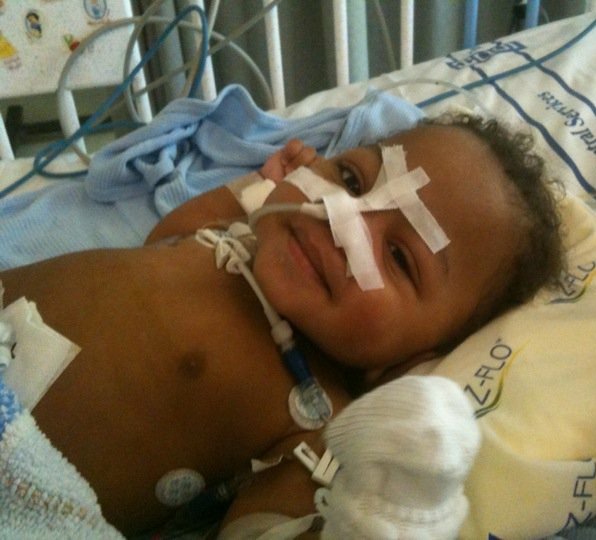
It’s common for parents of young children to worry about the unexpected accident that may occur while they’re out in public. But for the Henderson family, being prepared for the unexpected was something that lasted well beyond the early years of childhood.
Whether it was attending a family gathering or simply dropping by the grocery store, there was always a looming concern around when their youngest son, Brennan, may have his next vomiting or bowel incontinence episode.
“There were times when we would go to a restaurant and have to cover him with a blanket,” said Brennan’s mother, Gloria Henderson. “We did it to muffle the sound of him vomiting into a bag. It felt awful having to do it, but it was the only option we had.”
Brennan was born 3 months premature with a host of debilitating health conditions, including necrotizing enterocolitis (NEC).
“Necrotizing enterocolitis is a condition more commonly seen in premature babies that affects the intestines,” said Dr. Simon Horslen, medical director of solid organ transplantation and head of the Intestinal Rehabilitation Program at Seattle Children’s. “‘Enterocolitis’ means inflamed small intestine and colon, and ‘necrotizing’ means it causes tissue death. With NEC, the intestines become inflamed and may become infected by bacteria. The inflammation can cause part of the intestine to die.”
A small baby faces a giant load of health issues
Weighing a little over the size of a pineapple at just 2 pounds, 4 ounces, 3-week-old Brennan was transferred to Seattle Children’s Neonatal Intensive Care Unit (NICU) to undergo multiple tests and evaluations.
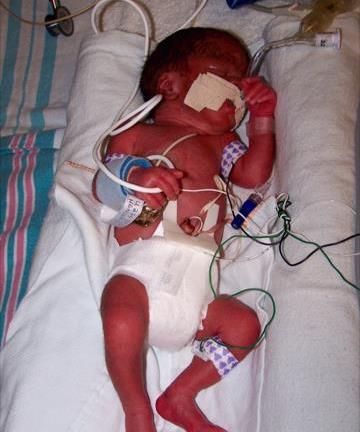
“He wasn’t putting on any weight, yet his stomach looked huge and swollen,” said Henderson. “The X-rays showed air bubbles in his intestines, which doctors later diagnosed as NEC.”
In the first few weeks of his life, Brennan underwent two surgeries, one of which removed a large part of his small intestine, before he was able to go home.
“When we were finally able to bring him home after spending nearly six months at the hospital, we were met with the challenges of his motility,” said Brennan’s father, Glen Henderson. “He was vomiting 13 to 14 times a day and had frequent loose stool.”
The family did their best to keep their home clean by laying blankets and pads on the floor. The laundry machine would be on constant rotation as Brennan would cycle through five to six outfits per day.
While managing Brennan’s intestinal motility issues, his parents also kept track of how he obtained proper nutrients given how much of it he would lose at one time because of the vomiting, along with his lack of small intestine which blocked the absorption of food and water he needed to survive. A central venous line, which was inserted in his body shortly after birth, was how he received intravenous feeding also known as total parenteral nutrition, or TPN for short.
To add to Brennan’s health concerns, he was diagnosed with cerebral palsy at 6 months old, which limited his mobility. However, the challenges he faced with both mobility and lack of intestinal function didn’t prevent him from going to school and being as active as he could possibly be.
