
In December of last year, Laura Coffman began to notice that something wasn’t quite right with her 2-year-old son, Hunter. He was leaning to one side and seemed to lose his balance easily. When he became lethargic and started vomiting a few days later on Dec. 28, she knew it was time to see the pediatrician.
After all standard tests came back normal, they were sent to Seattle Children’s for further testing and to find an answer. Unfortunately, it was far worse than anything Coffman could have imagined.
“What I thought was probably just Hunter being a wobbly toddler with a virus turned out to be a brain tumor,” said Coffman. “I will never forget that day. It was the most traumatic six hours of our lives.”
Tumor Paint sheds some light
Hunter was immediately scheduled for surgery to remove the brain tumor that was the size of a golf ball. In preparing for the operation, Coffman and her husband, Atom, were also presented with the opportunity to enroll Hunter in Seattle Children’s Phase 1 trial of BLZ-100 Tumor Paint. Since tumor cells can be difficult to distinguish from healthy cells, the drug aims to improve surgical outcomes by acting as a molecular flashlight that allows surgeons to visibly distinguish a tumor from normal brain tissue.
 “We didn’t see how it could hurt and we wanted them to use every tool at their disposal so we enrolled him in the trial,” said Coffman.
“We didn’t see how it could hurt and we wanted them to use every tool at their disposal so we enrolled him in the trial,” said Coffman.
Dec. 30 was the day of Hunter’s surgery. Another day the Coffman’s will never forget.
“As a parent you know that your child may never be the same after brain surgery – they may not be able to see, walk or speak,” Coffman said. “It’s the risk you have to take to save their life. But we trusted our surgeon, Dr. Amy Lee, with everything we had.”
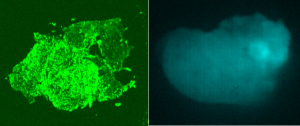
Prior to surgery, BLZ-100 Tumor Paint was administered by intravenous injection. In the operating room, the tumor glows green when viewed under a laser light and imaged with a near-infrared camera system.
BLZ-100 Tumor Paint was invented by a team led by Dr. Jim Olson, pediatric neuro-oncologist at Seattle Children’s and Fred Hutch and co-founder of Blaze Bioscience: The Tumor Paint Company. While this Phase 1 trial is focused on examining the safety of the drug and how well it targets tumor tissue, the hope is that it will eventually help guide skilled surgeons to prevent the removal of healthy tissue that can lead to serious long-term side effects.
“Cure is not just about successful treatment of a tumor, but successful treatment of a child,” said Dr. Sarah Leary, principal investigator for the trial and Hunter’s oncologist at Seattle Children’s. “Much of cancer treatment for children is a trade-off where curative therapy comes with serious long-term side effects. By lighting the way for expert surgeons, we’re hopeful that BLZ-100 Tumor Paint could help improve the quality of life for children by reducing treatment-related damage to the healthy brain.”
Hunter’s surgery went well and the majority of his tumor was removed. One small piece on his brain stem was intentionally left because removal may have led to serious neurological injury.
After surgery, it was not long until Hunter was back to his young self.
“We were incredibly lucky to have such an amazing surgeon and we were thrilled that he was able to bounce back so quickly,” said Coffman. “He was able to walk, run and put words together only weeks after the operation.”
A terrifying diagnosis, the journey to remission
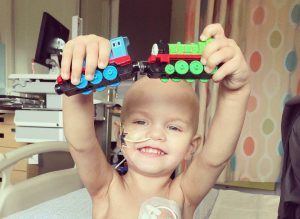 Once the tumor was removed, the Coffman’s faced their next hurdle as pathology determined that Hunter had a form of aggressive cancer called medulloblastoma. His next phase of treatment quickly began as he underwent seven months of chemotherapy and radiation to target the remaining tumor, as well smaller lesions in his brain and spine.
Once the tumor was removed, the Coffman’s faced their next hurdle as pathology determined that Hunter had a form of aggressive cancer called medulloblastoma. His next phase of treatment quickly began as he underwent seven months of chemotherapy and radiation to target the remaining tumor, as well smaller lesions in his brain and spine.
“I remember how terrifying that diagnosis was to hear, but Dr. Leary was so optimistic and immediately reassured us when she said ‘this is a cancer that we’ve cured many times,’” said Coffman. “And that’s exactly what they did.”
In August, four weeks after Hunter ended treatment, MRI scans confirmed he was in remission.
“The news was phenomenal – all of his cancer was gone,” she said. “You can’t ask for anything more.”
Today, Hunter is thriving.
“You’d never even know he had cancer or brain surgery,” she said. “His hair is growing back, he’s swimming, impressing us with his speaking skills and having playdates with friends.”
When reflecting on their decision to participate in the trial, Coffman is glad they had the opportunity to experience something that could be a game changer for future kids like Hunter.
“Brain surgery is not something you ever want to think about your child going through, but if that dreadful day ever comes, you definitely want a tool like Tumor Paint that could help guide the surgeon in making potentially life-altering decisions,” said Coffman.
What’s next for BLZ-100 Tumor Paint in children
Since the trial began in June 2015, Seattle Children’s has performed 15 brain surgeries with BLZ-100 Tumor Paint. To date, none of the patients have had any negative side effects and Leary and her team are working to determine the best dose. The drug also appears to be doing what it was designed to do – make tumor tissue glow.
“We have been excited to see that BLZ-100 Tumor Paint is binding to many different types of brain tumors in children and so far has not resulted in any side effects,” said Leary. “We are optimistic that in the future it could be an incredible tool when placed in the expert hands of a neurosurgeon that could lead to improved patient outcomes.”
Dr. Amy Lee, the lead neurosurgeon in the trial and Hunter’s surgeon, adds, “We believe BLZ-100 Tumor Paint holds tremendous potential and eventually could be a valuable aid for surgeons in differentiating tumor from healthy tissue, particularly when there are areas of question.”
Leary said their goal is that this Phase 1 trial at Seattle Children’s, which has the largest pediatric Brain Tumor Program and the most pediatric neurosurgeons in the Northwest, will be followed by other studies that lead BLZ-100 Tumor Paint to become a part of standard care for brain tumor surgery. The next step will be to determine the effectiveness of the drug, which will involve a larger collaborative study that will involve 15 of the leading pediatric brain tumor centers across the country.
“In the future, I hope we’ll look back and wonder how these surgeries were ever done without the lights on,” said Leary.

