 Julie Kobayashi, a 12-year-old girl from Hawaii, is Seattle Children’s third patient to receive the HeartMate II ventricular assist device (VAD), a device that allowed Julie to leave the hospital while waiting for a life-saving heart transplant. This is her story, from failing heart to transplant.
Julie Kobayashi, a 12-year-old girl from Hawaii, is Seattle Children’s third patient to receive the HeartMate II ventricular assist device (VAD), a device that allowed Julie to leave the hospital while waiting for a life-saving heart transplant. This is her story, from failing heart to transplant.
Julie Kobayashi started feeling sick on a Saturday in November 2013. She felt nauseous, but didn’t have a fever. The symptoms reflected that of the stomach flu. Her family wasn’t overly concerned at first. They thought the symptoms would subside and their daughter would be back to her normal self in no time. For Julie, an active and fun-loving 12-year-old, she usually didn’t let anything slow her down for too long.
When Monday rolled around, Julie felt well enough to go to school. She enjoyed school and had been working really hard practicing her clarinet for an upcoming concert. Missing school wasn’t an option in Julie’s mind.
Unfortunately, later in the week, Julie’s symptoms started to worsen.
“I noticed in P.E. that I was getting really out of breath. I was running really slowly,” said Julie. “I wasn’t my usual self. I’m usually really fast and at the front of the group in P.E. class.”
The next few days her symptoms would present like clock work. She would feel better in the morning, but progressively get worse. She wanted to continue to attend school normally, but her parents grew more concerned with each passing day. She wasn’t getting better. They began to wonder if Julie could be suffering from something other than the stomach flu.
On Nov. 26, the night before a class trip to Ice Palace, the only ice skating rink on the island, Julie felt at her worst. Despite feeling sick, she still wanted to go on the field trip, but her mother, Lori Kobayashi, had other plans. Julie would take a trip that day, but it would be to the doctor. Lori knew Julie needed to be seen by a doctor before Thanksgiving. They couldn’t wait.
Not stomach flu
When the doctor listened to Julie’s heart, it didn’t sound well. To determine what was wrong the doctor told Julie he would need to draw blood.
The needles were too much and no blood could be drawn. Julie fainted.
She was immeditately transported to Kapi’olani Children’s Hospital.
“We still didn’t know what was happening at that point,” said Lori. We just thought she was dehydrated. We thought everything would be fine.”
The news came as a complete shock. Julie was diagnosed with myocarditis, an inflammation of the myocardium, the heart’s muscle wall. In some cases, if it becomes severe, the heart cannot pump blood well to the rest of the body.
Julie went straight to the Intensive Care Unit (ICU) while her cardiologist began to evaluate if a heart transplant was needed. The family had three options for continued care: UCLA, Stanford, or Seattle Children’s Hospital.
“They gave us an option because they knew wherever we went for treatment, we’d be there for a while,” said Lori. “We had some cousins that lived near Stanford, so we thought that could be an option. But our cardiologist assured us that the collaboration he had with Seattle Children’s and Dr. Yuk Law would make the best fit.”
Waking up in Seattle
On Dec. 20, 2013, Julie was by herself on an air-ambulance to Seattle Children’s; her parents and little sister followed shortly after.
When Julie arrived at Seattle Children’s, she was greeted by a team of nurses, cardiologists and doctors, all there to make her feel comfortable until her family arrived.
It was Julie’s first time in Seattle. The change would be difficult at first, but she was determined to make the best of the situation. She focused on the better aspects of being so far from home. What excited her most was the thought of seeing snow, something she’d never seen before. It only took one day for her wish to be granted. Her second day at the hospital, Julie touched snow for the first time. It wasn’t falling from the sky, or pilled high atop a mountain, it was in a pink bucket, preserved just for her in a freezer.
A child life specialist in Hawaii, who previously worked at Seattle Children’s, called Seattle Children’s Child Life Department the day Julie was transported. She explained how eager Julie was to see snow and asked if it would be possible to make her wish come true. It was a wish Wendy Nicon, a child life specialist couldn’t ignore.
“It snowed the day Julie arrived,” said Nicon. “I went out to the playground at the hospital and shoveled snow into a pink bucket. I put it in the freezer just for Julie before leaving work that day. My job is to provide support to families, whatever that might look like. It’s not always as easy as giving someone snow. For Julie, it was meaningful. I’m glad I could help make her wish come true.”
It made the first day away from home a little easier. It was a sign that things might not be so bad.
The rest of Julie’s family arrived just in time for Christmas. They spent the day together, adjusting to their new normal. But shortly after Christmas, Julie started deteriorating.
Julie was diagnosed with Acute Cardiomyopathy, severe dysfunction of the heart muscle. The damage hurts the heart’s ability to pump blood and can lead to congestive heart failure.
Waiting for a heart transplant
On Dec. 28, 2013, Julie was listed for a heart transplant.
“She was in heart failure,” said Michael McMullan, MD, surgical director of Heart Transplantation at Seattle Children’s. “It takes a while for a heart to become available. Some patients can become so sick they don’t survive the process. For Julie, the best and safest way to get her to the heart transplant was with a Thoratec HeartMate II ventricular assist device (VAD).”