“He needed to be followed by an adult at school to assist him when he had an accident,” said his mother Gloria Henderson. “Brennan was never embarrassed and wanted to continue going to school despite not having the freedom to do things on his own. Yet, the repeated vomiting during the day made him so tired that it affected his learning and growth as a student.”
A remarkable treatment comes with an uphill battle
Although Brennan made a little progress with intravenous feeding, he continued to have significant problems with vomiting and remained dependent on TPN until his family learned about a new trial being offered through Seattle Children’s Intestinal Rehabilitation Program.
“When Brennan was nearly 3 years old, I offered the opportunity for him to participate in a 12-week trial using teduglutide, a drug to treat short bowel syndrome that showed to be effective in adults,” said Horslen. “As soon as the treatment was available for pediatric use, we became involved in a clinical trial to examine its effectiveness.”

Seattle Children’s Intestinal Rehabilitation Program is the only program in the Pacific Northwest that brings together a team of specialists to restore intestinal function in children who have intestinal failure. Research shows that multidisciplinary teams like the one at Seattle Children’s make a big difference in reducing the health problems these children face.
Within 2 weeks of the 12-week trial, Brennan’s family noticed something remarkable – his chronic vomiting completely stopped.
“We couldn’t believe it,” said Henderson. “It was like a miracle. This was the first time in Brennan’s life that we had ever experienced him completely free of having to vomit multiple times in a day.”
Brennan was also able to cut down on TPN because he was no longer losing nutrients as fast.
However, after the 12-week trial ended and he no longer had access to the experimental drug, the incredible progress Brennan had made began to diminish. The vomiting returned and his TPN was increased once again.
“It was heartbreaking to see Brennan suffer from his old patterns,” said Henderson. “We knew we had to do something to make sure he had the treatment he desperately needed to live normally.”
The family did everything they could to get Brennan back on teduglutide – a treatment that can cost over $1,000 a dose.
“We first started by petitioning our insurance company to cover the treatment,” said Henderson. “When that didn’t work, we wrote a letter to the U.S. Food and Drug Administration to allow Brennan to have the treatment under ‘compassionate use,’ meaning he would be allowed to use it outside of a clinical trial. We ended up being denied.”
Having exhausted those options, there was one left that the family decided to try with help from Vickie Kuiper, an intestinal rehab nurse coordinator at Seattle Children’s.
“Vickie had cared for Brennan for several years and she knew the extent of his health issues and how well he did on teduglutide,” said Henderson. “She wanted to help him in any way she could.”
Kuiper decided to take a different approach by focusing on the financial costs associated with Brennan’s medical care.
“This time, we not only explained to our insurance what he was like on and off the treatment, we also outlined the costs of Brennan’s medical care,” said Henderson. “Without the treatment, Brennan would be in and out of the hospital on a frequent basis, costing our insurance a lot more than when he was on the treatment that kept him out of the hospital.”
After a suspenseful wait, the family received fantastic news that their request for Brennan’s treatment was approved.
A dramatic change for the family’s future
In June 2016, Brennan restarted his treatment using teduglutide, producing the same positive results he experienced the last time.
His continued use of teduglutide has allowed him to come off of TPN completely for the first time in his life.

“We are so grateful for Brennan’s wonderful care team at Seattle Children’s,” said Henderson. “Without them, we wouldn’t have learned about this ‘miracle’ treatment and wouldn’t have had the support and resources we needed to get it for him.”
Brennan’s life has dramatically changed thanks to the intestinal rehab team who offered the clinical trial using teduglutide to his family.
“It’s very gratifying seeing the clear change in patients like Brennan after they are introduced to a treatment,” said Horslen. “There’s been an evolution of intestinal rehabilitation and it’s been valuable in helping to prevent or reverse these types of health conditions affecting children.”
The Henderson family has experienced a newfound freedom for their family.
“It’s been life-changing,” said Henderson. “We can go on trips and not worry about hovering over him with bags and towels to clean up.”
Brennan, now 7 years old, has been taking full advantage of his renewed energy and good health by participating in sports like basketball, soccer and swimming.
“I remember he used to sit quietly by the side of the pool as he watched his older brother swim,” said Henderson. “Now, he’s able to join him. Simply seeing his smile and laughter makes me so happy.”
Resources:
- Seattle Children’s Intestinal Rehabilitation Program
- Seattle Children’s Gastroenterology and Hepatology

