The following is part 2 of our two-part series on ECPR, a combination of CPR and ECMO offered at Seattle Children’s Hospital to save the most fragile patients’ lives. Part 1 covered Hannah Mae Campbell’s incredible story where ECPR and a heart transplant saved her life and allowed her to be the thriving toddler she is today. Here, we discuss how Seattle Children’s has spearheaded a first-of-its-kind ECPR simulation program to improve the process that allows the hospital to save patients in a time of crisis.
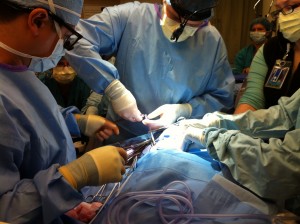
ECPR takes place when a patient goes into cardiac arrest, does not respond to CPR and is then put on Extracorporeal Membrane Oxygenation (ECMO), a machine that functions for the heart and lungs when the organs fail or need to rest. Hannah Mae Campbell’s experience demonstrates the importance of technology like ECMO and why it’s important to continually improve complex, life-saving processes like ECPR.
Since January of this year, Seattle Children’s has executed the largest-scale ECPR simulations in the nation, with medical staff coming together bimonthly to practice as though they were in a real ECPR situation. Even though Seattle Children’s ECPR outcomes are higher than the national average, the hospital initiated the simulations with the goal of standardizing each step of the process to further improve outcomes for patients.
“Refining the process and providing this hands-on education for the nurses, surgeons and staff in our intensive care units is critical to ensure we can do very complicated things very well in a time of crisis,” said Dr. Taylor Sawyer, neonatologist and director of the Neonatal Perinatal Fellowship Program. “As they say, practice makes perfect and we want everything to run as smoothly as possible when we’re dealing with low frequency, high risk events like ECPR.”
Dr. Michael McMullan, surgical director of Cardiac Transplant and director of Mechanical Cardiac Support and ECLS Services at Seattle Children’s, says ECPR benefits many patients because when their heart stops, that’s not the end. But the goal in improving each step of the process goes beyond just saving patients’ lives.
“With the simulations, we strive to do everything better to not only increase survival, but also to improve neurological outcomes in patients and lessen brain injury due to lack of oxygen,” said McMullan. “We want these kids to do more than just survive; we want them to go on to have a high quality of life.”
What makes ECPR so complex?
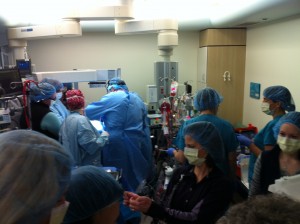
ECPR is an incredibly rare, technical event that involves a large team of more than 20 nurses, doctors, surgeons and other specialists who must work seamlessly together – very quickly – in order to save a patient’s life.
Once a child goes into cardiac arrest, CPR begins. If the child is not responding to the artificial breathing, chest compressions and epinephrine typically used in CPR, a decision is then made by the medical team and the child’s parents whether or not to put the child on ECMO, which can act as a bridge to the next phase of treatment. If it’s decided to put the child on ECMO, the EMCO team rapidly assembles to begin the process. The ECMO machine must be prepped and surgeons must operate, connecting the patient to the machine, which is called cannulation – all while chest compressions continue. Of course, it’s difficult for a surgeon to operate while chest compressions are being administered, and so the two physicians must alternate in a methodical fashion.
“There are a lot of moving parts that have to be choreographed in order to accomplish the end goal of successfully getting the patient stabilized on ECMO,” said Dr. Joan Roberts, director of Critical Care Simulation. “It’s almost like a dance where every person must perfect their role and have timing down to a tee.”
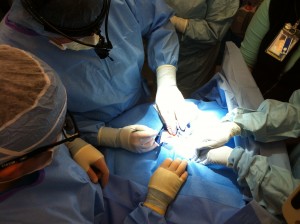
The simulation team strives to make the experience as realistic as possible. In every simulation, teams practice using a state of the art, high-fidelity pediatric simulation mannequin from the Seattle Children’s Learning and Simulation Center, which has been specially modified for ECPR training. The mannequin is controlled by a simulation technologist and provides feedback on how well chest compressions are being done, and whether or not the patient has been successfully connected to ECMO.
“There is a great deal of realism and energy in each simulation and everyone in the room gets really caught up in what’s going on as though we’re working on a real patient,” said McMullan. “We also stress the system where we incorporate problems and figure out the best trouble shooting. That’s how you really improve.”
The simulation team also uses an innovative ECMO cannulation simulation system that was developed at Seattle Children’s. McMullan said the system is so unique and effective that his team has trained physicians from around the world on how to use it in their own hospitals, and it is now being used globally.
Improving the ECPR process
So far this year, about 185 staff members at Seattle Children’s have participated in the simulations, and several improvements have already been made.
One particular area of focus has been on finding ways to ensure that high-quality CPR is maintained because chest compressions are often required for extended periods of time until the patient is stabilized on ECMO. High-quality CPR means that the depth and speed of chest compressions are correct and the numbers of interruptions are minimized. This is especially important for patient’s neurological outcomes.
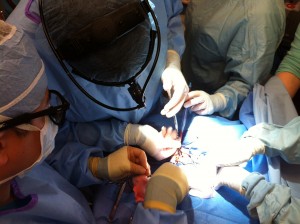
To address this, Roberts and Dr. Silvia Hartmann, an intensive care unit fellow, found that the use of a metronome was an effective tool for keeping the best rhythm for compressions. Therefore, the team will be using defibrillators that have metronomes built into them, she said.
Another key area of improvement has been in improving the sequence for how and when the surgeon operating and the physician doing chest compressions alternate, minimizing the number of compression interruptions.
“We have refined the process of CPR during cannulation, designating that the staff member providing CPR will keep time and notify the surgeon of how much time has passed without CPR,” said Sawyer.
The goal is for the surgeon to operate for a designated period of time, ideally less than one minute, and then resume compressions for at least one minute to ensure the patient is receiving adequate CPR.
Staff members who have been involved in the simulations have also expressed much greater comfort with ECPR, and feel much more confident in their role and what to expect. The ECMO specialists have commented that these simulations feel almost like the real thing and they have increased their comfort communicating with the surgeons during the cannulation process, Sawyer said.
“Overall, we’ve seen a lot of progress in improving teamwork, communication and coordination between the medical and surgical teams, we’ve optimized techniques for administering CPR and we’ve established effective protocols for each key step in the process,” he said.
Roberts adds, “The simulation-based training has also been effective in allowing staff to train in a safe environment where they can try new things to maximize patient outcomes, and then debrief and discuss what worked well.”
Sharing key learnings with the medical community
At the end of this year, the simulation team will be compiling data and key learnings from the simulations and submitting them for publication in hopes of better educating the medical community about the best way to perform this life-saving process. The team is also planning to conduct a study evaluating the clinical impact of the simulation-based training.
“We’ve taken all of the steps involved in ECPR and improved on each one to make the process better and more efficient, which we hope will lead to better outcomes for our patients,” said Sawyer. “Since we were the first to really study this process on such a large, in-depth scale, we feel that it’s important for us to take these critical findings and share them broadly for others to learn from as well.”
Resources:
- Seattle Children’s Learning and Simulation Center
- Seattle Children’s Heart Center
- Seattle Children’s Neonatology program