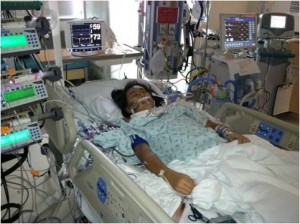 The day after New Years, on Jan. 2, 2014, Julie underwent surgery to implant a VAD, a device used to support patients with severe heart failure. It serves as a bridge to heart transplantation. The VAD pumps blood through the body for the heart and allows the heart muscles to rest and recover. It also allows patients the ability to leave the confines of the hospital while waiting for a transplant.
The day after New Years, on Jan. 2, 2014, Julie underwent surgery to implant a VAD, a device used to support patients with severe heart failure. It serves as a bridge to heart transplantation. The VAD pumps blood through the body for the heart and allows the heart muscles to rest and recover. It also allows patients the ability to leave the confines of the hospital while waiting for a transplant.
“The VAD allows patients to recuperate. Sometimes the heart will get better,” said McMullan. “With Julie, however, her heart failure was more chronic in nature, and took longer to develop. Without the VAD, she would have been stuck in bed waiting for a transplant. The VAD allowed her to rehabilitate and made her healthier, allowing her lungs and kidneys to work better. It also improved her chance of surviving until a heart became available.”
Julie went into recovery, a VAD in place. She finally started to feel better.
Each day was better than the last. Slowly, she was weaned off the many tubes protruding from her small body. The VAD was working. She was finally untethered from her bed and able to leave the hospital.
“I hadn’t been able to walk out of a hospital since Nov. 27,” said Julie. “With the VAD, my parents didn’t always need to be by my side. I liked to think I was my old self again.”
Julie’s heart had taken a toll, she still needed a heart transplant, but at least the family could wait for her new heart outside the hospital walls.
“The hard part is waiting”
Julie was discharged from Seattle Children’s on Feb. 4, 2014. With the VAD she had to stay in the Seattle area, but the idea of merely stepping outside of the hospital was liberating.
Julie made a list of everything she wanted to see and do while she waited for her new heart.
- Pikes Place Market
- See real snow, not snow in a bucket
Her list was short. And in no time at all it would get even shorter.
 On Feb. 7, 2014, it started to snow in Seattle. For the Kobayashi family, it was a sight they’d never seen before. The odds that it would snow in Seattle while Julie could leave the hospital with a VAD was nothing short of miraculous.
On Feb. 7, 2014, it started to snow in Seattle. For the Kobayashi family, it was a sight they’d never seen before. The odds that it would snow in Seattle while Julie could leave the hospital with a VAD was nothing short of miraculous.
The next day, the family made their first snowman and learned the art of making snowballs. It was a magical day for the Kobayashi family. They played together in the snow for hours, and forgot for at least a little while that their daughter was waiting for a heart.
Getting the call
Exactly one week after being discharged from Seattle Children’s they got a call. They had an offer for a heart.
Julie was in disbelief. She thought her dad was playing a joke on her. She didn’t think she’d be lucky enough to get a heart so quickly. She already had plans set for later in the week, field trips and a dinner date with a family whose child also received a VAD at Seattle Children’s earlier in the year. She was just getting used to her new independence. She was getting back into a normal routine thanks to the VAD. Now, she would be headed back to the hospital.
But it finally sank in.
“I have a heart!”
Preparing for a heart transplant
When the family arrived at Seattle Children’s Julie started to feel a little anxious.
“I got over the fact that I would need a heart transplant,” said Julie. “What really bugged me was knowing my heart belonged to someone else. Something bad happened to them. You just feel bad that they had to go through something so tragic. It was hard to believe that something bad had to happen to another person to help me live.”
Julie came out of surgery around 3:30 a.m. on Feb. 12, 2014. She had a new heart.
Out of transplant and into the Cardiac Intensive Care Unit (CICU), the surgery went very well. After only a week, she moved to the surgical unit.
“She’s exceeding expectations,” said Lori. “She’s making a really rapid recovery. Each day is a step forward.”
The road ahead

Julie and her family will still need to spend a couple months at Seattle Children’s before traveling back to their home to Hawaii, but for the time being, the Kobayashi family is settling into a routine in Seattle, and making the best of their home away from home.
“Julie is doing great,” said McMullan. “Once our cardiologists feel she’s safe, she can go back to Hawaii and live normally. The goal is to allow her to live whatever life she wants. She can be whatever she wants to be.”
And now she has that chance.
“Through everything, we’re so thankful our doctor recommended Seattle Children’s. We know we made the right choice for Julie,” said Lori. “From the nurses to the doctors, everyone we’ve met has been compassionate and caring. They’ve taken such good care of Julie and us. They’ve given us support along the way. From the days leading up to Julie’s transport from Hawaii, until now, everything you can think of has been coordinated and handled for us – transportation to and from the Ronald McDonald House, massages, hair cuts, school and support for our youngest daughter. It’s relieved so much stress for us. Even though our situation may be hard at times, Seattle Children’s keeps parents in the best possible state. They just make it easier.”
Resources:
- Seattle Children’s Heart Center
- Heart Center patient stories
- New heart device at Seattle Children’s improves patients’ survival rate and quality of life
If you’d like to arrange an interview with the Heart Center or the family, please contact Seattle Children’s PR team at 206-987-4500 or [email protected].

