
When asked about the birth of her daughter Harper, Sydney Beare lights up.
“Harper was 8 pounds, 1 ounce, 21.5 inches and the most beautiful baby I’ve ever seen!” she said.
By all accounts, Harper was an exceptionally happy, and seemingly healthy, baby. She began sleeping though the night when she was just a few days old and almost never fussed, even when teething. Beare said her daughter was “totally content.”
But in July 2017, when Harper was 9 months old, she became seriously ill.
Harper first developed an ear infection, a staph infection and had an infected cut on her finger. During the next month she became lethargic and pale.
Beare noticed bruises on her legs, and later on her back and face. Harper began having diarrhea and vomiting. She also slept all the time. Despite all this, Harper’s well-child checkup in August revealed no concerns.
Then, on Aug. 21, Harper woke up with a fever.
“She was just lying there, with dry, cracked lips, screaming,” Beare remembered, choking back tears. “I was worried something was wrong but I pushed that idea aside because I didn’t want to think anything bad could happen to my baby.”
“Our lives completely changed”
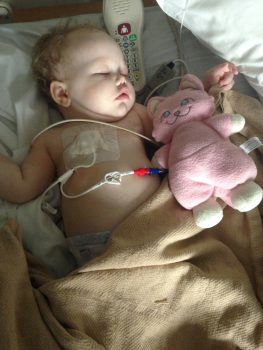
Beare took her daughter to the nearest pediatrician who immediately referred her to an emergency department.
“I thought, ‘Maybe she has a bug and is dehydrated.’ I was sure it would be a quick clinic visit,” she said.
But a doctor soon informed Beare that Harper had acute lymphoblastic leukemia (ALL).
“It took my breath away,” Beare recalled, struggling to speak. “I didn’t know it could happen to somebody so young. In that moment, our lives completely changed. We couldn’t go back home; we just hit the ground running.”
Beare and Harper were immediately taken by ambulance from their small hometown in Idaho to Sacred Heart Hospital in Spokane.
“I just kept thinking, ‘No. No. This is not OK.’ I just held her and cried,” Beare said.
At the hospital, Beare learned her daughter had a 40% chance of surviving. They started a treatment plan that would include two years of chemotherapy.
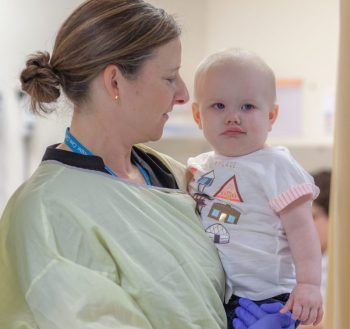
For months, Harper was known as “the superstar patient.” She had few side effects and was happy and charming, learning to walk in the hospital halls and blowing kisses to everyone she met.
But after the four rounds of chemotherapy, it was clear Harper’s leukemia was not responding to the treatments. Her oncologist said the best chance of surviving would be to go to Seattle Children’s for chimeric antigen receptor (CAR) T-cell immunotherapy. She would also be part of Seattle Children’s High-Risk Leukemia Program where experts in research, diagnostics and treatment work closely as a team throughout a patient’s journey to ensure the best possible outcome.
Giving Harper a chance
T-cell Immunotherapy is a method of treatment where a patient’s T cells (white blood cells in the immune system that fight infection) are reprogrammed so they can seek out and destroy cancer cells wherever they are hiding in the body.
“Historically, patients like Harper did not survive,” explained Dr. Rebecca Gardner, an oncologist and former associate medical director of Seattle Children’s Immunotherapy Integration Hub. “When her oncologist reached out to us, we all agreed she needed a bone marrow transplant, but she needed to be in remission first. We believed T-cell immunotherapy was her best option to get there.”
Harper qualified for PLAT-05, a first-in-the-nation pediatric phase 1 trial at Seattle Children’s that tests the safety and feasibility of CAR T cells that have been reprogrammed to target CD19 and CD22 proteins simultaneously. CD19 and CD22 are expressed by most leukemia cells.
Seattle Children’s researchers developed PLAT-05 as an investigational treatment option that will hopefully lead to long-term remission for patients whose cancer expresses CD19 and CD22.
