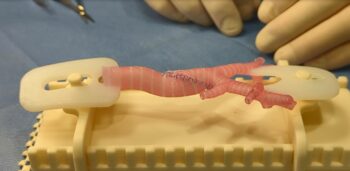
Healthcare organizations are increasingly looking to incorporate the use of 3D-printed models to help improve outcomes for pediatric patients in need of very complex surgeries. Doctors at Seattle Children’s are now utilizing 3-D printed models created in the hospital’s Innovation Lab to train international care teams in a highly specialized procedure, known as a slide tracheoplasty, that improves airflow in a child’s obstructed airway.
The 3D-printed airways for the slide tracheoplasty — an extremely complex surgery that involves dividing a child’s windpipe at a precise location and angle, and can have a higher mortality rate than other open airway procedures –have been in high demand. This year, Seattle Children’s Dr. Kaalan Johnson, an otolaryngologist, has shared his expertise with surgeons in numerous countries around the world, including Argentina, Fiji, Costa Rica, England and South Africa by distributing hundreds of the 3D-printed tracheas and providing trainings for this challenging surgery.
This work was recently featured on KING 5’s Healthlink alongside the project’s collaborator Dr. Seth Friedman, manager of Innovation Imaging and Simulation Modeling at Seattle Children’s.
“This allows (for) a much more equitable distribution of experience – getting prepared for not just the procedure itself, but also patient-specific preparation for surgeries,” Johnson recently told KING.
Most recently, Johnson mentored doctors at the Garrahan Children’s Hospital in Buenos Aires on the implementation of 3D-printed models for improved airway surgery precision, which led to the first of its kind pediatric workshop in Argentina.
“People are learning how to do this procedure that was just never possible before, except to see this picture in a text book,” explained Friedman. “This has been very impactful because it’s actually training the next generation.”


Johnson says that without training like this some doctors around the world are put in a difficult position of either not attempting the surgery at all – which could be fatal for patients in need – or doing their best with the resources and training that they have available.
“I think that in most of these cases, international surgeons are put in a situation where giving it a shot is the best alternative within their power to provide for these families who are desperately seeking a solution for their child,” said Johnson.
However, through this global effort and unique collaboration, outcomes can be improved for patients.
More than 500 3D-models have been developed and printed in Seattle Children’s Innovation Lab, and interest continues to grow.
3D-modeling also enables doctors with a unique ability to show families precisely what a surgeon is going to be doing during a procedure.

“It’s a much more helpful device rather than using a whiteboard for example,” added Friedman. “Parents would likely feel better knowing that there is a lot of practice going on before some of these major, complex surgeries.”
Johnson plans to travel to more international destinations to continue to train teams abroad in the year ahead.

