
Chrissy Ehlinger had a very normal pregnancy, so when her son Carter was born she had no concerns about his health. He was beautiful and perfect and looked like any healthy baby should. It wasn’t until a simple, inexpensive and non-invasive newborn screening test called pulse oximetry screening revealed the unthinkable.
Pulse oximetry testing is not required in every state, even though it is recommended by the United States Department of Health and Human Services, the American Heart Association, the American College of Cardiology, and the American Academy of Pediatrics.
Fortunately for Chrissy, the hospital where baby Carter was born elected to do pulse oximetry testing on newborns. Here, Chrissy recounts how that decision saved her little boy’s life.
Carter’s story
While pregnant with our second child, we were living on Eielson Air Force Base just outside of Fairbanks, Alaska. This pregnancy was much like the first – fairly uneventful and pretty tiring. We had the usual ultrasound of the baby, including his heart, at 20 weeks and I naively thought that meant everything was perfect. I had no fears about the baby’s health.
Just after midnight on Sept. 12, 2012, my water broke. We were ecstatic! Little Carter Thomas came into the world at 1:11 p.m. The instant I saw him I could see how beautiful he was. We were blessed with another healthy baby boy.
However, that night was a little rough. I was having difficulty nursing and Carter wasn’t sleeping very well. I wasn’t very good at breastfeeding my first son, so I wasn’t alarmed when Carter was just as difficult.
The next day, I was anxious to get home. The staff was busy with the last of the newborn tests for Carter and the discharge paperwork for me. My husband had packed up our car and was ready to go. The nurse came into our hospital room to retrieve Carter for one last test.
But they never brought him back.
Waiting for Carter’s test results
Too much time had passed, and having done this before, I knew it was taking longer than it should have. The minute the nurse walked into my hospital room without Carter, my heart sank. My mother instinct told me something was wrong, and unfortunately, my instinct was right.
I was informed that Carter’s tests weren’t coming back normal and they needed to perform a few more tests to see if they could get answers.
Panic stricken, I started making phone calls. How could something be wrong with my perfect little baby? That’s the only thing that kept passing through my mind. I didn’t quite understand at the time, but Carter had failed a routine pulse oximetry test, which can help discover critical congenital heart disease (CCHD) in newborns. The test monitors the baby’s oxygen saturation in the body. Unfortunately, the test indicated that something was potentially wrong with Carter’s heart.
Our trip home would have to wait
The next piece of news we received was also quite unsettling. Carter was going to have to be flown to Anchorage, Alaska to see a pediatric cardiologist. My thoughts went immediately to our 2-year-old who was staying with a friend. Only one parent could fly with Carter to Anchorage, so I sent my husband, Nick, to retrieve my overnight bag from the car, and he headed home to see our 2-year-old. My family would have to join me later. I couldn’t leave Carter’s side and we needed to find out what was wrong with his heart.
Hooked up to tubes and monitors, we prepared to fly out. I remember thinking how much I wish I could hold him. At that point, everything was surreal. It was more like a dream – or rather a nightmare – and little did I know the news would get worse before it got better.
Diagnosing Carter
I received the news in the neonatal intensive care unit (NICU) at Providence Alaska Medical Center from Dr. James Christiansen, a pediatric cardiologist at Seattle Children’s Pediatric Cardiology of Alaska based in Anchorage. Carter was born with a heart defect called transposition of the great arteries (TGV). His body was not receiving the oxygenated blood that he needed, and he would need to be flown to Seattle Children’s Hospital in Seattle for open heart surgery. The news made the floor drop out from under me.
I couldn’t believe what was happening to my beautiful baby boy. I was already miles from home, alone, with my small overnight bag, and now we were headed to Washington in a few hours for an unknown period of time. Before this moment, I didn’t know anything about heart defects. All of the sudden, I was immersed in a new world, unexpected and terrifying. I learned that heart defects are more common than you may think, but you never believe it will happen to your child.
A trip to Seattle Children’s saved Carter’s life
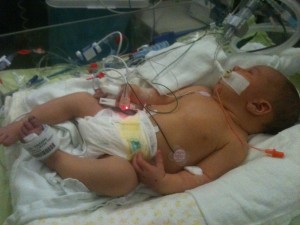
I don’t remember a lot after we arrived at Seattle Children’s, but that’s only because everything went so smoothly. From the first moment we stepped into the hospital we had a team by our side. I remember being so tired, from giving birth, from traveling so far. It was an extremely exhausting experience, both physically and mentally. One of the nurses immediately took me by the hand, got me a room and made a bed for me. She made sure I took care of myself. She told me, “You can’t take care of Carter without taking care of yourself first.”
The experience gave me a completely different perspective. You have to be a certain type of person to be a nurse, but until that moment, I didn’t realize how remarkable and compassionate you truly have to be. I was so very thankful for her.
We had a team of doctors, nurses, cardiologists and surgeons all attending to us, all attending to Carter. It was truly remarkable. Every day the team kept us in the loop as to what was going on. I was never worried. I loved listening in on rounds. I couldn’t understand everything the doctors would discuss, but if I had a puzzled look on my face, they’d happily explain what they were talking about.
And after a week in the NICU at Children’s, Carter underwent his life-saving heart surgery. Pediatric heart surgeon Dr. Michael McMullan was incredible.
During the surgery they gave us a pager. We got updates throughout the surgery and were able to call whenever we had questions. It made the situation a lot less stressful for us.
After only two weeks, and an amazingly speedy recovery, we headed home to Alaska with our little bundle of joy. He was now not only beautiful, but finally healthy, thanks to Seattle Children’s.
The importance of screenings
Pulse oximetry testing and Children’s saved little Carter’s life. Without pulse oximetry testing, we would have brought Carter home only to end up in a dire, life-threatening situation. Thankfully, the test did what it was supposed to do.
Where Carter is today
 Today, Carter sees a pediatric cardiologist every six months, as a precaution. It’s hard to tell when looking into Carter’s big, blue, smiling eyes that he’s had a rough start to life. Anyone who meets him sees a sweet, energetic 15-month-old boy. He is truly special and everyone who meets him knows it.
Today, Carter sees a pediatric cardiologist every six months, as a precaution. It’s hard to tell when looking into Carter’s big, blue, smiling eyes that he’s had a rough start to life. Anyone who meets him sees a sweet, energetic 15-month-old boy. He is truly special and everyone who meets him knows it.
Carter is living proof of why pulse oximetry screening is so important. For him, the test was lifesaving.
About pulse oximetry testing
Seattle Children’s has been educating the region’s care providers about the importance of universal pulse oximetry screening. Currently, Washington State does not require pulse oximetry screening on newborns.
“Our emphasis is on being a regional resource for training so that screening is not only implemented, but implemented well,” said Amy Schultz, MD, a pediatric cardiologist at Seattle Children’s, and co-leader of the Pulse Oximetry Screening Team.
Resources:
- Seattle Children’s Heart Center
- Seattle Children’s Neonatology
- Pulse oximetry Screening for Critical Congenital Heart Disease
- Seattle Children’s Pediatric Cardiology of Alaska
If you’d like to arrange an interview with a doctor in the Heart Center please contact Seattle Children’s PR team at 206-987-4500 or [email protected].

