My daughter pushes my hand away abruptly and the spoonful of food goes flying. I turn to her twin to coax her to eat a spoonful of puréed lentil soup, and she promptly gags on the tiniest lump and spits it out. Typical case of the terrible twos? No, they are 3 and a half, […]
Morgan Wood has been coming to Seattle Children’s since he was born — and as an adult, he continues to benefit from recreational and social skills classes at the Alyssa Burnett Adult Life Center. He is known among both friends and providers for sharing his life mantras, which he developed to work through challenges related […]
My first Mother’s Day was in 2004. I anticipated sleepless nights and lots of happiness around the arrival of my first son, Adam, due in early May. Instead, there were potted plants and sympathy cards and a single white rose in a blue vase after my son was stillborn just before midnight on April 24. […]
In honor of World Kidney Day, On The Pulse shares the inspirational story of 5-year-old McKinley Miller who was born with just one kidney that did not develop normally. “She’s our little miracle,” said McKinley’s mother, Jennifer Miller. “We want other people to know there’s always hope. All you have to do is look at […]
Watch little Alexis (Lexi) Melton, 7, Irish dance across a stage, or effortlessly ski down a slope, and you would never guess the hurdles she’s had to overcome in her short life. When Lexi was born, her family didn’t know if she would survive. Her extremely rare craniofacial condition literally makes her one in a […]
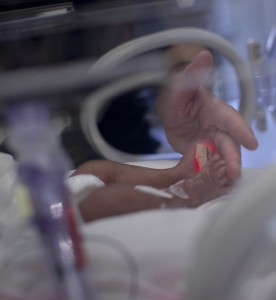
Every new mom hopes to have a healthy baby who enters the world right on time. But unfortunately, deliveries don’t always go as planned, and some babies arrive too soon. Preterm birth, which according to the CDC occurs when an infant is born before 37 weeks of pregnancy, affects about one out of every 10 […]
Worldwide, preterm birth is the leading cause of death for all children under age 5, taking the lives of more than 1.1 million children every year. Now, new research utilizing the emerging field of systems biology aims to harness big data in an effort to reduce the global burden of preterm birth. Seattle is well […]
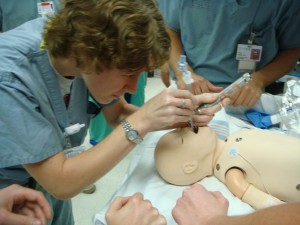
All new parents hope for a healthy delivery, but in the rare instance that an unexpected medical issue arises as baby enters the world, it’s crucial that the newborn delivery and transport care teams are well versed in performing neonatal emergency procedures. Breathing difficulties are some of the most frequent unexpected medical issues in newborns, […]
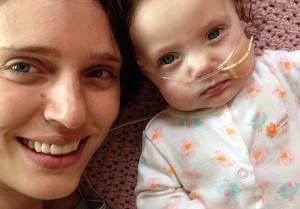
Everything went perfectly when Amanda Erickson’s first baby was born. Bennet arrived right on time on March 11, 2012, healthy and eager to nurse. Exactly two years later – on March 11, 2014 – Bennet’s sister, Juliette, came into the world. This time, says Erickson, “it was an adventure birth.” In other words, nothing went […]
On May 1, Dr. Tom Hansen will step down as Seattle Children’s CEO after 10 years of service. During his leadership, Hansen was known as a visionary with big ideas – big ideas that helped us become one of the best children’s hospitals in the world while getting us closer than ever to achieving our […]