You’ve probably seen it before: something falls, a loud noise ensues, and a cat with an arched back and poofy tail sprints away.
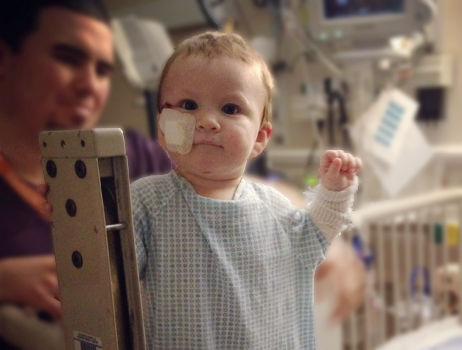
Unfortunately for 7-month-old Spencer Nicholson, when he loudly pulled a bin off a pantry shelf, the family cat was spooked right in his direction. Spencer fell on the floor and the cat, claws out, ran him over. Spencer was left with a deep scratch on his right cheek.
His mom, Kelsey Nicholson, took Spencer to urgent care near their home in Arlington, Washington, where she received a prescription for antibiotics. But hours later, Spencer’s face started to swell. By that evening, Nicholson was so concerned that she took her baby to the emergency room at her local hospital.
Doctors told Nicholson the swelling was probably due to cellulitis — an infection under the skin — but sent them to Seattle Children’s because something just didn’t seem right.
At Seattle Children’s, doctors examined little Spencer’s face, trying to figure out why it had swelled so dramatically.
“It took about two hours before somebody finally said, ‘You know, we don’t think it is…but it could be necrotizing fasciitis,’” said Nicholson. “My heart dropped and I had this all-encompassing fear of not knowing what was going to happen.”
Spencer the zebra
Necrotizing fasciitis — commonly known as flesh-eating bacteria — was the last thing Nicholson expected, or wanted, to hear. She recalled a recent news story about a teenage girl who lost most of her limbs when she contracted the disease. The only way to truly diagnose it is through exploratory surgery.
The surgery resident who saw Spencer in the Emergency Department that night called Dr. Richard Hopper, chief of craniofacial and plastic surgery, about Spencer’s case. It was 2 a.m., but if it was necrotizing fasciitis, the team had to act quickly to save Spencer’s face, and possibly his life. The disease spreads fast and becomes life-threatening very quickly.
Hopper came to the hospital right away, and the team took Spencer into surgery. Nicholson’s worst fears were confirmed: Spencer had necrotizing fasciitis in his face.
“It’s really bad, it’s really scary and it’s in my 7-month-old,” recalled Nicholson.
Nicholson remembers the care team telling her about a phrase in medicine: ‘When you hear hoofbeats, think of horses, not zebras.’ Horses refer to a common diagnosis, while zebras refer to a rare, exotic one. “My kid was the zebra,” she said.

Spencer underwent three surgeries to remove the dead, infected tissue in his face.
“As Dr. Hopper put it, this disease is like wildfire,” said Nicholson. “You have to get in front of it and take out all the tissue or it’s going to keep coming back.”
The surgeries were successful, and after a week in the Pediatric Intensive Care Unit, and another week in the Medical Unit, Spencer was sent home.
Now, as an active, spunky 4-year-old, Spencer is just like any other kid.
“He’s alive and able to drive us crazy thanks to Seattle Children’s,” said Nicholson.
Although Spencer has a scar that runs from his right eye back toward his ear and down his face, over the years it has faded so much that it’s hardly noticeable. The spot on his cheek from the initial cat scratch is actually a bigger scar, said Nicholson.
A profound impact
Last year, Nicholson left her job for a role at Seattle Children’s Research Institute.
“How do you not want to work for the place that’s had such a profound impact on your life?” she said.
As the administrative assistant for Dr. David Rawlings, director for the Center for Immunity and Immunotherapies, Nicholson loves working in the midst of research that’s leading to new therapies and cures. The experience has inspired Nicholson to give back to Seattle Children’s over the years.
“Things like what happened to Spencer happen. They’re random and chance, so I want to make sure that if someone is in the same situation we were in, there are funds to help that family,” said Nicholson. “We were lucky that we were able to absorb the cost of Spencer’s medical bills, but not everybody is.”
Nicholson knows firsthand the human component that makes the scientific work taking place at one of the nation’s top pediatric research centers meaningful.
“I like to remind others that there’s a face of someone who is benefiting from what we do,” said Nicholson. “I want to help them remember that face. My kid is that face.”
Resources
- Plastic surgery at Seattle Children’s
- Unique protocol for flesh-eating bacteria helps Trey get back to life
- Ways to give back

