutrition, pain management and physical therapy, emotional health support and school services.
Today with care from Ketterl and the whole AYA team, Faye, who celebrated her 20th birthday in November, is recovering from her bone marrow transplant.
“I feel confident that I’m in the best place to receive cancer treatment,” Faye said. “Forty years ago, my cancer probably would have killed me; I certainly wouldn’t have had the opportunity to freeze tissue from my ovary. So, while I still have a long road ahead, I feel really grateful.”