Beare was deeply disappointed Harper hadn’t achieved remission with conventional chemotherapy, but she was confident this treatment was the best option for her daughter.
“I told myself, this is a trial, so Harper gets to be a part of saving so many other lives. It was a big perspective shift for me. I realized Harper was going to do something amazing,” she said.
Shining through treatment
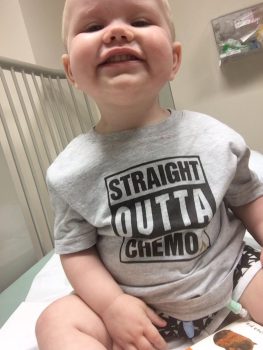 Harper’s T cells were removed in April through apheresis — a process in which blood is removed by a machine that separates the liquid part of blood from the blood cells. White blood cells are collected while the rest of the cells are returned to the patient along with their blood plasma.
Harper’s T cells were removed in April through apheresis — a process in which blood is removed by a machine that separates the liquid part of blood from the blood cells. White blood cells are collected while the rest of the cells are returned to the patient along with their blood plasma.
The cells were then engineered to express a certain CAR on the surface of the cell. The CAR is like a puzzle piece that’s designed to attach perfectly to a specific antigen or marker on the surface of the cancer cell. When they attach, the T cells attack the cancer cells as if they were fighting an infection.
Harper’s newly reprogrammed T cells were grown to multiply into billions of new cells and infused into her in May. She was in the hospital for a week, with a couple days of fevers, before she was released.
“Harper handled the therapy very well and recovered beautifully. It was as benign a course as anyone could have.”
“Look how far we’ve come”
On June 12, Beare received good news. Ten months after her initial diagnosis, Harper was finally in remission.
“I started sobbing,” Beare said. “It was the best news ever. It felt like the day she was born. The past 10 months flashed before my eyes and I thought, ‘Wow, look how far we’ve come.’”
The first thing Beare did after hearing the good news was call another mother whose young son was receiving his T cells that same day.
“I just cried ‘It works! It works!’” she said.
For Seattle Children’s providers, this is easily the best part of the job.
“Every time I get to walk into a room and tell a kid, ‘You’re in remission,’ it’s the most amazing feeling. It never gets old. It’s an incredible honor to deliver that news to families who have been through so much.”
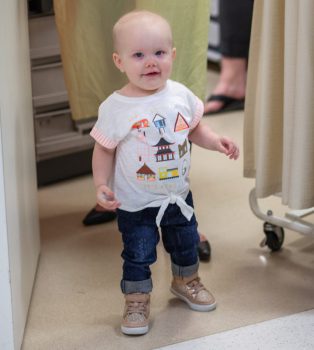
A few weeks later, Harper was thriving.
“She is running, fast!” Beare said. “She is getting into stuff and doing toddler things. She has a massive vocabulary and her hair is coming in. Essentially, she is a normal kid but with 20 times the energy! It’s so nice to finally get to experience what normal toddlers are like.”
But Harper’s cancer journey was not over. To ensure she remained in remission, she underwent a bone marrow transplant on Aug. 7.
So far, Harper has handled the treatment well. Beare is hoping they will return home by Thanksgiving.
“Harper is something special, and I’m not just saying that because she’s my kid,” Beare said. “She adapts, she is resilient, and I have no doubt she is going to get through transplant and have an amazing life.”
 “Some researchers have suggested CAR T cell therapy is more difficult to administer to infants than older kids or adults, but that has not been our experience. We are just as capable at giving infants T cells, and Harper embodies that beautifully. I believe she will remain in remission long-term and there is a really good chance her cancer will never come back.”
“Some researchers have suggested CAR T cell therapy is more difficult to administer to infants than older kids or adults, but that has not been our experience. We are just as capable at giving infants T cells, and Harper embodies that beautifully. I believe she will remain in remission long-term and there is a really good chance her cancer will never come back.”
Seattle Children’s is dedicated to improving CAR T-cell immunotherapy for a variety of childhood cancers to the point that it helps patients achieve long-term remission – and ultimately – a cure. For more information about these trials, please call (206) 987-2106 or email [email protected].
If you are interested in supporting the advancement of immunotherapy and cancer research at Seattle Children’s, please visit our donation page.

